A Lateral ankle sprain is the most common sports-related injury that physiotherapists see. This is also the most widespread type of ankle sprain in non-athletes. An ankle sprain happens when you injure one or more of the ligaments around your ankle. Almost 85% of these sprains are lateral ankle sprains, where one of the three outside ligaments of the ankle is partially or completely torn. The biggest problem with this type of injury is that about half of the people with an ankle ligament sprain will choose the “wait and see” approach and not seek any treatment. Unfortunately, without assessment and management by a health professional, many of those will end up with chronic ankle instability (CAI).
The Anatomy of your Ankle joint
In anatomical terms, a joint is anywhere two or more bones meet. The top part of your ankle joint is formed by the two bones in your lower leg, also known as your shin. These are the thick, weight-bearing tibia on the inside and the thin, non weight-bearing fibula on the outside.
The talocrural joint (true ankle joint)
This is the joint between the lower parts of the tibia and fibula and one of the bones in your foot, namely the talus. The joint is a typical hinge joint that moves up and down. The up movement, when you lift your toes in the direction of your nose, is called dorsiflexion. Plantarflexion is the opposite movement, where you point your toes like a ballerina.
Inferior tibiofibular joint (bottom shin bones joint)
Another important joint at ankle level is where the lower parts of the tibia and fibula meet, basically forming part of the roof of your ankle joint. The inferior tibiofibular joint has very limited movement, but stiffness in this joint will result in pain during walking, climbing stairs, and running.
Subtalar joint (shock absorbing joint)
This is the joint between your talus (top foot bone) and heel bone (calcaneus). The subtalar joint changes the position of the back part of your foot, helping you to keep your foot flat, which means you can keep your balance on uneven surfaces. Movements at this joint are inversion, where the sole of your foot turns inwards, and eversion, which is then your sole turns outwards.
Ligaments
Keeping these joints stable and limiting movement, we will find various ligaments. The ligaments on the outside of your foot are the anterior talo-fibular ligament (ATFL), the calcaneo-fibular ligament (CFL) and the posterior talo-fibular ligament (PTFL). The deltoid ligament can be found on the inside of your ankle and is much stronger than the lateral ligaments.
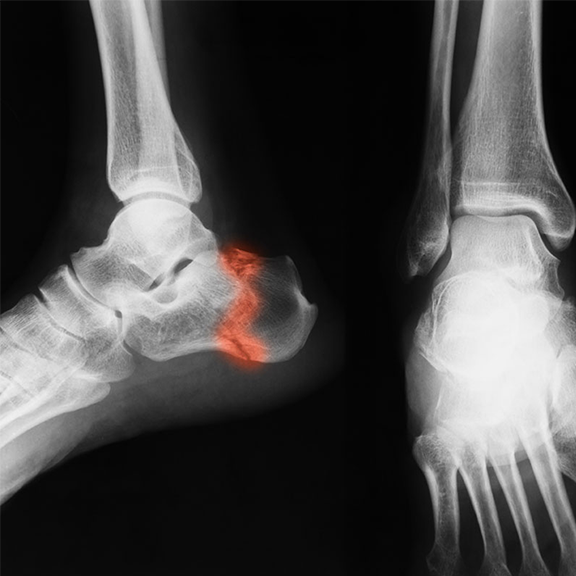
Why are ankle ligaments important?
Ligaments are made of collagen fibres which act like cables holding up a bridge. The ligaments in your ankle are crucial for static stability, in other words preventing excessive movement, and proprioception. Proprioception is your brain’s awareness of the position of your body and is often the missing link when it comes to recurring ankle sprains. Without this body awareness, you will find that you have trouble keeping your ankle from rolling when you stumble, walk on uneven surfaces, or land awkwardly from a jump.
ATFL
The anterior talo-fibular ligament (ATFL) is by far the most commonly injured ankle ligament. It is a flat, thin band at the front of the outside part of your ankle. It keeps your ankle from sliding forward and is damaged when you roll your ankle when your toes are pointed to the ground, i.e. in plantarflexion.
