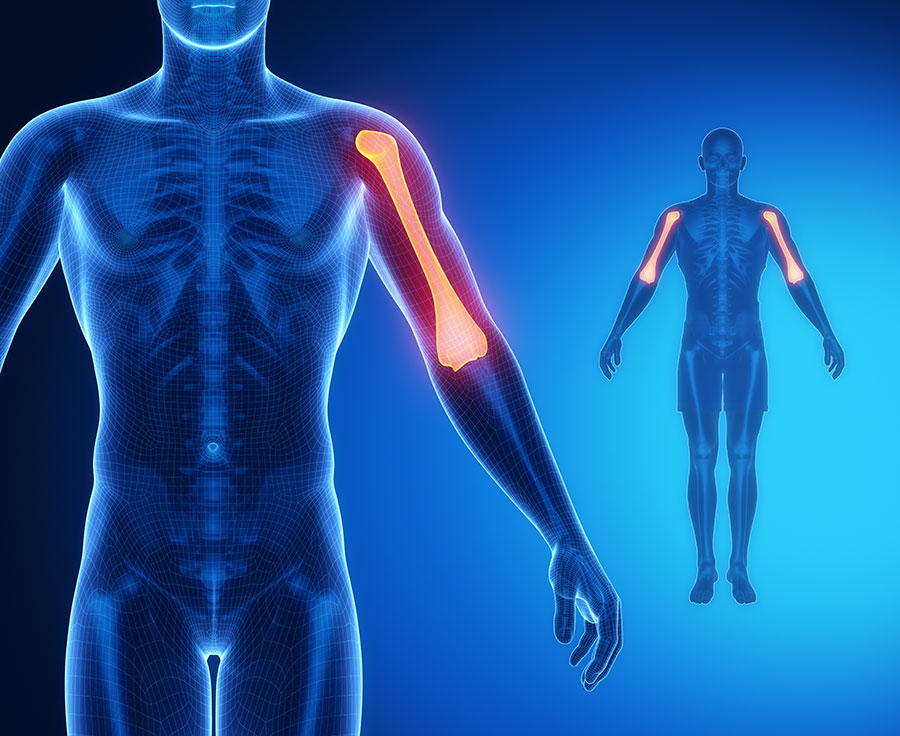
A shoulder joint dislocation is a very traumatic upper limb injury with a good chance of recurring again. Your shoulder joint is a very mobile ball-and-socket joint that consists of your humerus (upper arm bone) that fits snugly into your shoulder joint. When your humerus ‘pops’ out of your shoulder joint, you end up with a dislocated shoulder. Most times, it will lead to an anterior shoulder dislocation. Apart from your shoulder looking deform, the excruciating pain, that worsens when you try to move your arm is actually the least of your worries.
However, the main concern is not that your shoulder joint is painful, it’s about the combination of injuries that comes with a shoulder dislocation. Muscles, ligaments and tendons will all be injured and that will be the root cause of your pain.
Your shoulder stability will be ruined and that is why it is very important to get the right treatment after your shoulder dislocation. The injury will repeat itself if you don’t. Imagine your shoulder ‘popping’ out with something simple like reaching back to the backseat of your car to pick up your bags or even just putting on a jacket.
What does your shoulder joint consist of?
The shoulder joint is a ball-and-socket type of joint. This joint is called the glenohumeral joint. The long bone in your upper arm (humerus) forms the ball and the shoulder blade forms the socket (glenoid fossa). The head of the humerus usually fits snugly into the joint and this allows smooth movement. With a shoulder dislocation, the head of the humerus is forced out of the socket, usually by a traumatic force.
Because the shoulder joint is such a mobile joint, it needs stability. This is where static stabilisers and dynamic stabilisers plays their part.
Static stabilisers
Structures surrounding the shoulder joint that cannot contract or move. These include the joint shape, ligaments, shoulder capsule and the labrum (a fibrous ring of tissue attached to the edge of the socket that increases the depth of the socket). The inferior glenohumeral ligament (IGHL) is the main ligament preventing forward movement of the head of the humerus. Thus, this ligament is very important to prevent an anterior (forward) shoulder dislocation.
