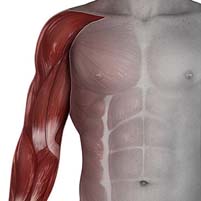
Pain, numbness, burning, tingling, stabbing or shooting sensations into your arm and shoulder blade could be a brachial plexus injury. Even though the cause is often a pinched nerve in your neck, many patients come in with severe arm symptoms, without neck pain. An injury to the brachial plexus can also cause weakness of your arm, right down to your hand.
What is the Brachial Plexus?
The brachial plexus is the neural network of your arms, one plexus on each side. A nerve root is the part where the nerve exits the spinal cord, and your brachial plexus consists of nerve roots from levels C5 to T1. These five nerve roots merge and divert to form the brachial plexus. A plexus is like a train station, where a lot of different routes come together and then split apart again. The brachial plexus splits to form three peripheral nerves that supply the entire arm. These are the median-, radial- and ulnar nerves.
Why is the Brachial Plexus so important?
Nerves are like power cables within our bodies. They supply “electricity” to allow our muscles to move, carrying messages to and from your brain via the spinal cord. These electrical impulses travel in both directions. Messages from the brain to your arm will travel to the muscles and joints, resulting in muscle contraction and movement. The return route from your arm back to the brain is a complicated network of nerves, carrying information from the periphery (fingers and toes) to your brain. If there’s an disturbance in this network, the messages can either not get to their destination, or the message becomes “distorted” somewhere along the way. You will experience this as either weakness, numbness, pain, pins and needles or a combination.
I have a Brachial Plexus injury – How did it happen?
Any trauma to the brachial plexus can cause injury to the nerves. Trauma includes compression/pressure, traction/stretching or severing/ripping apart. The most common brachial plexus injury is due to traction or stretching. The severity of the symptoms will be determined by what happened (traction, compression or severing) to which part of the plexus.
The upper part of the plexus (nerve roots C5 & C6) can be injured when your head is forced away from your shoulder, like a whiplash or rugby tackle. This also happens when you fall directly on the shoulder, and your head bends in the opposite direction.
The lower part of the brachial plexus (nerve roots C8 & T1) will be injured when your arm is forced above your head. This can happen if you slip while climbing and then grab hold of a rock or tree branch. The weight of your body jerks through your shoulder to your neck. A sudden hard pull on your arm, or even repetitive overstretching over time can also injure this part of the brachial plexus.
Causes of Brachial Plexus injuries
Compression injuries
- Tumors
- Inflammation
- Prolonged position which leads to decreased blood flow to the nerves
Traction injuries
- Fall
- Birth injury
- Contact sport (rugby scrum or tackle)
- Motor vehicle accidents
Severing injuries
- Knife wound
- Gunshot
How severe is my Brachial Plexus injury?
Neuropraxia (nerve compression)
Let’s say you had a memorable night out and “slept” hugging the loo, your brachial plexus is compressed for the duration of your nap. This causes damage to the rubber lining (myelin sheath) around the axon, due to a decrease in blood supply. Luckily the axon is intact. This is the least severe injury and will recover fully within 6 weeks. There is temporary loss of movement and sensation.
Axonotmesis
When the power cable (axon) and the rubber lining (myelin sheath) are damaged, it may lead to paralysis and sensory loss. Axonotmesis can heal but takes time. The nerve regenerates at an extremely slow pace. You will need patience because healing may take up to 2 years. This can happen due to a severe traction injury which less to bleeding around the nerve.
Neurotmesis
Neurotmesis is complete severing of the nerve, and the most severe injury. This can happen with a very severe traction injury, gunshot wound or knife stab. When the nerve is severed your pain may be minimal, but you will have no sensation or movement. Recovery is very slow with the potential of permanent damage. Surgical management is necessary to bridge the gap between the nerve endings.
Diagnosis
Physiotherapy diagnosis
We assess the function of your nerves by testing your sensation, power and reflexes. We also test the nerve’s sensitivity to movement with neurodynamic tests. These tests allow us to determine the severity of your injury and also the affected levels. If you need to consult with a specialist we are able to send you in the right direction. Different tests are used for all the different structures, so your individual case will determine which tests to do.
X-rays
After a traumatic injury like a fall or car accident, X-rays are indicated to assess bony integrity i.e. rule out fractures. However, nerves are not visible on an X-ray image, so this test is not useful for diagnosing nerve injuries,
Diagnostic ultrasound
With a sonar we can see the more superficial parts of the nerve and any possible areas of compression.
Nerve conduction study
A neurologist performs a nerve conduction study to assess the function of the nerve. This is a painful procedure. Needles are inserted and electrical impulses are sent through the nerve.
MRI
With a MRI we can see the nerves, bones and discs. This is a costly test that can only be ordered by a specialist, but isn’t always necessary to diagnose nerve injuries.
Why is the pain not going away?
In the case of a minor injury, that may have happened a few months or years ago, you may experience flare ups of pain with no cause. This is most commonly due to protective muscle spasm around the injured nerves which restricts the nerve’s ability to move and glide freely. Let us help you to work on this restriction and encourage, happy, pliable nervous structures in your arm.
Problems we see when patients come to us with Brachial Plexus injuries
Muscle Atrophy
Without normal nerve supply/innervation, muscles will begin to waste away within weeks. If left untreated, the muscle tissue undergoes permanent structural changes.
