A medial collateral ligament injury or MCL sprain is one of the most common knee ligament injuries. This ligament is located on the inside of the knee and it prevents gapping between the thigh bone (femur) and shin bone (tibia). An MCL tear occurs when the force on the ligament is too great to resist, usually due to a direct blow to the side of the knee or twisting your knee when your foot is fixed on the ground.
Under normal circumstances the knee moves in a straight line – bending and straightening. The ligaments on the side of the knee (collateral ligaments) prevent side to side movements of the knee in other words valgus (prevented by the medial collateral ligament) and varus (prevented by the lateral collateral ligament). A direct blow to the outside of the knee or thigh will cause a valgus force on your knee, putting tension on the MCL. These are usually high speed injuries, so you cannot correct the position of your knee before there is too much strain on the ligament. This results in an MCL sprain or tear.
What is the Medial Collateral Ligament?
A ligament is made up of densely packed collagen fibres. These collagen fibres do not stretch, so a ligament’s main function is stability in other words preventing specific movements. The medial collateral ligament is the biggest ligament on the inside of your knee. It is one of four knee ligaments responsible for the stability of your knee.
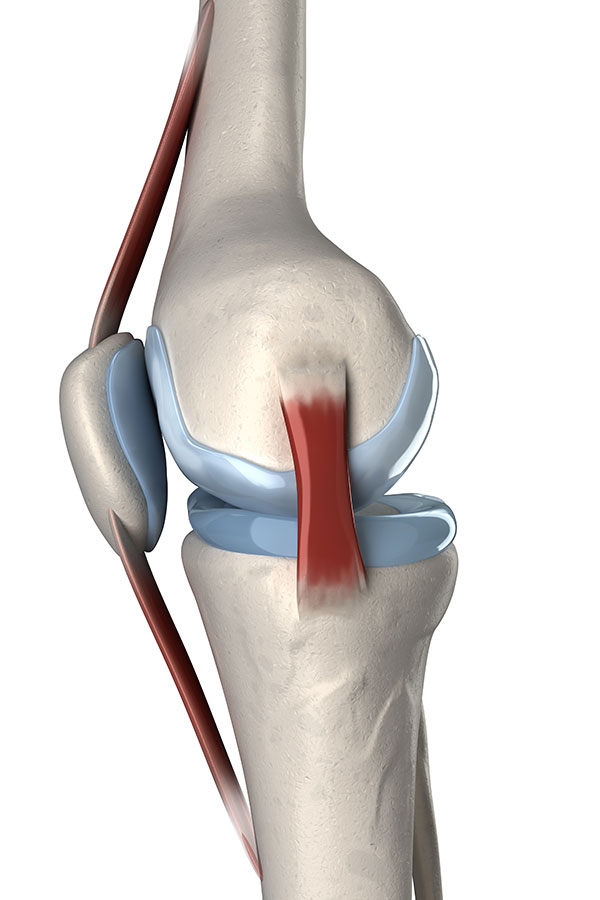
The MCL can be divided into superficial and deep fibres starting at the medial femoral condyle (the bony part on the inside and top part of your knee). The superficial fibres run down the inside of the knee and attach to the inner part of the shin bone. The deep fibres become part of the capsule surrounding the knee joint. This part of the ligament attaches to the top of the shin bone and the medial meniscus.
What does the Medial Collateral Ligament do?
The main function of the MCL is to resist a valgus force, in other words to prevent the tibia (shin bone) from moving too far outwards in relation to the knee joint. So when you are standing and your knee moves inwards, the MCL takes up the tension to prevent excessive movement. The medial collateral ligament is more vulnerable when the knee is bent, because the ligament is relatively lax in this position.
Another function of the MCL is to assist the ACL in preventing the tibia (shin bone) from moving too far forwards. This is why the ACL should always be assessed when you have pain on the inside of your knee.
How does an MCL injury happen?
A ligament sprain is a form of overstretching of the ligament. There are several classifications for ligament sprains depending on the severity (grade 1, 2 or 3). The fibrous band is like a pulley, which prevents the joint from moving into extreme ranges. When the force is too big for the ligament to resist, the fibers will tear. Overstretching the MCL may result in tears or a sprain of the ligament. It is important to know and understand the difference and implications. In the case of a tear, you may hear a snap or tearing sound.
For example when a rugby player is tackled on his knee from the outside with his foot firmly planted, the weight of the tackler will be greater than what the MCL can resist. The force against the player’s knee pushes his knee inwards. The MCL is at full tension while an uncontrollable load is being forced on it, therefore the ligament is pushed beyond its limits, causing a ligament tear or rupture.