CFL
The calcaneo-fibular ligament (CFL) is cord-like and in between the other two ligaments on the outside of your ankle. It is often injured with the AFTL when you roll your ankle with pointed toes. When you roll your ankle with a flat foot, this will be the first ligament you damage.
PTFL
The posterior talofibular ligaments (PTFL) is a very short ligament right at the back of your ankle. This ligament can be injured with the CFL when you roll your ankle on a flat foot.
I have an ankle sprain. What happened?
A sudden twist will damage your ankle ligaments. This twisting movement stretches the ligaments beyond what they can withstand, so the fibres start to tear or fray like a rope. The most common ankle sprain we see is when the ankle rolls inwards, in other words, the sole of your foot faces turn in towards the other foot. This is also known as an inversion sprain, which injures one or more of the ligaments on the outside of your ankle. The opposite movement, or an eversion sprain, will damage the deltoid ligament on the inside of your ankle. This injury is much less common, and is often found in combination with a fracture.
Most people think a torn ligament means complete rupture, like an elastic that snaps. Fortunately, the majority of ankle sprains are not complete ruptures. Ligament injuries are graded, based on severity. You might find that medical professionals will alternate between the words sprain and tear. That’s because the grading is based on how many fibres are torn. For instance, a complete rupture or grade 3 tear, means that all the fibres are torn. In the case of grade 1 or 2 tears, there are still pieces connected.
Causes of Ankle sprains
Studies have shown that 40% of traumatic injuries to the ligament happens during sport. Your ankle also becomes more vulnerable as the distance from the floor increases. That’s why women are more likely to injure their ankle ligaments if they wear high heels. Other common causes include
- Walking, Jogging or Running, especially on uneven or unstable surfaces
- Jumping landing or exercising on uneven or slippery surfaces
- Falling or getting your foot caught by an object on the floor, like a rug or a step
- Cutting sports that require complex foot movements, such as rugby, hockey, netball or soccer
- Contact injuries during a sport where someone else may step or fall on your foot.
Ankles get injured often, and at first it might only be a minor sprain. Unfortunately, the more this happens, the ligaments will start to get a repetitive strain injury. The ligament loses tension and becomes more lax, until your ankle is chronically unstable or the ligament tears completely.

How bad is my ankle sprain?
Grade 1
This involves some minor tearing of the ligament. You will have little or no instability, mild pain and some swelling on the outside of the ankle. There may be very little stiffness and a slight limp when you walk. The ligament is intact enough to limit movement at your ankle joint, so you might even feel able to walk it off and get back to your normal activities after a few days. The bad news is that ankle sprains tend to happen again after the first one.
Grade 2
With a grade 2 ligament injury, a moderate amount of fibres are torn, but at least 80% of the ligament is still intact. You will feel a bit unstable or unbalanced when you walk and slow down significantly when you get to steps. After a grade 2 ankle sprain, you will definitely be aware of pain and swelling. Your ankle will feel stiff and tight, especially after sitting still for awhile or when getting up in the morning. Walking normally will be very challenging, so you will walk with a noticeable limp, trying to keep your weight off the injured ankle. There might not be bruising immediately after injury, but you will notice bruising and discolouration on the outside of your foot and ankle within 24-48 hours after the sprain. Whereas the limp improves quite quickly with a grade 1 sprain, you’ll still be limping quite a bit the week after a grade 2 ankle sprain.
Grade 3
A grade 3 ligament sprain is where there’s total rupture of the ligament or more than 80% of the fibres are torn. Severe swelling and bleeding are signs that something needs to be done as soon as possible. Your ankle will feel unstable and you will be very hesitant to take weight on it. In some cases there may be no pain if all the fibres are torn, but in most cases the pain is excruciating. Walking will be agonizing and you won’t even be able to walk with a limp. Swelling and bruising will be severe and can be mistaken for a fractured ankle. Not all Grade 3 ankle ligament injuries require surgery, but some do! The best thing you can do is to seek help from a medical professional as soon as possible.