Dynamic stabilisers
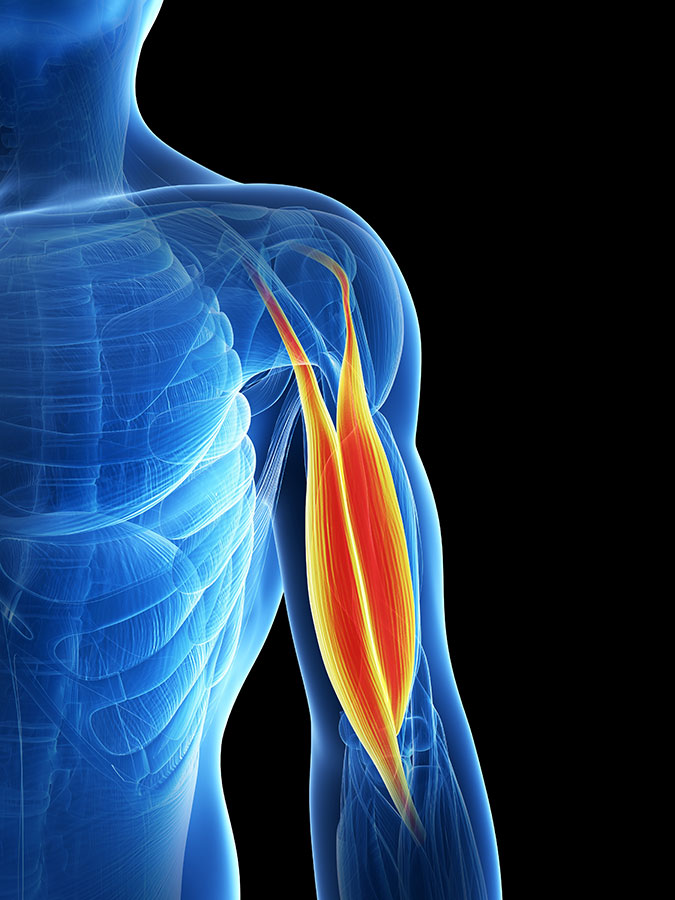
Groups of muscles around the shoulder that provide stability and also movement. The muscles work in force groups or force couples. These muscles keep the head of the humerus in the correct position. The rotator cuff muscles, together with assistance from the shoulder blade muscles and the long head of the biceps muscle are the main dynamic stabilisers. The front part of the deltoid muscle, together with the pectoral muscles and latissimus dorsi also assist in stabilisation of the shoulder joint.
A shoulder dislocation is not only a joint injury, but also an injury to the static and dynamic stabilisers that keep your joint in place. The injury to these stabilisers are just as serious as the joint injury and will need even more attention during your recovery.
What is the function of your shoulder joint?
Your shoulder joint is the one joint in your body with the biggest range of motion. It connects your arm to your upper body and provides your arm with a stable base to move from. Because it is such a mobile joint, you are able to lift your arm, reach out, pick up objects, reach your own face and even reach behind your back.
However, if your shoulder is the base and foundation of movements of your arm, it needs to provide stability as well. If this foundation is wobbly, it becomes unreliable and you’re scared of doing the most simple tasks. It helps you to pick up your kid, unload the holiday bags, tuck in your shirt at the back or helps you to catch on to something when you lose your footing. With an unreliable shoulder you start to think twice about picking up your kid, contemplating if it will ‘hold up’ or handle the weight. That should be enough reason for you to get your shoulder checked out after an injury like this.
How does a shoulder dislocation happen?
Think of your shoulder joint as a round, smooth golf ball that is resting on a tee. This golf ball needs to stay in place for you to complete your swing and hit that ball, to see it soaring through the sky. Your shoulder joint is supported and stabilised by muscles and ligaments as well and just like the golf ball staying in place on the tee, your shoulder joint needs to be stable for you to move (or swing) your arm.
