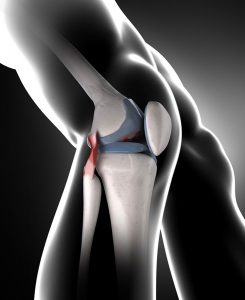
What do you do if you find the front of your knee swollen and sore? You feel worried coz one knee looks bigger and feels warmer than the other. Moving it feels very limited and painful. Sitting down or getting up gives you a sharp pain in the front of your knee and the thought of kneeling down is excruciating. If you feel any of these things, you could have a knee bursitis.
There are quite a few bursae around your knee and any of them can become inflamed, causing bursitis. You’ll feel that the obvious thing to do, is to rest and let the swelling settle, but often people struggle with recurring knee bursitis and pain. Especially when they try to get back into exercise again. To prevent this from happening, it is vital that you get help to get to the root of the problem and get the right treatment for your knee bursitis, from the start.
What is a bursa? And how does it fit into the anatomy of your knee?
Let’s look at the different structures that make up your knee joint.
Bones and joints
Your knee joint is formed by three bones namely: the femur (thigh bone), the tibia (shin bone) and the patella (knee cap). The patella sits in front of the femur and gives the front of your knee it’s round shape. When you bend or straighten your knee, your patella slides up and down as well.
All these bones are covered by a layer of cartilage, so that movement can be smooth. The femur and tibia form the tibiofemoral joint, whereas the patella and femur form the patellofemoral joint.
Joint capsule and ligaments
The tibiofemoral joint is covered by a layer of tissue, called the joint capsule. Together with the knee ligaments it helps to hold the joint together and keeps the joint fluid inside. Altogether, these structures improve the stability of your knee joint. The patella is positioned outside of the joint capsule.
Muscles and tendons
Here are the main groups of muscles that help you to move your knee:
- Quadriceps: This muscle stretches all the way from your hip bone, down your thigh and attaches at the front of your knee, below your patella. The quadriceps tendon is like a thick cable that attaches to your shin and it pulls your lower leg up when you straighten your knee. Your patella is directly attached to this tendon. So, when your quadriceps contracts, your patella slides up as well.
- Hamstrings: Like the quadriceps, your hamstring is a long muscle at the back of your thigh, stretching all the way from your sitting bone to the back of your knee. It splits into two separate parts and one part attaches to the inside of the knee, whereas the other attaches to the outside. This is the main muscle to help you with bending your knee.
- Calf muscles: These muscles can also be found at the back of your leg, running from the back of your knee down to your foot. They assist the hamstrings to bend your knee.
- Adductors: These are your inner thigh muscles. They start high up in your groin and run down the inside of your thigh to attach to the inside of the knee, helping you to cross your legs.
Each muscle that attaches to your knee joint, attaches via a tendon. These tendons anchor the muscles to the bone.
Bursa
A bursa is a small, slippery, fluid-filled sac and we have several around each joint in our body. Their main job is to decrease the friction between muscles, tendons and bones as they rub over each other. Some of the knee bursae are located superficially, just underneath your skin. Whereas, other are located deeper, in between other layers of tissue. Some of the deeper bursae connect with the joint capsule and joint fluid. In other words, if the fluid inside the knee joint builds up, it automatically affects the fluid inside the bursa as well, leading to swelling. The membrane of each bursa is permeable, meaning fluid can pass into it from surrounding tissues.
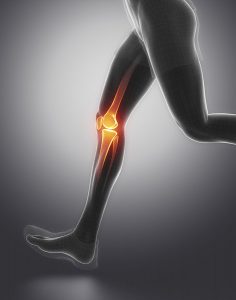
The bursae around your knee are called:
- Suprapatellar bursa: Located between the femur and the quadriceps, just above the patella. It allows for movement of the quadriceps muscle over the distal end of the femur.
- Prepatellar bursa: This bursa lies on top of the patella, between the patella and the skin. It allows for movement of the skin over the underlying bone.
- Deep and superficial infrapatellar bursa: Below your patella, is the spot where your quadriceps tendon attaches to your tibia. The deep infrapatellar bursa lies beneath the quadriceps tendon, whereas the superficial infrapatellar bursa lies on top of it. Basically, they allow smooth movement between the tendon, the bone and the skin.
- Pretibial bursa: This one is located between the tibial tuberosity and the skin. That is the bony knob just below your patella. It allows smooth movement of the skin over the tibial tuberosity.