Diagnosis
Physiotherapists are experts when it comes to diagnosing and managing ankle sprains. This is an extremely common injury, so we have hands-on experience when it comes to treating painful ankles. First, we determine the area and severity by performing stability tests. These tests involve applying tension to the ligament fibres. We test the different ligaments in the ankle by stressing each one individually using its direction of pull. This can give us a clear picture of how many of the ligaments are injured and to what extent.
Even though the main indication is a ligament sprain, our assessment will always cover the ankle as a whole. Damage to tendons, bones and other joint tissues in addition to ligament damage is typical. Quite often fractures of the smaller foot bones are missed. Especially when an ankle sprain happens when landing on the twisted ankle from a step or height. A physiotherapist must look at the whole foot and ankle structure to determine how many structures are involved in the injury.
After we have performed clinical tests, we will determine what, if any, other tests we should refer you for. However, these tests are not always indicated and, if they are, the timing is important. In many cases having extra tests done too soon after injury will not give accurate results. Your physiotherapist can guide you on the correct course of action.

X-rays
Your Physiotherapist will determine if it’s necessary to take X-rays to exclude fractures of the Tibia, Fibula or Tarsal bones. If your sprain is more severe, you may need X-rays to determine if there are any broken bones (fractures) or bones that have moved out of position (subluxation).
X-rays in children are more frequent due to a potential injury to the bone’s growth plate can disrupt the healthy growth of the bone. X-rays of both ankles will show the comparison between the two sides so that they can compare the injured ankle with a healthy one. If so few injuries have fractures why bother to take x-rays at all?
Diagnostic ultrasound
A sonar is the first choice to determine if and the extent of ankle ligament damage. This, however, becomes very difficult if the ankle is already very swollen. That is why it is usually better to reduce the swelling first before going for a sonar.
The sonar will show superficial soft tissue and the top layer of the bones, but it is not the best way to exclude a fracture. We are sometimes able to see a fracture if it is right at the top or if the ligament pulls a piece of bone from its attachment (avulsion fracture).
MRI
An MRI is a very expensive scan which can only be referred by a specialist and in the ankle, it is an orthopaedic surgeon. This is the scan of choice if there is underlying pathology in the ankle joint that was not picked up by X-ray or sonar. This can show us all the soft tissues and often will be able to show us if there is any problem inside the ankle joint itself.
Why is the pain not going away?
The most likely reasons are that a fracture has been missed or you have developed Chronic Ankle Instability (CAI). Research shows 30% of people can develop CAI. Causes have been linked to a delayed muscle reflex, poor stability of lower leg muscles, poor lower leg muscle strength, and impaired postural control. That is why we address all these aspects in your rehabilitation program after an ankle sprain.
The most common fracture missed is in the midfoot (foot bones) or an avulsion fracture where a piece of bone pulls away from the insertion of the ligament on the bone. Initially missing the fracture, the recommendation is to do an X-ray after six weeks. Above all, the second x-ray can show where bone healing took place.
One condition which is often missed is a syndesmosis injury or high ankle sprain. This is a serious ankle injury where the ligament and membrane holding the two shin bones together tears. These structures are responsible for keeping the bottom ends of the two shin bones together. If it’s torn, the ankle becomes very unstable. Furthermore, it has a poor healing rate which can result in chronic ankle instability.
Problems we see when patients come to us with torn ankle ligaments
Undetected ligament tears with ankle sprains
Depending on your local emergency room, your suspected “ankle fracture” may be low on the priority scale. If the x-ray shows no fracture, you will probably be sent home with no further treatment. Unfortunately, an X-ray doesn’t rule out ligament tears. Walking around with torn ankle ligaments, you will quickly realize that the swelling and pain won’t go away on its own. By the time patients see us to assess their sore, swollen ankle, there is already weakness of the surrounding muscles and stiffness of the ankle joint.