A shoulder dislocation is not just a joint injury
When a traumatic force is applied to your shoulder, big enough to force the head of the humerus out of the socket, it causes a dislocated shoulder. Your body will respond to the trauma of a shoulder dislocation by initiating a massive inflammatory reaction. A dislocated shoulder needs to be placed back into the right position as soon as possible, because this inflammation will lead to swelling and severe pain later on, which makes it harder to manage. Other structures like the static and dynamic stabilisers around the shoulder joint will always be injured as well. Muscles (usually the rotator cuff muscles), ligaments or the labrum can tear, nerves or arteries can be damaged and bones can even fracture.
Muscles
If these stabilising muscles are not strong enough to withstand a force applied to your shoulder, it is so much easier for a shoulder dislocation to happen. They will be overwhelmed and unable to handle the force that is pulling or pushing your arm out of its socket. These muscles are pulled past their limits. This leads to a dislocated shoulder and a muscle injury.
Ligaments
The same counts for the ligaments around your shoulder. If you are very hypermobile or ‘double-jointed’, you naturally have more range than most people. It also means that your ligaments have become lax over time. Now, when a traumatic force is applied to your shoulder, the ligaments won’t be able to withstand it, and it leads to your arm ‘popping’ out of the socket. With ligaments that allow too much movement and that is stretched apart with a shoulder dislocation injury, your shoulder stability will not be what it should be. There is a great chance that this type of injury will happen to you again. Next time, it will happen a lot easier and won’t need as much force.
Subluxation
A partial dislocation (subluxation) happens when the humerus only ‘popped’ out of the socket partially or spontaneously relocates back into position by itself.
A shoulder can dislocate in four directions: Anterior (to the front), posterior (to the back), inferior (downwards) or superior (upwards). The severity of your injury and how you got injured, will determine in which direction your shoulder gets dislocated.
Types of Shoulder dislocations:
- Anterior shoulder dislocation: This is the most common direction in which a shoulder dislocates. It usually happens when you fall onto your arm that is stretched out or when you get a direct hit/tackle onto your shoulder. The head of the humerus will ‘pop’ out towards the front of your shoulder.
- Posterior shoulder dislocation: This is an uncommon form of shoulder dislocation. It usually happens with severe muscle contraction due to seizures or electrical shock or when you fall forward over your bike, directly onto your outstretched arm.
- Inferior shoulder dislocation: This is a very uncommon form of shoulder dislocation. Only with extreme forces, forcing the head of your humerus down and out of the socket, will you get an inferior shoulder dislocation.
It is very important to get your shoulder checked out after a shoulder dislocation. This way, instabilitiy and any other injured structures around the shoulder can be identified and you can get the right treatment from the start.
Causes of a dislocated shoulder
There are several ways in which a traumatic shoulder dislocation can happen to you:
- Falling directly onto your shoulder
- Taking a rugby tackle or any other form of impact onto your shoulder from behind
- Falling onto an outstretched arm that’s lifted sideways and turned outwards
- Severe muscle contraction from a seizure or electrical shock
- A hard pulling force on your arm, pulling your arm out of the socket of the joint
- Getting hit directly onto the front of your shoulder during a motor vehicle accident
If you had a shoulder dislocation once, the chances of the injury repeating itself is big. Instability of your shoulder stabilisers lead to recurring dislocations. If you get to this stage, the simplest of activities can cause a shoulder dislocation to happen again & again. To name a few:
- Reaching out for your handbag from the back seat of your car
- Picking up your kid
- Your dog pulling on its leash when you walk
- Reaching behind your back to put on your bra
- Putting on a jacket
Symptoms of a dislocated shoulder
How bad is my shoulder dislocation?
Your shoulder can either be partially dislocated (subluxated) or fully dislocated. A shoulder dislocation is a traumatic injury and will always involve not only your shoulder joint, but the other soft tissue structures around your shoulder as well. The amount of other structures that gets injured will depend on the type of injury and the direction of dislocation.