The collagen fibers snap like a tension cable when overloaded and the fibers unravel. On a cellular level, injury will cause a split along the sheath of the ligament (like a sleeve around the ligament). Inflammation develops in response to injury which causes swelling, pain and loss of function, causing the knee to buckle inwards. The swelling contributes to loss of space around the ligament that restricts the normal movement of the ligament in its sheath. Mucoid degeneration and fibrinoid necrosis (a type of cell death) indicate ligament tears.
Causes of a Medial Collateral Ligament injury
Acute medial collateral ligament injuries
An MCL sprain occurs mostly during sporting activities and a single, sudden overload on the ligament will be classified as acute trauma. For example, during a rugby tackle to the side of your knee causing your knee to buckle inwards.
Another example could be during netball or ballet, when your foot stays planted on the ground, but your upper body and knees turn either in or out. This causes the MCL to twist which can result in a sprain, especially with fast movements when you cannot correct the position of your knee in time.
Medial collateral ligament injuries could also be the result of non-sporting activities like missing a step and falling on the knee with your foot turned outwards.
Chronic medial collateral ligament injuries
If the knee stability muscles are not firing properly the ligament will have to take up the slack, increasing your risk of a medial collateral ligament injury. If the ligament doesn’t get properly treated and rehabilitated, it could cause repetitive sprains. Recurrence of micro tears in the ligament could lead to laxity or rupture of your ligament.
How bad is my MCL injury?
Grade 1 MCL sprain (mild)
A small amount of fibers torn, you will have some discomfort and pain. The ligament only sustained a mild stretch injury. No swelling and minimal pain, but you may run into problems if the cycle repeats itself. Recurrence of micro tears in the ligament could lead to more severe tears. You will have no loss of function or range of movement of your knee, but may experience pain at some point during the movement. You will be able to continue playing.
Grade 2 MCL sprain (moderate)
A partial MCL tear with some swelling and bruising. Pain level increases quite a bit from a grade I and moving your knee will cause pain. It may feel uncomfortable to bend or straighten your knee and it may feel unstable, as if the knee wants to “give way”.
In a grade 2 MCL injury 20% to 80% of the fibers torn. You will not be able to put weight on the leg in other words take a normal step. Even if you try to continue playing, you will have a considerable amount of pain and limping. The pain will not allow you to straighten your knee or lift your leg forward (knee to chest).
Grade 3 MCL sprain (severe)
A complete MCL tear. Swelling and discoloration (bleeding under the skin) are visible. The knee feels as if it wants to give way completely. Putting your full weight on the leg is nearly impossible. Bleeding and swelling will definitely be present.
The main concern with a grade 3 tear is the ligament’s ability to stabilize the knee joint – if the ligament tears into two separate flaps, there is no way the ligament can ‘heal’ or reattach without surgery. A Sonar or Diagnostic Ultrasound will show the full extent of the damage. Surgery is the best option to reconnect the separated segments of the torn Medial Collateral Ligament.
Often there will be no pain, but the disfigurement is quite obvious, since all the fibers are torn. It is important to know that there could be other structures involved with such an injury, but we will discuss this in more detail with our differential diagnosis later.
Diagnosis Medial Collateral Ligament injury
Physical Examination
After taking a thorough history and finding out how the injury happened physiotherapists can determine which parts of your knee may be injured. We do specific tests for each structure in the knee, so we can differentiate between what is injured and what isn’t. If you’re uncertain, let us rather have a look and give you our opinion.
To test the integrity of the medial collateral ligament we use the MCL valgus stress test, Swain test and Anteromedial drawer test. Using these tests we can accurately determine if there is an instability or medial collateral ligament injury in your knee. In our assessment we also test the ligaments on the inside, outside and the menisci (cartilage) in the knee.
X-rays
X-rays can be helpful to exclude fractures of the patella, femur, tibia or fibula, but will not show an MCL tear. This is usually the test most emergency rooms opt for, but when there are no fractures diagnosed, they conclude that the ‘knee ligaments’ are torn. However, this doesn’t tell us much. Get to your physiotherapist so that we can test each ligament individually and get a more conclusive diagnosis.
It is important to note that children have softer bones, though. The anchor of the ligament can tear away from the bone more easily resulting in an avulsion fracture, which may be visible on x-ray. It is essential to make sure there are no fractures if we suspect a medial collateral ligament injury in a child before proceeding with further tests.