- Lateral gastrocnemius bursa, fibular bursa, fibulopopliteal bursa and subpopliteal bursa: All of these bursae can be found at the back of your knee on the outside. Each of one is located between a layer of muscle tissue and a bone. They allow smooth movement of these muscles’ tendons over the bone.
- Medial gastrocnemius bursa and bursa semimembranosa: These bursae are also located at the back of your knee, but on the inside. They lie between layers of your calf muscles and hamstring muscles where they attach to the femur or tibia. They also also allow for smooth movement of these muscles’ tendons over the bone.
- Pes anserine bursa: This bursa is found between the medial (tibial) collateral ligament and the pes anserinus. The pes anserinus is the connection point for the tendons of three muscles namely: sartorius, gracilis, and semitendinosus. This bursa prevents friction between the ligament, the bone and the tendon.
Clearly, there are a lot of bursae around your knee and their names probably sound funny. So, how do you know which one is the one that is causing you problems? Usually, it is the prepatellar, infrapatellar or pes anserine bursae that becomes inflamed, causing knee bursitis. But technically you could get bursitis in any of these bursae.
What is the function of a knee bursa?
Have you ever looked at your knees in a mirror? There are quite a few bony points and knobs that can be seen and felt around your knee. Now, imagine the friction between these bony points and the surrounding ligaments, tendons and skin each time you bend or straighten your knee. It will get even worse if you walk or run, because then you are bending your knee repeatedly.
Bursae reduce friction and cushion pressure points between your bones, tendons, muscles and skin near your joints. The bursae around your knee makes it possible for you to bend and straighten your knee over and over again during your normal daily routine. Whether it involves you climbing stairs, running, cycling or squatting down.
Without them, these points of pressure would have caused severe, burning friction that could have frayed the tendons or ligaments like a rope.
I have knee bursitis. How did it happen?
You can compare a bursa with a water balloon filled with only a little bit of water. If you fill this balloon with more water, it is going to swell up and become bigger. The pressure of the water inside will simply build up more and more. Now, if you try to squeeze this water balloon into a box or a confined space, it fills the whole space and increases the pressure inside of it.
Instead of water, a bursa is filled with synovial fluid (joint fluid). And the term bursitis means: inflamed bursa. Excess friction and pressure on a bursa cause injury, which in turn cause inflammation. With inflammation in the bursa, the synovial cells will multiply and increase collagen formation and fluid production. The membrane of the bursa is permeable and allows the entrance of high protein fluid, which increases the volume of fluid in the bursa. With prolonged inflammation, the membrane of the bursa can even become thickened and fibrous.
Now, come back to the picture of the water balloon. If one of the bursae around your knee becomes inflamed and swells up like a water balloon, it increases pressure on the tissues around it. Usually, there is enough space for the gliding movement between tissues, but with swelling, that space gets cramped. It is bound to cause you a lot of pain and limit your movement, due to the fact that other tissues now get irritated and sore as well.
Usually, it is the prepatellar (front), infrapatellar (below) or pes anserinus (inside) bursa that is affected. That is why knee bursitis is known for swelling that makes the front of your knee look big and round.
Very seldomly can your diagnosis simply be knee bursitis as it doesn’t happen out of its own. Something needs to irritate it, for it to become inflamed.
Causes of knee bursitis
Increased friction – Bending your knee repeatedly during running, walking, cycling, or climbing stairs will all lead to increased friction between muscle tendons and bursae of the knee. This irritates the membrane of the bursa and leads to bursitis
Increased pressure – Kneeling is a position that can often lead to knee bursitis. Doing an activity that require you to kneel for a long time can easily cause knee bursitis e.g., scrubbing the floor, gardening, playing with your dog or kneeling next to the bath when your kids take a bath.
Direct trauma – Falling directly onto your knee or being hit directly on your knee can injure a bursa and trigger it to start swelling.
Infection – If a bursa gets infected by bacteria, it will also swell up and cause symptoms much the same as knee bursitis.
Inflammatory conditions – Conditions such as gout, arthritis or tuberculosis can cause increased levels of inflammation in your body, which can make you more prone to bursitis.
Muscle imbalances and patella tracking problems – If certain knee muscles work harder than they should, it leads to more friction and more irritation.
Knee joint instability or hypermobility – The knee joint gets pushed into uncomfortable positions due to a lack of stability to keep it in place. This leads to increased pressure on bursae around your knee.