Typical soft tissue injuries with an anterior shoulder dislocation:
- Bankart lesion: Damage or tear of the labrum at the front edge of the socket. If a piece of the bone breaks off together with the labrum, it is called a bony Bankart lesion.
- Damage to the shoulder ligaments (especially the ligaments at the front of your shoulder joint).
- Hills-Sachs lesion: A compression fracture at the back of the head of the humerus.
- SLAP lesion: A tear of the labrum.
Posterior or inferior shoulder dislocations aren’t as common, but can cause the following soft tissue injuries:
- Damage to the inside of the shoulder joint, including fractures and extensive ligament damage.
- Rotator cuff muscle tears.
- Damage to arteries and nerves. Damage to the axillary artery and the axillary nerve may result, together with other nerves that form part of the brachial plexus. Nerve damage will lead to a weak or paralyzed deltoid muscle, which leads to difficulty in lifting up your arm. It will also cause extreme and burning pain, pins and needles and numbness. If an artery is damaged, it will lead to your hand becoming cold and pale.
There is a possibility that when your shoulder is reduced (put back into position) after a shoulder dislocation injury, a nerve or artery can be injured or ‘pinched’. So, even after you have been helped and your shoulder joint is in a normal position again, you can still struggle with other soft tissue structures that have been injured. It is very important that you get a full evaluation after a shoulder dislocation to be able to get the right treatment from the start.
Shoulder dislocation again & again
The risk of getting a shoulder dislocation again increases each time it happens. The static and dynamic stabilisers that are supposed to improve your shoulder’s stability, gets weaker and ‘looser’ with each dislocation. With time, your shoulder becomes very unstable. This can lead to spontaneous and recurring shoulder dislocations that happens without an injury causing it. So, the focus must shift from correcting the dislocation, which is only the first step. These static and dynamic stabilisers must be checked and fixed before your shoulder pops out again.
Diagnosis
Physiotherapy evaluation
Our physiotherapists are experts in human anatomy and movement with the necessary experience to diagnose shoulder dislocations very easily. We understand the intricacy of the shoulder joint and can accurately diagnose which other soft tissue structures have also been injured. A clinical assessment and getting the necessary information about the injury is the starting point.
During your physiotherapy evaluation, we will stretch and stress the shoulder joint as well as the shoulder labrum and muscles and ligaments in the area. We also test muscle strength and length, range of movement and can measure swelling in the area. An anterior or inferior shoulder dislocation is often easy to identify by just looking at your shoulder. Our physiotherapists are the best at diagnosing this type of problem.
If your physiotherapist suspects that you have a shoulder dislocation, you will have to get an x-ray taken of your shoulder and you will have to have your shoulder reduced (have it put back in position).
X-rays
Your physiotherapist will refer you for an X-ray if you have a suspected shoulder dislocation. The bones that form part of your shoulder joint will be visible on an x-ray. The x-ray will show the position and direction of the dislocation and it is very important to exclude any possible fractures. An x-ray needs to be taken before and after your joint is reduced. This way, it will determine if your shoulder joint is back in the right position and exclude any further bone damage. It can be hard to see a posterior shoulder dislocation on an x-ray, but changing the position from which the x-ray is taken can help. Anterior shoulder dislocations are more common and easier to see on an x-ray.
Diagnostic Ultrasound
Doing a diagnostic ultrasound will not be very effective to diagnose a shoulder dislocation. It will not be able to provide the necessary images of what is going on deep inside your joint. However, it could be effective in showing more superficial muscle tears. If your physiotherapist feels that you have possibly torn one of the muscles around your shoulder, you will be referred to get a diagnostic ultrasound. This will only happen after your shoulder has been successfully reduced and after the necessary x-rays has been taken.
MRI or CT scan
A CT-scan is recommended if your x-rays showed that you have a fracture, especially around the rim of the shoulder joint. An anterior shoulder dislocation can cause a fracture to the rim of the glenoid fossa or a fracture to the posterior head of the humerus. The CT-scan will be able to determine the size of such a fracture.