Incomplete rehabilitation
It’s important to complete a rehabilitation program because it makes it less likely that you’ll hurt the same ankle ligaments again. If you don’t complete rehabilitation, you could suffer constant pain, instability and post-traumatic arthritis in your ankle joints. If your ankle still hurts, the sprained ligament has not healed completely. On the other hand, the diagnosis might be incomplete or wrong.
You don’t want to go through this whole process over and over again, just to re-injure it. Unfortunately, this is exactly what we see every day as most people think it is just a minor sprain. The cases of Chronic Ankle Instability (CAI) is increasing and it is preventable. Prevention is definitely better than cure when it comes to ankles!
Chronic Ankle Instability
This is most often the problem with ankle injuries, the more often the ligaments get injured, the worse they get at their job and the more we get injured. Chronic ankle ligament injuries are very common. Research has shown us that between 1-4 years after an injury: 5-46% of people still have some pain, 3-34% have re-injury, and 33-55% of people report their ankle feels unstable.
Incorrect movement patterns
Your body will help you compensate for the slight ligament injury. This is because an injury affects more than the joint which it is supposed to protect. Ligament injuries change the way you walk or run. This compensation pattern can cause you to re-injure the same ligaments and keep getting the same problem. Rather seek help from experts before these movement patterns catch up with you.

The pain isn’t too bad – is it okay to walk around on my sprained ankle?
Well, no. The ligaments around your ankle keep the joint stable. If these ligaments are partially or completely torn, the increased tension during walking can overload the already injured ligaments. Apart from that, your tibia and fibula will slide forward and backward without the support of the ankle ligaments. Please do not make the injury worse, rather let a medical professional take a look.

Physiotherapy treatment for a sprained ankle
Physiotherapists determine the ligaments that are partially or completely torn and explain what to do in the first 72 hours after treatment. We also start treating pain, stiffness and swelling at the first session and use strapping or taping to protect the injured ligaments. If you have more than one torn ligament or a grade 3 tear, we will advise you on how to use the moon boot and crutches. Early movement has been shown to help with healing after an ankle sprain, but should be done under the supervision of a medical professional.
When a physio oversees your recovery, you will be able to walk without the moon boot at week 6, not only start taking the boot off.
Phases of rehabilitation: Grade 1 and 2 ligament tears
Phase 1 – first 72 hours
This phase is all about protecting the injured ligaments. We have various techniques to get the job done, like taping, splinting or a brace to prevent excessive movement. Treatment for pain relief will also start during the first session, including electrotherapy like laser or ultrasound, and gentle soft tissue mobilization. Crutches will help you to get around without putting weight on your ankle which reduces pain and inflammation, supporting the healing process.
At the end of phase 1 your pain should be manageable and you should be able to walk comfortably with crutches. With a grade 1 tear, you should be able to take weight on your foot during walking.
Phase 2 – day 3 to week 2
After phase 1, our focus will also include mobility while we still address pain and protecting the healing ligaments. We will start early scar tissue mobilization to prevent thickening of the ligament which can cause complications later on. Once the swelling and pain are under control, we will start adding joint mobilization, myofascial release, neural mobility and gentle exercises to improve mobility and stiffness.
At the end of this phase of treatment, you should be walking normally (grade 3 tears will still be in the moon boot and walking with crutches) with minimal pain. Swelling should also be minimal and range of movement will be at least 50% of the uninjured side.
Phase 3 – weeks 2 – 4
We will guide you when it’s safe to start putting weight on your ankle, remove the moon boot and start walking short distances. Grade 1 ligament tears will start specific functional exercises to restore full range of movement and start strengthening the muscles around your ankle. Once you can take full weight on your ankle again, your exercises will become more challenging to improve your flexibility, balance and coordination.