Often, knee bursitis is caused by more than one factor. Sometimes, it starts with an injury, but most often it feels like it starts out of the blue and simply gets worse.
How severe is my knee bursitis?
Mild – You can bend your knee almost fully before you feel pain
You will feel like you still have full range of your knee movements and will feel pain only when you’ve bent your knee all the way or when you’ve done a sumo squat. The swelling of the bursa is still minimal and it only irritates the tissues around it when you’ve put enough pressure on it.
Moderate – You cannot bend your knee further than halfway
Now, you regularly feel knee pain. It looks swollen and puffy and bending your legs to sit down or climb stairs is painful. At this stage, the inflammation has caused enough swelling that the bursa has started to irritate the tissue around it. When you bend your knee, you simply increase the pressure on it, making it feel much worse. Resting seems to help, although when you’ve sat down for a while, your knee feels really stiff when you want to get up and walk again. Exercise makes it feel much worse, because doing more with your knee leads to increased swelling and inflammation of the bursa. This is a tricky phase indeed because you will feel better when you don’t move your leg. Unfortunately, that is no way to live and if you simply push through the pain and swelling, it can easily become worse.
Severe – You cannot bend your knee at all and you can’t straighten it either
Your knee looks really bad. The swelling makes your knee look like a tennis ball. Together with that, it feels really warm and looks angry and red. The pain and discomfort bother you constantly. You can’t sleep and you can’t walk The swelling and inflammation has become so severe that any movement irritates it by putting further pressure on it.
If bacteria gets into a bursa, it can cause septic knee bursitis. Then, it will cause infection together with the inflammation. The fluid inside gets infected and needs to be treated by antibiotics or needs to be drained. With septic knee bursitis, you will also feel ill, eg. fever, body aches, chills etc. You will need to consult a doctor.
Diagnosis
Physiotherapy diagnosis
Our physiotherapists are experts in human anatomy and movement, with the necessary experience to diagnose knee bursitis. We understand the biomechanics of your knee joint and how the surrounding muscles, tendons and ligaments affect your knee movement. We can accurately diagnose which knee bursa has been affected and also help you to determine what could be the underlying cause. Doing a full clinical assessment and getting the necessary information about your pain is the starting point.
During your physiotherapy evaluation, we will stretch and stress your knee joint, test the strength of the muscles that attach around the knee and evaluate your knee and hip stability. This way we’ll be able to know how your knee movement and activities have been affected.
Thorough evaluation makes our physiotherapists the best at diagnosing this type of problem.
X-rays
X-rays will only give us an image of the bones in your knee. Knee bursitis cannot be seen on an x-ray. However, x-rays will show the integrity and alignment of your knee joint. If your physiotherapist feels it is necessary to evaluate the knee joint as a possible cause of your knee bursitis, you will be referred to the right place.
Diagnostic ultrasound
A diagnostic ultrasound (sonar) will be a helpful test to confirm the diagnosis of knee bursitis. It is able to show excess fluid and swelling.
It is not compulsory that you get a sonar before you see your physiotherapist for the first time. However, if your physiotherapist feels it is necessary that you get one, you will be referred to the right place.
MRI
An MRI scan can image all of the structures in your knee, including bursae, muscles, tendons, joints and bones. However, you need a referral from a specialist to get an MRI scan and it is an expensive test.
It is unnecessary to get an MRI straight away, but if your physiotherapist feels it is necessary for you to get one, you will be referred to the right specialist.
Why is the swelling and pain not going away?
Initially, your knee pain is caused by inflammation and swelling of a bursa, causing pressure and irritation when you move your leg. Resting seems to help, so you start to use your leg less than before. Unfortunately, this leads to stiff muscles and joints and compensatory muscle patterns.
On the other hand, it isn’t that easy to avoid using your leg. Routine activities like walking, climbing stairs, sitting down, getting up of driving all cause you more pain. These movements cause irritation that can lead to more inflammation and it starts up the cycle of pain again. You can easily become stuck in a cycle of pain, not knowing if it is safe to move or not.
Effective treatment of knee bursitis needs to adress the underlying cause. Swelling needs to go down and the bursa needs to return back to its normal size. Friction needs to be reduced by adapting your activities. Then, with time, the tissues need to get used to moving again and should be conditioned for the work that they should do.
The sooner you sort out exactly what is causing the knee bursitis, the better. It is the only way to prevent the swelling and pain from coming back again.