A MRI-scan will show any soft tissue injuries, even injuries deep inside the shoulder joint like a labrum tear.
These scans are very expensive and you will need a referral from an orthopaedic specialist. Your physiotherapist can refer you to the right specialist to get the right scans, if necessary.
Why is my pain not getting better after I had a shoulder dislocation?
Let’s say you had an anterior shoulder dislocation, which was reduced when you went to your doctor and after that you felt much better. Immediately after your shoulder was put back in place, you felt relieved and could move your arm again. Initially, you rested your arm and took some medication, but now you find that your pain is not improving as you had hoped.
Without a proper evaluation and treatment plan, your shoulder pain won’t simply improve. The trauma of a dislocated shoulder, is severe. It will take at least 6 weeks for your body to work through the complete cycle of recovery and healing.
Now, imagine that after a week or two you feel good enough to return to your training or sport. If your body has not had the chance to heal and strengthen all the structures that got stretched open during your shoulder dislocation, it will not be ready to cope with the load of picking up anything heavy or throwing a ball. It will only contribute to cause more trauma and keep you in a cycle of continuous pain.
Simply resting your arm or keeping it in a sling for a few weeks will not be a solution. After resting for such an extended period of time, your muscles would have become weak and your shoulder joint stiff.
Addressing the bigger picture and everything that got injured through a proper rehabilitation program, is the only way for you to improve and to prevent dislocations from happening again in the future.
What NOT to do
What you should do
Making the feeling of instability worse
A big problem we see with dislocated shoulders
A common problem we see is that patients wait too long before they seek help after they’ve had a shoulder dislocation. By the time patients come to see us, they have had shoulder pain and problems for months. Now, the shoulder has become unstable, muscles have become weak and you are stuck in a cycle of pain and dysfunction. Recovery will take so much longer.
Often, patients try to take anti-inflammatory medication in the hopes of decreasing their pain. This, however, only slows the process of healing. Initially you will have to take pain medication to ease your pain, but medication won’t help for your shoulder’s instability. You are not addressing the root of the problem by simply taking medication. The only way to address your pain and instability will be to look at every structure that got injured and get the joint stable again.
Long-term use of a sling is another problem we see. Using a sling or brace, will support your shoulder and give it the necessary rest. However, long-term use of a sling like this will only lead to you getting used to it. It will lead to weakness and stiffness and this in turn will lead to other problems that will only increase your recovery time.
Physiotherapy treatment
We are confident that we can provide the best possible treatment after you’ve had a traumatic shoulder dislocation and if you struggle with recurring instability and dislocations. Patients are often anxious to get back to their normal activities and that is why we are here to provide guidance and answers to ease your fear. We’ll implement a very effective and structured plan of action that treats all the aspects of the problem. This way your shoulder stability will improve and you’ll be able to move and exercise with confidence again. However, it’s important that you commit to the treatment plan after you had a shoulder dislocation, as this improves your chances of successful long-term recovery.
The basic structure of our treatments:
- Determine what has been injured
- How bad is it injured?
- Protect it from further injury
- Give it time to heal
- Strengthen surrounding muscles
- Re-evaluate to monitor progress
We will be looking at different aspects, like testing and measuring your ability to functionally use your arm. And we will also look at other aspects like muscle strength, range of motion, flexibility and stability. Treatment techniques will include: soft tissue massage, joint mobilisations, dry needling, strapping, laser therapy, nerve mobilisations and guiding you through a rehabilitation program of gradual strengthening, control and conditioning of the muscles around your shoulder.
Phases of rehabilitation
1st Phase: Protection & initial Healing
Protect
We have found that patients tend to continue using their injured arm after a shoulder dislocation. This means that the injured shoulder joint and muscles still has to carry the load each time that you use your arm or pick up something. It is better to put your arm in a sling for at least the first week after your injury (this will depend on the severity of your injury). This way your shoulder joint is stabilised and protected.
Rest
Rest from activities that is worsening your pain, training or taking part in sport. Use a sling to decrease the work that your arm and shoulder needs to do.
