Is lower back pain and discomfort taking the excitement out of your pregnancy? Things that you used to do without thinking about it being effort, like putting on your shoes, getting out of your car or simply carrying groceries.
Pregnancy-related lower back pain is extremely common and occurs in up to 70% of pregnancies. It usually starts at around 18 weeks, but onset can even be as early as 6 weeks into your pregnancy. Even so, you don’t have to lie awake at night hoping the pain will go away. A physiotherapist can help you find relief for your sore back.
Don’t let back pain stand in your way! There are so many things to do and to get ready for, before the baby’s due date arrives. Rather call us to help you get answers and to find relief.
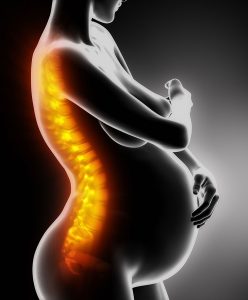
Some background on your lower back and pelvis
Your lower back or lumbar spine is made up of 5 vertebrae, intervertebral discs and various ligaments and muscles. Just below your lumbar spine is your sacrum. This bone, that looks like an upside down triangle, is part of your pelvic girdle and links your upper body to your legs. The other bones that make up the rest of your pelvis are called the ilium (or “hip” bone), ischium (or sitting bone) and pubis.
Your lumbar vertebrae and pelvis give your lower back bony stability, but what about movement?
Imagine jumping off a low wall and keeping your legs rigid and straight. When your feet hit the ground you will feel the shockwave all the way up to your ears. That’s one of the reasons your lower back needs to allow some movement – for shock absorption. Allowing movement means that your lower back needs to sacrifice some stability. The more movement there is, the less stability you will have. Unless there’s another system to make up for this decrease in stability. This is where your muscles and ligaments come in.
The effect on your Muscles and Ligaments during Pregnancy.
Firstly, muscles in and around your lower back contract (shorten) and lengthen to make movement possible. It not only makes movement possible, but it also controls the movements, keeps you from losing your balance and keeps you upright. Reaching up for something on a shelf or getting up after putting on your shoes are only possible because you have muscles in your lower back. Some of these muscles also cross your hip joint linking your upper body and your legs. If your pelvis is stable this link allows movement of your legs for walking, climbing steps, running and jumping.
Secondly, ligaments provide stability to stop too much movement of a joint. An everyday example of a joint will be something like the hinge in a car door. The hinge allows a certain amount of movement to let the door open and close. It only stops the movement if the door opens too much to prevent damage. In the same way, ligaments in your lower back allow you to bend forwards, backwards and side to side, but will stop you from going too far and straining the joints. Many of these ligaments connect your lumbar spine to your pelvis and also connect the different bones of your pelvis to each other. In contrast to your lower back, your pelvis has minimal movement because its main purpose is to support your upper body and create a stable attachment for your hip and thigh muscles.
Unfortunately, your body’s need for pelvic stability is exactly why lower back pain is so common during pregnancy.
Your body undergoes a lot of changes during pregnancy to prepare for childbirth. Hormones fluctuate, you retain water and even the shape of your body changes. These hormonal changes don’t only cause nausea, mood swings and cravings, though. One of these hormones, called relaxin, causes changes in your connective tissue specifically causing ligament laxity. This means that your ligaments allow more movement in your pelvis to eventually allow for childbirth. Before that time comes, though, this laxity also results in less stability in your lower back and pelvis that could lead to lower back pain.
Is that all?
In addition to your changing hormones, there are also more obvious changes to your body that can contribute to your lower back pain.
As your baby grows, you will find that your center of gravity moves forwards, becoming more pronounced as your baby bump gets bigger. Over time you will gradually start leaning backwards to keep your balance. This change in posture increases stress and strain on your lower back due to the increased curvature or lordosis.
In most cases, women will gain 11-15kg during their pregnancy. This weight gain also adds extra strain on your lower back and shifts your center of gravity even more. Extra stress on the structures in your lower back can lead to inflammation. Inflammation leads to pain which results in muscle spasm as your body tries to protect you and decrease the tension on your lower back.