Problems that arise when we see patients with knee bursitis
Waiting too long and not getting a proper diagnosis
A common problem we see is that patients wait too long before they seek help. By the time patients come to us for help, they have severe swelling that limits a lot of their movements. In some cases, they even had knee bursitis a few times before. The longer you wait, the more advanced the problem becomes and the longer it will take to get better.
If you don’t get a proper diagnosis from the start, it wastes time. If anyone treating your knee bursitis is not looking for the cause, they will keep on treating only the symptoms. This is ineffective, as your knee bursitis could simply return.
Trying out, but not completing different forms of treatment
Often, patients take anti-inflammatory medication in the hopes that it will ease their swelling and pain. Or they try to get relief by putting transact patches or ice on their knee. These treatments might make your swelling and pain feel somewhat better, but they are not adressing the root cause of what is causing your knee bursitis. Chances are, that once you try to get active again, the swelling will simply flare up again.
Using crutches or wearing a knee brace might be useful in the beginning to make it easier for you to walk, but it won’t be a long term solution. The longer you use it, the more dependent you will become on it. It leaves you with a weak knee that feels very stiff.
And then, a lot of people tend to feel a lot better once their swelling and pain eases, so they stop their treatment halfway through the treatment programme. You need to address the deeper problems and make sure your knee muscles and tendons can do the work that you require of it. That is the best long-term solution. So make sure you complete your knee bursitis treatment program. Patience is key.
Resting too much or too little
Resting and elevating your leg too much leaves you weaker than before. Whereas, too much movement, exercise and stretching will leave you with more swelling, pain and inflammation. People tend to want to stretch or foam roll to ease the stiffness in their knee, but you can easily overdo it. Finding the balance between resting and doing safe movements is key!
Let us help you get the right treatment for your knee bursitis and stop it from stopping you in your tracks.
Physiotherapy treatment
We can provide the best treatment for the swelling, pain and stiffness caused by knee bursitis. We understand that you want to crouch down to play with your kids or work in the garden without worrying about getting up again. That is why we are here to provide guidance and answers. Physiotherapists can implement a very effective and structured plan of action that treats all the aspects of your knee bursitis and gets you back to your living your life confidently. Our physiotherapy treatment will help you to get the full movement and strength of your knee back.
The basic structure of our treatments:
- Determine which knee bursa is affected
- The severity of the inflammation
- Protect it from further injury
- Give it time to heal
- Regain movement and strengthen
- Re-evaluate to monitor progress
We will be looking at different aspects, like your knee’s ability to move and provide stability. This includes muscle strength, range of motion, flexibility and stability. Treatment for knee bursitis will include: soft tissue massage, joint mobilisations, dry needling, strapping, laser therapy, nerve mobilisations and guiding you through a rehabilitation program of gradual strengthening, control and conditioning. It’s important that you commit to the treatment plan, as this improves your chances of successful long-term recovery.
Phases of rehabilitation
1st Phase: Protection and initial healing
Protect
Patients tend to push through their pain and even continue to exercise with knee bursitis. This can cause continuous inflammation and pain. Protect the injured area by resting more than usual and avoiding painful movements.
Avoid anti-inflammatory medication
Avoid using anti-inflammatory medication if possible as it delays healing. Ideally, use only pain medication without an anti-inflammatory component in the initial phases of your injury. That way, your pain will be under control, and with time you can taper off and stop taking the medication completely.
Compression and heat
Strapping can provide good support for the painful area in your back, which in turn will decrease your pain. Heat also has a pain-relieving effect, so you can apply a beanbag or hot water bottle to the area of your pain.
Information
Make sure that you get information from the person that is treating you. Its important to understand what you should and shouldn’t do. If you are informed, you can also make the right decisions. Your body knows best, so avoid too many types of treatments at once.
Load
Let pain guide you to gradually return to your day to day activities. Initially, it is tricky to know if it is better to rest or to move, but finding a balance between the two is the best you can do.
2nd Phase: Tissue healing and improving knee range of movement
We will monitor the levels of inflammation and pain and help to improve the healing process taking place. Less inflammation means less swelling of the bursa and that means less irritation and pressure. On a cellular level we’re able to accelerate healing using dry needling, laser and ultrasound. With time, the swelling should go down and your knee should look normal again. This allows the muscles, tendons and layers of tissue to move freely again. Ultimately, that is how you get full range of your knee joint back.