As soon as there’s no pain, don’t test it. Give it time to heal.
Ice
Ice cubes wrapped in a towel, tied around your shoulder reduces pain & inflammation. For at least the first 2 days or until the swelling goes down, apply an ice pack onto your shoulder every few hours. Always keep a towel between the ice and your skin (to prevent freeze burn).
Compress
Use strapping or an elastic compression bandage tied around your arm and shoulder, to keep your shoulder joint supported. This can be done either with taping or tube grip bandage and it helps to control swelling and reduce pain.
Elevate
It might be a bit hard to elevate your shoulder, but if your arm or hand becomes swollen after having a dislocated shoulder, you could elevate your arm. Lie on your back with your arm on a few pillows beside you (your arm must be higher than your heart to allow gravity to assist in draining the fluid away).
2nd Phase: Establish pain free range of movement
Depending on the severity of your injury, you will have to immobilise your arm in a sling for the first 6 weeks after having a dislocated shoulder. Even during this time your physiotherapist can start with the treatment process by doing passive movements. Your wrist, elbow and shoulder will need to be moved, gently at first, but this way your joints won’t become severely stiff. Over time it will become clear which movements you are able to do, and which ones you should avoid. There is a pain free range of movement that you’re safe to move in, and our exercises will be targeted between these boundaries.
As you progress through your treatment plan, we aim to gain a larger pain free range of movement while your painful range becomes less intense.
3nd Phase: Tissue healing
We monitor the progress of healing of all the structures that got injured with your shoulder dislocation. On a cellular level we’re able to accelerate tissue healing by stimulating a healing response in your body, using dry needling, laser, ultrasound and electrotherapy. Finding the balance between rest and movement is important for optimal tissue healing to take place. We can give you the best advice on this matter.
4th Phase: Tissue Stress & muscle activation
During each session we will re-evaluate to see if you are achieving the necessary targets for the tissue to be able to handle tensile, elastic and compression forces. We use isometric muscle contractions to help the muscles and surrounding soft tissue get used to movement. This type of muscle contractions are muscle contractions without momentum. This way, muscles around your shoulder stay active without compromising your injury site.
5th Phase: Active full range of movement
Before you can start strengthening your muscles, you need to be able to move your arm and shoulder through the full range of motion. Remember, your shoulder joint is very mobile, so there will be many movements to work on. During this phase of your treatment, we will start to stretch and push your joint into the end of the range. Any scar tissue that formed inside the shoulder joint or around other injured structures must be lengthened and orientated to allow the soft tissue to move and muscles to contract without any restrictions. We use massage, stretches and neurodynamic mobilizations to achieve full range of movement.
On completion of this phase you should be able to move your arm in all directions. Previously, you might have felt anxious about your shoulder ‘popping’ out when you put your arm behind your back. Now, after completing this phase of treatment, you’ll be able to fasten your bra behind your back without thinking twice.
6th Phase: Muscle Strength
It is common to feel some pain when you start contracting muscles that haven’t moved in a while. This is due to breaking down of abnormal fibrous tissue adhesions that restrict movement. However, to get your shoulder joint stable again, it’s very important to strengthen the muscles in your arm and around your shoulder. During this phase you will start to do exercises with resistance.
7th Phase: Shoulder stability and control
During this phase of your treatment plan, you will continue with strength training. However, the exercises will be adapted and progressed so that you are working on control of your movements more. Eccentric muscle exercises as well as using your own body-weight and putting weight on your shoulder helps to improve stability. Lifting, pulling or pushing will be much easier to do and you won’t feel anxious about your shoulder not holding up anymore
8th Phase: Returning to normal activities
Gradually, we will help to build you back up to take part in your normal activities and training at your normal intensity. This way we determine if your shoulder joint is stable enough to withstand repetitive loading without flare-ups. Your physiotherapist will guide you to re-engage in your routine in safe increments, and help with adjustments where necessary. We’ll get you back to work, back to driving or back to your hobbies.