Another effect of this weight gain is that your abdominal muscles have to stretch as your uterus expands with your growing baby. These muscles play an important part in your posture and the stability of your lower back. The more your abdominal muscles stretch, the harder they have to work to stabilize your back. Eventually the muscles will be so weak and stretched out that your body will have to look for stability elsewhere. The work usually shifts to your lower back and buttock muscles that are already overworked due to the ligament laxity caused by your changing hormones.
How bad is it?
When your lower back pain starts you notice a dull discomfort at first. The discomfort comes and goes, but doesn’t really interfere with your day. You can still finish all your chores around the house, get out of bed easily and sleep like a baby. In the morning you have some stiffness in your lower back, but nothing that a bit of a stretch can’t get rid of.
As the problem gets worse your pain is there more often than not. Lying down gives you some relief, but it doesn’t last long. When you get up to carry on with your day your lower back pain is right there waiting for you. Your pain starts to spread to your buttock area and sitting for more than 30 minutes is unbearable. The only thing worse than sitting is standing for the same period of time. Stretching helps for your morning stiffness, but only for a couple of minutes. This stiffness then stays with you until you go back to bed at night.
If you don’t pay attention, the problem gets even worse until you have a constant dull pain in your lower back. This is accompanied by a stabbing pain in your buttock, especially climbing stairs or twisting to get in your car. Pain even starts to spread down the back of your thighs at this point. Standing, sitting and walking are excruciating and you might not be able to face a flight of stairs. Even lying down at night doesn’t bring you any relief, even though you are exhausted after a long day of struggling with your lower back pain.
Diagnosing pregnancy-related back pain
Physiotherapy diagnosis
Our physiotherapists are experts in human anatomy and physiology. We listen to your story and know which questions to ask to get the full picture of your problem. During the physical assessment we will do movement tests, muscle length tests, test the nerves in the area and apply pressure to different parts of your lower back. The combination of tests and the information you give your physiotherapist will allow us to accurately diagnose and treat your lower back pain.
X-rays
X-rays of your lower back are not recommended during pregnancy, so this test should not be used to find the cause of your pain.
MRI
An MRI will show the deeper structures in your lower back, but unnecessary imaging should be avoided during pregnancy. Consequently, this test will only be used to diagnose your lower back pain in extremely rare cases if recommended by a surgeon.
I’ve been resting often, so why isn’t the pain in my lower back going away?
Once you develop lower back pain it will tend to get worse as your pregnancy progresses. As your baby grows, you will start gaining weight which puts more strain on your lower back. Especially because most of this weight will be over your abdomen. This extra weight will increase the curvature of your spine, putting even more strain on all the structures in your lower back.
Another reason that your pain doesn’t go away in spite of any resting and stretching you may do is the increased laxity of your ligaments. Your hormone levels will keep on changing with each week of your pregnancy. On the one hand this laxity is an important part of preparing for the birth of your baby. On the other hand, though, your lower back depends on these ligaments for static stability. As the laxity increases, this stability will decrease. The resulting muscle spasm in your lower back is your body’s attempt to get some of this stability back. However, muscle spasms will inevitably lead to further back pain and stiffness.
Make sure you get the right treatment before your lower back pain starts to take away the joy and excitement of your pregnancy.
Problems we see when patients come to us with lower back pain during pregnancy
Waiting too long to get help
Lower back pain might start suddenly during your pregnancy, but it won’t go away in the same way. As your body changes you will find that your back pain and muscle spasm only gets worse if you carry on like before. The longer you wait to get help, the longer it will take to get rid of the problem.
Jumping between treatment options
Another problem we see is that someone with back pain will go for one treatment and give up if the pain doesn’t go away immediately. This leads to a jump to another kind of treatment and so on and so forth. Rehabilitation is a process, not a quick fix. You have to work with you physiotherapist to complete this process to get rid of your lower back pain.