During your examination, it will become clear what you are able to do, and what you should avoid. You’ll be able to bend your knee up to a certain point, before your pain starts. This is your pain-free range of movement and our exercises will be targeted between these boundaries of your pain. With time, the pain-free range of movement will increase and you’ll regain the full range of movement of your knee.
3d Phase: Posture, walking pattern and knee stability
The way you walk and use your leg during everyday activities, will influence the position of your patella and knee joint. As well as the muscle balance around the knee. Adressing your gait pattern and the way you position your knee during exercise is the first step to improve knee stability. Your knee should be stable enough for you to sit down or climb stairs without feeling like it can’t carry your weight. Doing balance exercises and weightbearing exercises will be part of this phase.
4th Phase: Strength and endurance
It’s common to feel some pain when you start to exercise again. Your muscles now need to adapt to the work that you require of them again. Poor endurance and fatigue could be another reason for pain when you exercise. Luckily, this will get better when you strengthen the muscles around your knee and your day to day activities will become easier again. Kneeling down won’t be such a daunting task. During this phase of rehabilitation we will progress your exercises more and more, adding resistance, doing more repetitions and building your overall strength and endurance.
5th Phase: Getting back to your routine, training or sport
Gradually returning to your routine and getting used to the intensity of your usual activities is a big part of your recovery. We need to determine if you are ready to return to fully working and training without any painful flare-ups of knee bursitis. Even with repetitive movements throughout your day, like walking or running, your knee joint, bursa and surrounding muscles should be able to carry the load. Your physiotherapist will guide you to re-engage in safe increments, and make adjustments where necessary.
Getting you back to running, cycling, swimming or jumping is the ultimate goal.
Healing time
Usually, knee bursitis is a secondary problem, not necessarily the PRIMARY problem. So, we must first determine if the swelling and inflammation was stimulated in response to an underlying overuse or biomechanical injury. Typically, the swelling should start to settle within a week, but you may still experience knee pain or stiffness in the weeks to come. It can take anything from 3 weeks to 6 weeks to clear up.
Depending on the severity of your symptoms and initial inflammation, you will need physiotherapy treatment twice a week for the first two weeks. After this, your treatment sessions can be spread out to once a week or once in two weeks. You only spend an hour at a time with your physiotherapist. How fast you recover will greatly be up to you. If you complete your physiotherapy treatment protocol, you should be able to recover completely and return to your sport.
Other forms of treatment
- Your doctor will probably prescribe anti-inflammatory medication or give you a cortisone injection to get inflammation to ease. Both of these medications will give temporary relief to the swelling and stiffness that you are experiencing. However, it will not be the solution to your problem. Once the effect of the medication wears off and you try to get back to working or exercising, your bursitis could simply return.
- Getting your knee ‘aligned’ or ‘clicked’ in the hopes of improving your knee stiffness will not improve the state of the bursitis. It could even worsen or trigger an inflammatory reaction again. You need to look at the bigger picture.
- A biokineticist will be able to help you in the final stages of your rehabilitation or to get you back to actively training for your sport.
- Using crutches and wearing a knee brace might help with the discomfort from the swelling initially, but it won’t be the solution to your problem. In fact, muscles become weaker when you wear a brace and you become dependent on the brace. It will only worsen your problem.
- Stretching or foam-rolling your knee will not help for the swelling or the pain. You can easily overdo it and irritate it even further.
Is surgery an option?
Surgery is not the first option for knee bursitis. Recurring knee bursitis happens due to other underlying injuries. An orthopaedic surgeon might be able to remove or drain your swollen bursa. However, that will greatly affect the amount of friction on the spot where it is removed. It might feel like a solution in the moment, but you run the risk of future surgeries because without the bursa, your muscles and tendons could now be injured too.
If the swollen bursa has become septic, you will need to see a doctor to get antibiotics or to have the bursa drained of the septic fluid. Your physiotherapist will refer you to the right doctor, if the the underlying cause of your knee bursitis seems worrying.
What else could it be?
- Knee ligament injury: Usually a traumatic type of injury that leads to a tear of one of your knee ligaments. Symptoms include: knee swelling and bruising and pain when walking.
- Osteoarthritis: Pain and stiffness of the knee that feels especially worse in the mornings and with cold weather.
- Patellofemoral pain: Pain at the front of the knee that becomes worse with exercise or repeatedly bending your knee. The movement and position of the patella is the problem with this condition.
- Knee tendonitis: Any of the tendons around your knee can become inflamed with overuse type of injuries. Often goes hand in hand with bursitis. Pain feels worse during or after exercise