Joint Contractures
Nerve injuries cause muscle weakness or paralysis, so the joints of your arm will lose range of movement. This causes stiffness and shortening of the joint capsules and tendons and eventually, permanent loss of mobility.
Shoulder Instability
Weakness in your shoulder muscles, due to the brachial plexus injury, can lead to instability and abnormal movement patterns of your shoulder.
“Claw Hand” Deformity
If the lower part of the brachial plexus is injured, the small muscles in your hand will be affected. These muscles weaken and atrophy, leading to hyperextension of the knuckles and curling of the fingers.
Edema and Circulation problems
Muscle weakness and atrophy means a loss of the “muscle pump” effect, in other words the mechanism your body uses to return blood to the heart. The result is poor circulation leading to swelling and poor temperature regulation.
Physiotherapy treatment
Physiotherapists are experts when it comes to diagnosing and treating nerve injuries. Treatment is focused on pain relief and supporting the healing process of your injured nerves. Modalities include nerve mobilization, myofascial release and dry needling, electrotherapy and strapping, to treat protective muscle spasm, relieve pain, and encourage pain free movement.
Phases of rehabilitation
1st Phase: Protection & Pain relief (week 1-2)
During this initial phase of treatment we will use gentle joint mobilizations, nerve mobilizations and electrotherapy for pain relief. Strapping is useful to take some of the strain off the painful nerves. Even with the right treatment, it can take up to a week to get pain relief, so an important part of this phase is education and guiding you through the process. We will give you advice about positioning, what you can do at home and what to avoid.
By the end of this phase your pain should be at a manageable level and you should be able to use your arm for small daily tasks.
2nd Phase: Early range of motion (week 2)
Once your pain has settled, we start using treatment techniques to get movement back. These include joint mobilization, myofascial release and nerve mobilization. We will still use electrotherapy, like laser and ultrasound, for pain relief. This phase starts to incorporate gentle range of movement exercises to encourage healing and restore normal movement of your arm.
By the end of this phase of treatment, you should have enough mobility for daily tasks. You should also be able to find a position where you have minimal pain.
3rd Phase: Muscle activation and motor control (week 3-4)
When you reach phase 3 of treatment, your pain should be under control. Now we shift our focus to muscle activation and motor control. When we have pain, our deep stabilizing muscles lose their normal function. Unfortunately, this function doesn’t just switch on again when the pain is gone. Motor control exercises target these small muscles. Initially, we will start exercises in easy positions like lying flat, and progress to sitting and adding movement.
By the end of this phase, you should know how to activate the small muscles around your neck and shoulder. You should also be able to work at your computer or desk for about 30-45 minutes at a time before needing a break.
4th Phase: Strengthening (Week 4 – 6)
After we’ve addressed the motor control and muscle activation around your neck and shoulder, we can start with the resistance exercises. Resistance exercises are important to regain muscle strength around the injured area. Not only is it crucial for healing, it’s also an important part of long-term management for nerve injuries. To add resistance, we will use elastic bands, bodyweight and dumbbells. As you get stronger and regain full movement of your arm, resistance will increase over time to make sure the nerve adapts to extra load.
At the end of phase 4, you should have no pain, be sleeping through the night and have full range of movement. You should also be able to perform all you normal daily tasks without effort.
5th Phase: Clearance phase (Week 6 – 8)
In this final phase of treatment, we test and load your brachial plexus to assess healing. The difficulty of your exercises will increase to get you back to normal activities and we will also add nerve gliding exercises to maintain the restored movement.
By the end of this stage, you will have a home exercise program according to your level of activity before the injury. You should have full range of movement of your neck and arm, no pain with activity and almost normal strength of your injured arm.
Healing time
Your recovery time will depend on the extent of your injury and how your respond to rehabilitation. Nerves take a long time to heal, and this process often takes 6-8 weeks of non-surgical treatment. A completely severed nerve can take up to 12 – 18 months of rehabilitation after surgical management.
During the first phase of treatment, you will have two physiotherapy sessions per week. In the next phase, we will see you once a week for the following two weeks. Thereafter, sessions will be spaced out about 10 days to two weeks apart, depending on your progress.
Other forms of treatment
- General practitioner/Doctor – medication for pain relief and to decrease neurogenic inflammation around the nerves.
- Soft collar (neck brace) – not always necessary, but may help relieve pressure on the muscles and nerves in your neck.
- Shoulder sling – may help to decrease tension on your neck and shoulder.
- Orthotist – can supply a neck brace or shoulder sling, if necessary.
- Chiropractic – strong techniques used by chiropractors may increase irritation to the nerve.
Is surgery an option?
When the nerve is severed, surgical management will be necessary. A neurosurgeon will determine the appropriate surgical option. In the case of a severed nerve, the surgeon will reconnect the ends of the nerve. If scar tissue is compressing the nerve, causing damage, a neurolysis is performed. Rehabilitation is crucial after surgery to protect the healing nerve, restore nerve function and range of movement. There is no shortcut to recovery, but your physiotherapist will be with you every step of the way.
What else could it be?
- Cervical radiculopathy – whole arm is not affected, only a specific nerve root.
- Peripheral nerve injury of the median, radial or ulnar nerve – nerve symptoms mostly in the forearm and hand.
- Thoracic outlet syndrome – will also present with other symptoms, like changes in temperature or skin color.
Also known as
- Parsonage Turner syndrome
- Stinger
- Burner
- Brachial plexus lesion