Stretching and foam rolling
You may feel like your lower back or buttock muscles are tight all the time, but stretching will only help temporarily. The muscle spasm in your lower back is how your body compensates for the lack of stability caused by changes in your ligaments. Stretching these tight muscles will give you some relief for a while. However, due to the pregnancy hormones you might not have anything else to help with stability, so the muscle spasm and lower back pain will just be back in no time.
Not resting
Have you ever heard the saying that pregnancy isn’t a disease? This question is usually asked by someone older who just kept on doing everything they did before getting pregnant. The truth is that your body is going through a lot when you are pregnant and lower back pain is very common. Nevertheless, it does not mean that you should spend all day resting. Listen to your body and if your lower back starts to feel uncomfortable, take it as a sign that you need a break.
Using back braces and preggy belts
In theory using braces isn’t a problem, but in this case it only hides the underlying problem with an external source of stability. A back brace will also block movement and cause further weakness in the muscles around your lower back and abdomen. To treat your lower back pain effectively we need to restore your mobility by getting rid of the muscle spasm. Then we need to increase your own inner stability by strengthening the inner muscles of your lower back to make sure the muscle spasm stay under control through the rest of your pregnancy.
Physiotherapy treatment
All the changes that go with being pregnant can be quite stressful, so not knowing why your lower back hurts or what you can do about it can make you even more anxious. Our physiotherapists can answer your questions to set your mind at ease. We will walk you through the do’s and don’ts.
The main focus of treatment will be to improve the stability around your lower back and pelvis. We do this by using techniques like massage, joint mobilization, strapping and, most importantly, therapeutic exercises. Initially your exercises will focus on motor control, then progress to strengthening and eventually to exercises in less stable positions like step-ups.
Finding the right intensity of exercises is always important, but this is even more true when you are pregnant. Overdoing it will put too much strain on your body, but not doing enough won’t be effective to make you stronger. To improve the stability of your lower back you will be relying mostly on your muscles. This means that finding the right level of exercise is crucial to treat your back pain effectively. Fortunately, your physiotherapist is an expert at guiding this process.
Phases of rehabilitation
1st Phase: Improve mobility and treat muscle spasm
In the first phase of your treatment we will address the stiffness and pain in your lower back. A lot of this stiffness you experience is caused by lower back muscle spasm. At first the muscle spasm was useful to make up for the decreased stability in your lower back caused by ligament laxity. Unfortunately, this usefulness stops when the muscles are too fatigued to work properly. An overworked, exhausted muscle quickly turns into a muscle spasm that puts more stress and tension on your already painful spine. Muscle spasms will also block segmental mobility of your spine. Segmental mobility refers to the small movements between the vertebrae in your spine, so loss of this mobility also contributes to your stiff and painful back.
It may seem like stiffness should solve the problem of instability, so why do we want to improve mobility? The stiffness and muscle spasm you feel in your lower back act like a splint, simply moving the problem to an area that isn’t painful. Or isn’t painful yet… Moving the problem will help temporarily but only until that area also becomes overloaded and painful. Now you end up with an area of stiffness and pain that gets bigger and bigger until you can’t remember which one started first.
This doesn’t have to be the case, though. Your physiotherapist will use techniques like massage and joint mobilizations to treat your lower back muscle spasm and restore this segmental mobility. Strapping is a helpful part of your treatment during this phase. We use tape to give you some external support and take some of the load from your lower back muscles.
At the end of this phase you should be able to change positions more comfortably, like getting up from sitting or straightening up after brushing your teeth.
2nd Phase: Improve stability and start muscle activation
The second phase starts once the segmental mobility in your lower back improves, allowing more movement. The goal of this phase is to start improving the stability around your lower back and pelvis. Ligament laxity is responsible for the feeling of instability in your lower back. Even though treatment can’t reverse the laxity, we can still help you to control the movement better by recruiting some of the other structures in the area. This is where your muscles come in. Not the muscles responsible for the tightness contributing to your back pain, but the small stabilizing muscles in between the lumbar vertebrae.