MRI
An MRI may be useful to rule out other injuries to the knee, for example, a meniscus injury, bursitis, ACL, tendonitis. But when a pure MCL injury is suspected, it is an unnecessary and expensive thing to do an MRI. The deep part of the ligament is more prone to injury, which could also lead to a medial meniscus injury, in which case an MRI would be necessary. However, this is an expensive test and you will need to consult an orthopedic surgeon to be referred for an MRI.
Why is my ligament pain not going away?
If you are asking yourself ‘why is it taking so long for the pain to go away’ then you might want to consider the following: When a ligament tears the body will repair the injured fibers by sending cells to start the healing process of the torn ends of the fibers.
Healing is a process and any injury needs time to recover and become strong again. The torn ligament reacts the same as an open wound, like having a cut on the bottom of your foot. If you keep walking on it, you will shear away the healing cells that are closing the wound. The more you walk or run through the pain, the longer it will take to heal. If the pain returns every time you start running again, you have missed the most vital aspect of the healing process. The ligament length and strength must return to normal before you return to participating.
Getting worse
Therefore, the medial collateral ligament can be prone to recurring injury or progression of the injury from a grade I to II or III. If you sustained a grade I injury the pain will settle down over a couple of days. The ligament isn’t healed yet, but because the pain improved you return to your normal sport, for example rugby. Your knee bends while you run and you have to suddenly change direction while your foot stays on the ground and your knee bends inwards. The ligament is definitely not ready to handle this load yet. You may have made it worse progressing from a sprain to a tear. It is always better to allow the full healing time whilst strengthening the muscles around the knee before getting back onto the sport field.
If you are taking anti-inflammatory medication for your ligament tear, STOP taking them. Inflammation is the body’s natural way of healing the injured collagen fibers. The medication is preventing this process from taking place, not to mention masking the effect of the trauma on the tissue if you return to running while still using anti-inflammatories.
What NOT to do
What you should do
Making the injury worse
Physio treatment for Medial Collateral Ligament injury
Physiotherapy treatment of an injured or torn MCL will start with a detailed assessment. This is how we make an accurate diagnosis and plan the course and goals of treatment. For example, the treatment plan and goals of a rugby player will differ from those a dancer or recreational runner.
Physiotherapy modalities used to treat knee ligament injuries may include:
- Manual therapy – we use joint mobilizations if the knee joint movements are restricted.
- Soft tissue massage – we use specific soft tissue mobilization to make sure the ligament doesn’t become stiff and tight as it heals.
- Electrotherapy – Laser and Ultrasound to promote healing of the ligament.
- Dry needling or acupuncture – to release tension in the thigh muscles.
- Strapping – we use strapping to help with pain relief and swelling.
- Taping – taping can be used to correct bio-mechanical problems.
- Exercises – as your injury heals we will increase the intensity of your exercises.
- Education – explaining your condition and our treatment plan is a major part of physiotherapy. You are encouraged to ask questions throughout the process.
The end goal of rehabilitation is always to return our patients to their pre-injury level of activity.
Rehabilitation & Goals
1st Phase: Protection & initial Healing
P
Protect.
A hinged knee brace may be necessary to protect the MCL injury and limit movement of the knee joint, especially side to side (valgus and varus) movement. If you experience pain when putting your full weight on the knee or walk with a limp, you should use crutches when walking until you can tolerate full weight-bearing. Pain is your body’s warning that you need to protect the area.
R
Rest.
Do not continue training/sporting activity at this stage. A physiotherapist will be able to guide you in gentle, pain free exercises to start strengthening muscles around the knee without putting excessive strain on your injured MCL.
It is also important not to return to sports (even if the pain improves) without having the knee assessed. Not having pain does not necessarily mean your injury has healed completely.
I
Ice.
Ice cubes wrapped in a towel, tied around your knee reduces pain & inflammation and speeds up the healing process. For at least the first 3 days or until the swelling goes down, apply an ice pack for 20 minutes every two hours. Always keep a towel between the ice and your skin (to prevent freeze burn).
C
Compress.
Use strapping or elastic compression bandage to keep your MCL injury supported and to control swelling. You will also find that it will help with pain relief. This can be done either with taping or tube grip bandage.
E
Elevate.
Lying on your back with your foot on a chair (your knee must be higher than your heart to allow gravity to assist in reducing swelling). Raise your knee for 15 minute intervals during the day.
2nd Phase: Establish pain free range of movement
During our examination and testing, we will find out what you’re able to do and what you should avoid. We will identify factors that contribute to your pain, specific to your MCL injury. There is a pain free range of movement that you will be safe to move in and during this phase our exercises will stay within these boundaries. For example full extension (straightening your knee) will be painful and full flexion (bending) will also cause pain with an MCL sprain. This means that your initial exercises will be where the knee is in a relaxed, pain free position.