At the end of phase 3 you should have full range of movement and almost no pain or swelling. For a grade 1 tear, you should be walking normally without support by now. You should also be able to go for a short, easy jog by the end of this phase (grade 1 tear). Grade 2 tears will usually progress to a speed brace at the end of this phase, but grade 3 tears will still be in the moon boot until week 6.
Phase 4 – weeks 4 – 8
By now, grade 1 ligament tears should be jogging and start with jumping and hopping drills. Balance should be equal to the uninjured side and you should have no pain, stiffness of swelling. To prevent future sprained ankles, this phase will include more advanced exercises to strengthen your leg muscles, and keep your ankle joint stable.
A grade 3 tear will start supervised exercise out of the moon boot and walking short distances on a flat, stable surface. We will also start the same exercise program that grade 1 tears started during the previous phase.
At the end of this phase, grade 2 tears should be walking normally, jogging, hopping and jumping. They should also have full range of movement, no pain and know the warning signs of when they have done too much.
Grade 3 ligament tears – non-surgical management
These injuries will follow the same phases of rehabilitation, but all phases will be about 4 weeks later than grade 1 and 2 tears. Progression will depend on symptoms and severity of the initial injury. Your physiotherapist is an expert in monitoring progress and adapting your rehabilitation program to your problem.
When is it safe to get active again after an ankle sprain?
Uncomplicated grade 1 injuries take between 2-4 weeks to heal. However, if more ligaments or other structures are also injured the healing time will be longer, depending on the individual tissue injured. Grade 2 injuries without damage to the other tissue around your ankle will take between 4-8 weeks to heal. Recovery of grade 3 injuries will depend on the management. Non-surgical management will be 12-14 weeks with the first 4-6 weeks in a moonboot.
In the first phase of treatment we will see you twice a week for pain management, education on how to protect your ankle and treating stiffness and swelling. From week 2 we will see you once a week and start with mobility and strengthening exercises. Depending on your progress, we will probably see you every second week from week 4 and then once a month until you can successfully perform clearance tests.
Other forms of treatment
- General practitioner to prescribe pain medication if necessary. Anti-inflammatory medication is not recommended in the first 48 hours after injury, as this can delay healing.
- Moonboot to protect the injured ligaments and prevent excessive movement.
- Crutches are useful to take the weight of your injured ankle. This helps with pain relief and also protects the injured ankle to support healing.
- Stretch therapy is not recommended because any tension on the already fragile ligament will either cause further injury or delay healing.
- Chiropractic adjustments is unnecessary after an ankle sprain and should probably be avoided.
- Speed brace, or ankle brace, after the moon boot or in the first weeks after you return to sport.
Is surgery an option?
Complex or unstable grade 3 ankle ligament tears may require surgical management. The procedure will depend on the ligaments injured and degree of instability. With complex ankle injuries, there may be fractures of the foot bones or torn ligaments between the small bones in your foot. In some cases, the ligaments don’t reattach because the torn ends of the ligament are too far apart. Syndesmosis injuries are usually surgically repaired to prevent future instability and complications.
After surgery, your ankle will be immobilized for 4-6 weeks (depending on the orthopedic surgeon) and the rehabilitation process thereafter are almost identical to that of non-surgical management.
What else could it be?
Less common injuries excluded from the differential diagnosis include:
- Ankle pain
- Ankle fracture (medial/lateral malleolus, distal tibia/fibular)
- Damage to the medial ligament (deltoid)
- Dislocated ankle
- Sinus Tarsi Syndrome
- Other soft tissue damage e.g. muscle strain
- Anterior ankle Impingement
- Tarsal Tunnel Syndrome
- Cartilage or osteochondral lesions
- Peroneal Tendinopathy
- Posterior Tibial Tendon Dysfunction
Also known as
- Torn ankle ligaments
- Twisted ankle
- Ankle strain
- Rolled ankle

