You may feel chest pain anywhere from your neck to your upper abdomen. Chest pain may be caused by problems in your heart, lungs, throat, muscles, ribs, or nerves. Some of these conditions are serious and life threatening, while others are not. If you have unexplained chest pain, the best course of action is for a medical professional to evaluate you.
Causes of chest pain
There are several causes of chest pain and as stated not all are serious. Chest pain can be caused by internal organs or may even be referral from the back. Chest pain may be caused by:
- Cardiovascular system — referral from the heart (medical emergency)
- Respiratory system — referral from the lungs, usually due to infection
- Gastrointestinal — referral from the stomach and intestines
- Musculoskeletal — referred from muscles, intervertebral discs and joints
- Psychological e.g. panic attacks
- Miscellaneous e.g. tumours
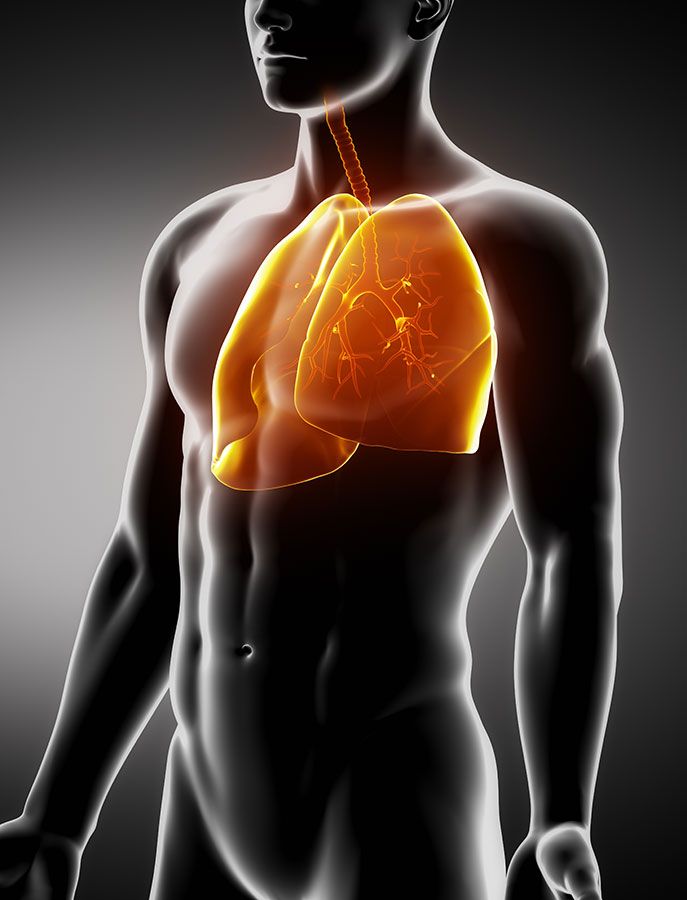
Our professional experience with chest pain
Most people will know we can successfully help in the treatment of musculoskeletal chest. Most people are however unaware of our role during respiratory chest pain. Physiotherapy can be very beneficial to a person suffering from a chest condition, from bacterial lung infections to chronic emphysema.
Our main aim is to maintain a patent airway, by assisting in the removal of secretions form the lungs. We do not provide full chest treatments, but we can refer you to the appropriate Physiotherapist.
If you are struggling with a lot of phlegm, this is a good time for treatment as Physiotherapist can aid you in the removal of the secretions. This will enable you to recover quicker, prevent re-infection and decrease your symptoms especially shortness of breath and fever (caused by secretion retention).
Some other practices are involved at surrounding day-care centres where we perform suctioning and assist in the removal of secretions from children’s lungs to prevent progression of an infection and reduced airflow to their lungs. Babies breathe mostly through their noses up until 7 months old. They are able to breathe through the mouth but struggles to do so, because they are still developing the ability to control of their mouths.
Symptoms of chest pain
Moderate symptoms
- Moderate pain associated with arm movements
- Chronic cough for more than 3 months
- Pain that intensifies when you breathe deeply or cough
- Moderate shortness of breath
- Fever and chills
Severe symptoms
- Crushing or searing pain that radiates to your back, neck, jaw, shoulders and arms &emdash; particularly your left arm
- Severe shortness of breath together with nausea, sweating, or coughing up blood
- Blood in phlegm/sputum
- Feeling anxious, dizzy or generally unwell
- Episodes that often last 10 to 15 minutes or more.