As your rehabilitation progresses we aim to gain a larger pain free range of movement while your painful range becomes less intense.
3rd Phase: Tissue healing
We monitor the healing of your MCL tear and track the fibrous tissue formation, re-attachment and scar tissue healing. On a cellular level we can support the healing process using dry needling, laser, ultrasound and electrotherapy.
4th Phase: Regain Full Range of movement
One of the most important components of rehabilitation after a medial collateral ligament injury is regaining full range of movement of your knee joint. We use massage, stretches, neurodynamic- and joint mobilizations to achieve full range of movement.
We will guide you with static exercises, for example pressing your knee down into a rolled up towel, to start regaining muscle control around the knee. It is important to decrease swelling if your knee is still swollen at this point.
Once you can tolerate full weight-bearing you will progress to the next phase of rehabilitation.
5th Phase: Restore Full Muscle Strength
Another crucial part of rehabilitation after an MCL injury is to restore full strength of the muscles around your knee. Dynamic strengthening exercises are introduced during this phase of rehabilitation while treatment will also still aim at restoring and maintaining full range of movement (bending and straightening the knee).
The main goal during this phase of rehabilitation is regaining muscle control during daily activities for instance walking, squats and standing on one leg. After this phase of rehabilitation you should be able to start light jogging and return to full activities of daily living i.e. walking, driving etc. without pain.
To progress to the next phase of rehabilitation you should be able to stand on the injured leg and bend your knee (single leg squat).
6th Phase: Improve control of rotational- and valgus forces on the knee
In this phase of rehabilitation we will add a rotational (turning) component to exercises to protect the healing MCL tear. The muscles that control rotation of the knee should be strong enough to prevent excessive load on the medial collateral ligament, especially when rotation is combined with flexion (bending the knee). Rehabilitation will focus on controlling twisting movements for example when you get into the car or change direction when walking fast.
You can progress to the next phase of rehabilitation when you can perform walking lunges with an upper body twist.
7th Phase: Agility training
Agility training will commence once range of movement and muscle strength have been restored. The goal of this phase of rehabilitation is to restore your ability to move quickly and easily while preventing a recurrence of your MCL sprain. Examples of exercises would be quick steps in different directions, sprints with change of direction, acceleration (going faster) and deceleration (slowing down) exercises.
This phase is important to enable your knee to respond to sudden changes, for instance if you slip on a wet floor and lose your balance.
You will progress to the next phase of rehabilitation once you can perform changes of direction quickly and easily.
8th Phase: High load resistance training
One of the final phases of rehabilitation is strength training with high loads. All the components of the previous phases will still be maintained, but more resistance will be added to exercises. This is important for heavy everyday activities you may need to perform for instance carrying heavy furniture up a flight of stairs.
You will progress to the sport-specific phase if range of movement, muscle strength, agility are restored.
9th Phase: Testing for return to activity
Gradual build up into your previous intensity of normal activities and training to determine if your MCL injury is able to withstand the repetitive loading without flare-ups. Our physiotherapist guides you to reengage in safe increments and will adjust where necessary. We’ll follow your progress and adapt where needed.
Rehabilitation during this phase will start focusing on return to sport. Range of movement and strength developed during the previous phases will be maintained and exercises for power and sport-specific agility will be added to the exercise program. Exercise repetitions and training time will be increased to build endurance. Plyometrics – like jumping down from a step, jumping onto a box etc – will also be an important part of your rehabilitation during this phase.
At the end of this phase of rehabilitation you should be able to run, change direction and perform jumping activities in different directions without pain, discomfort or apprehension.
10th Phase: High Speed, Power, Proprioception
This is the final stage of rehabilitation and can last anything from 2-4 weeks. Your physiotherapist will still continue with myofascial release, trigger point release and electrotherapy modalities where needed, but functional rehabilitation is the most important part of this phase.
Depending on your sport, your physiotherapist will tailor specific exercises that will help strengthen the muscles pertaining to your sport. A successful outcome is when you have gained knowledge throughout the rehabilitation program and can participate at full power and speed, not to mention minimizing your chance of future injury.
The medial collateral ligament must be tested under high load and speed to ensure that your knee will be able to keep up with the demands of your sport. During this phase your physiotherapist will guide you to return to normal activities, this includes challenging your knee past its ‘normal’ boundaries to determine how it reacts to different forces. Ultimately we prepare you to return to participating in your sport.
Whatever must be done – we’ll get you there. Jumps, Landing, Sprints, and much more.