Once the joints or segments in your spine aren’t held rigid by muscle spasms, these small stabilizing muscle can start firing again. Their main function is stability, so during this phase you will start doing specific exercises to get these muscles firing again. At first your exercises will be in more stable, or easier, positions like lying on your back or sides. As the muscles start to function the way they should, we will make your exercises more challenging by changing positions and adding movement.
Strapping is still a useful part of your treatment to give you some support while we retrain and recruit muscles. We will also continue massage and joint mobilizations to maintain the mobility you’ve gained so far.
At the end of this phase you should be able to lift your hips easily while lying on your back. You should also be able walk and turn around in bed with minimal pain.
3rd Phase: Muscle strengthening
After the previous phase of treatment the small stabilizing muscles in your lower back should be activating and ready to go. In this next phase we will start to build on that foundation by strengthening the bigger stabilizing muscles. This will include your hip muscles to help with stability of your pelvis.
One of the main functions of your pelvis is to support your lower back and provide stability when the rest of your body is moving. Strengthening the muscles around your pelvis will give you a more stable base of support. This is an important step in your treatment, because once your pelvis has more stability the muscles in your lower back don’t have to “fake” stability by blocking your movements.
Exercises will start in more stable positions like in the previous phase, but with added resistance using elastic bands. Your physiotherapist will increase the difficulty of your exercises as your pain and stability improve by adding exercises in positions like sitting and standing.
By the end of this phase you should be able to walk without feeling off balance and climb steps with little to no discomfort.
4th Phase: Maintain mobility and continue strengthening
By the time you reach this phase of rehabilitation you should be able to walk, climb steps and drive comfortably. Turning around in bed shouldn’t wake you up and your back shouldn’t be the reason you struggle to put on shoes.
However, now is definitely not the time to stop looking after your back. As your pregnancy progresses your center of gravity will keep on moving and each week will add extra weight that loads your spine. Your ligament laxity also increases until the end of your pregnancy and only gets back to normal months after the birth of your baby. This means muscles that might have been strong enough at one point won’t be able to keep up after another week.
In the last phase of treatment your physiotherapist will help to maintain the mobility that you’ve gained in the previous phases. We also keep checking the intensity of your exercises and adapt your program accordingly. Your sessions will be scheduled further apart than in the previous phases and the goal of this phase is to maintain improvement and support you through the last part of your pregnancy.
Some other possible treatments for pregnancy-related lower back pain
- Your obstetrician can prescribe medication to help with pain relief and can also do tests to rule out other causes of lower back pain like kidney stones. Be sure to mention any new symptoms to your doctor, especially before you try new or alternative treatments.
- Pain medication and injections should be avoided during pregnancy, unless prescribed by your obstetrician.
- Getting your back or neck ‘aligned’ or ‘clicked’ won’t solve the underlying problem. Lower back pain in pregnancy is due to too much movement without control. Strong techniques that “click” your back will only trigger a protective muscle spasm as your body tries to get more stability.
- A biokineticist can help you with an exercise program to get you stronger safely once your physiotherapist has treated your pain.
- Wearing a “preggy belt” or SIJ-belt can help to relieve some of your symptoms. Unfortunately, these devices provide external stability for your lower back. This leads to further weakness of the stabilizing muscles in the area due to disuse.
- Stretching may help temporarily, but the reason for the muscle stiffness is lack of stability and control in your lower back. If you don’t do any strengthening exercises to “replace” it, your body will have to resort to muscle spasm again in an effort to protect you.
What else could it be?
- Lumbar disc injury – sharp, stabbing pain that gets worse with bending.
- Lower back muscle spasm – a deep, dull ache that is somewhat relieved by stretching.
- Lumbar joint sprain – if you have a sharp, stabbing pain that you can pinpoint you might have a lower back joint sprain.
- Piriformis syndrome – buttock pain with numbness or tingling that can spread to the back of your thigh.
Also known as
- Pregnancy-related lower back pain.
- Pelvic girdle pain.
- Pregnancy-related pelvic girdle pain.
- Sacroiliac (SI) joint pain.
- Buttock pain in pregnancy.