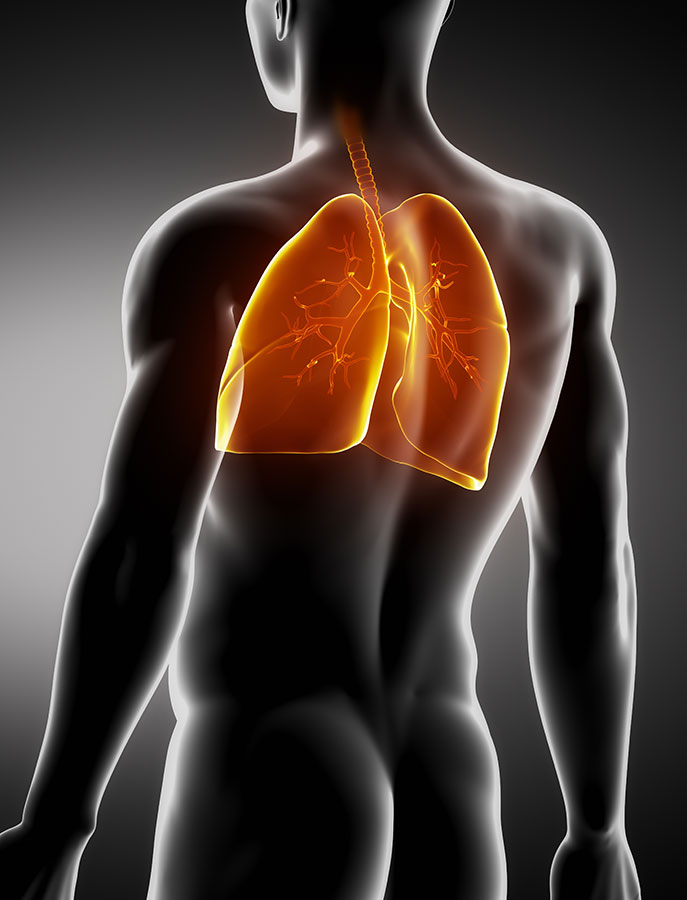
How can physiotherapy help with respiratory chest pain?
Conditions such as upper respiratory tract infection, acute and chronic bronchitis, pneumonia and cystic fibrosis all result in excessive phlegm or sputum production. Retention of sputum not only results in shortness of breath but may be the cause of pain and fever.
We work in conjunction with your physician in the treatment of chest problems. Treatment usually starts with the nebulizing of medication (supplied by the patient or referring doctor) to decrease the viscosity (thickness) of the phlegm. Generally two types of medications are prescribed by your doctor:
Bronchodilators dilate (open) the bronchial passages to assist in easier breathing and space to clear out the secretions.
Mucolytics reduces the viscosity of the mucus in the airways, making it easier to cough up sputum and phlegm.
Lung physiotherapy combine these techniques:
Postural drainage
Involves lying in certain positions that promotes the secretions to drain to the trachea to clear the muscus from the lungs.
Percussion
Involves ‘clapping’ the chest wall to cause mucus to drain through the airway to the main bronchi.
Shaking
A direction specific movement of the chest wall angled at the main bronchi and trachea to clear excess secretions form the airway.
Breathing exercises
Restore breathing pattern and relieve chest pain from coughing.
This treatment allows the patient to breathe easier, clear secretions faster, cough less and prevent lung damage.
What is nasopharyngeal suction?
Nasopharyngeal suction is a Chest physiotherapy technique used by respiratory physiotherapists that involves utilizing the airway of the nose to remove secretions (phlegm) from the upper airways when the patient cannot do so themselves. This inability could be due to:
- lack of an effective cough
- large secretion volumes
- particularly thick secretions
- fatigue
- low level of consciousness
The technique involves passing a suction catheter down the nose’s airway until it stimulates a cough. This is an invasive procedure only used in circumstances where other techniques have been trialed and failed. If repeated suction is required, an artificial nasal airway will be inserted to help decrease discomfort.
Nasopharyngeal suction is often used in combination with manual chest physiotherapy techniques (such as vibrations), to optimize volume of secretions attained. Sometimes nasopharyngeal suction is used to get a secretion sample for analysis; however, suction is only used when:
- Secretions are known to be present
- Accessible by catheter
- Secretions are proving detrimental to patients respiratory function
- the patient is in distress due to the secretions
- The patient is unable to clear the secretions independently by any other means