Problems we see with medial collateral ligament injuries
Stopping treatment too soon: The pain will return, if the program is not followed until the last week. Patients generally “feel better” after the two weeks of pain management and thus continue on their own with their activities, only to come back after a few weeks with the same problem. The main aim here is not to merely get rid of the pain.
Getting back to sport too soon: Not completing the rehabilitation process can be detrimental to your MCL injury. If you load it too much, too soon, the ligament will not be able to withstand the forces being put on it and you could sustain a re-rupture, starting the whole process right from the beginning, only this time with even more scar tissue to begin with. This can become a recurrent problem and may weaken the ligament to such extent that your knee becomes completely unstable.
Generic braces provide a false sense of security and sometimes athletes will return to sport still using a brace. If the muscles around the knee joint are not strong the brace will not prevent re-injury of the knee.
Waiting too long to come for physiotherapy due to the false sense of support the swelling provides. Swelling makes it more difficult to assess and diagnose the knee completely. (See excerpt on swelling in the knee at general knee ligament injuries)
Not attending to your injury apart from physiotherapy: Your physiotherapist will give you a home program you need to follow. We only see you for an hour maybe twice a week. The rest of the time, it is your responsibility to do what is necessary in order for complete healing to occur.
How long will it take to heal?
Time to recover from a medial collateral ligament injury will depend on the severity of your ligament tear.
A grade 1 MCL injury will take between 2-4 weeks to heal. However, the healed collagen fibers only reach maximal ligament strength after 6 weeks, so to limit the possibility of re-injury it is advisable not to return to sport too soon. If you have to train before 6 weeks it is advisable to use a hinged brace to protect the healing ligament.
If you have a grade 2 MCL injury your recovery time will be between 6 to 8 weeks. With early treatment, we try to get you jogging at 6 weeks, but you should expect return to activity no sooner than 6 weeks.
With grade 3 MCL injuries, your healing time will depend on whether the conservative treatment or surgery option is chosen. Conservative treatment will involve more than 8 weeks of intensive rehabilitation. Initially we will see you twice a week until your pain is under control. Thereafter we will see you once a week to check on the stability and control of your knee. Once you can tolerate everyday activities and control the movement of the knee we will see you once every 10 days or 2 weeks to check on your progress and increase the intensity of your exercises.
Surgery is definitely indicated if a complete rupture of the anterior cruciate ligament is present with medial collateral ligament injury. Full recovery may take 4-6 months and you can only return to sport after 9 months to a year of intensive rehabilitation.
Other medical treatments for a medial collateral ligament injury
- Your doctor can prescribe medication for pain relief.
- Hinged knee braces. With a total rupture of the MCL restriction of certain ranges is necessary to protect the MCL to allow it to heal. This is especially important in the initial phase of healing, but the brace should be removed as the musculature around the knee gets stronger. The limited ranges should also be adjusted as rehabilitation progresses.
- If you have a grade 2 or 3 tear crutches will be useful for a couple of days. At least until you can put most of your weight on the leg and walk without a limp.
- Cortisone injections will help decrease swelling and inflammation, which will help with pain relief, but it does not improve the instability caused by the ligament injury. This is more useful in the case of a chronic MCL sprain, because with an acute injury inflammation is the body’s way of starting the healing process.
It is still necessary to see a physiotherapist after cortisone for proper rehabilitation of the knee. - Biokineticists can help with rehabilitation in the final stages when there is no pain and you have full range of movement. It is important not to start rehabilitation with a biokineticist too soon. If you have pain, stiffness or instability you should see a physiotherapist first.
Surgery for a Medial Collateral Ligament injury
Most MCL injuries do not require any surgery. However, if there are other structures involved (Like ACL or Meniscus) or if you have a rotatory (twisting) instability surgery might be considered depending on the severity. Even with a grade III there is no more advantage to surgery than there is with bracing and proper rehabilitation. In fact, the healing after surgery will take longer than going through the conservative rehabilitation process. Conservative treatment is also non-invasive and less costly that surgery.
What else could the pain be?
- Knee or patellar dislocations – weakness and laxity of your knee joint.
- Medial meniscal injuries – catching during twisting of your knee.
- Anterior cruciate ligament (ACL) tear – you will have pain and the knee will feel unstable going down stairs.
- Knee joint osteoarthritis – deep ache that eases with movement.
- Tibial plateau fracture – deep pain that throbs even when not walking.
- Patellar subluxation/dislocation – unable to walk and pain with full weight bearing.
- Medial knee contusion – no instability with ligament testing.
- Posteromedial corner injury – the pain would be more to the back of the knee.