9th Phase: High Speed, Power, Coordination
Your shoulder movements must be tested under high load and speed to ensure that the stability of the joint and the muscles are able to keep up with the demand of your body. During this phase your physiotherapist will guide you to return to your normal activities, but also challenge your muscles past their ‘normal’ boundaries to determine how it reacts to different forces. Your shoulder stability will be put to the test in a big way. Ultimately we prepare you to return to participating in your sport.
Whatever must be done – we’ll get you there. Pushups, throwinging, pushing and much more.
10th Phase: Sport Specific Training
This is the final stage of treatment after your shoulder dislocation. Your physiotherapist will still continue with myofascial release, trigger point release and electrotherapy modalities where needed, but functional rehabilitation is most important during this phase.
Depending on your sport, your physiotherapist will tailor specific exercises that will put your shoulder stability to the test and help strengthen the muscles you use most in your sport. A successful outcome is when you have gained knowledge throughout the rehabilitation program to understand your injury and if you can now participate at full power and speed, not to mention the benefits of minimizing your chance of a recurring injury. Swimming, boxing, bowling or doing pull-ups ups are all things we want you to be able to do again without pain or fear.
How long will it take to heal?
Depending on the severity of your injury and which other soft tissue structures got injured, your normal phases of healing takes about 6 weeks. A dislocated shoulder is a very traumatic type of injury, whether it is an acute traumatic dislocated shoulder or a recurring dislocation. Your whole joint was stretched open. It will affect the stability of your shoulder and needs to be fixed.
Initially, you will need treatment twice a week for two weeks, after which the treatment sessions can be spread out to one each week. You only spend an hour at a time getting physiotherapy treatment. The rest of the work will be up to you to do at home. We will give you enough time in between each session to spend time on your exercises. If you would like to get back to playing sport, that will increase your recovery time by another few weeks to months.
Getting back to a fully functional level and actively participating in sport after a shoulder dislocation will take you 3 months to 6 months.
If you had other soft tissue injuries or fractures together with your shoulder dislocation, it will take longer to heal. This increases your recovery time. It is important that you follow through with the treatment plan after your shoulder dislocation. This way you will prevent it from happening in the future again.
Other forms of treatment for your shoulder dislocation
- Medication: Initially, you will need pain and anti-inflammatory medication to decrease your pain. Anti-anxiety medication may be prescribed for the emotional stress associated with a dislocated shoulder. However, long-term use of these medications are not good for your health and anti-inflammatory medication will simply suppress the healing process. Taking medication for a long period after your shoulder dislocation injury, won’t be the solution to your problem, especially if other structures got injured and you are not getting the necessary treatment for it.
- Cortisone injections: Your doctor might suggest that you get a cortisone injection if your pain persists after you had a shoulder dislocation. This could ease the discomfort and pain of any inflammation that could still be going on. However, long-term use of cortisone is not good for the integrity of your joints.
- Wearing of a sling: The emergency doctor, or GP will suggest you make use of a sling to give your arm the necessary rest. However, even if you have to wear the sling for a few weeks, physiotherapy treatment can already start. Your physiotherapist can assist you by moving your arm passively and preventing severe stiffness. The use of a sling is not a permanent or long-term solution. With time, your arm will get used to it, and get weak. Active rehabilitation is still needed.
- Getting a manipulation done: After having a dislocated shoulder, your shoulder might feel stiff. Almost as if you need to ‘click’ it back in. Getting a manipulation or re-alignment done is not a good idea at this stage. Your shoulder is already unstable after a dislocation, a manipulation could worsen this.
- Seeing a biokineticist: When you have worked through your treatment plan with your physiotherapist and you need help with further rehab, a biokineticist will be valuable to help you get stronger.
Is surgery an option?
Acute traumatic dislocated shoulder
If your shoulder cannot be reduced back into its neutral postion, it might need to be done in theatre by an orthopaedic surgeon. If you have torn muscles, a torn labrum, torn ligaments or a fracture, you will need surgery. This will be seen on an x-ray or on a scan and you will need to be referred to an orthopaedic surgeon as soon as possible. With surgical repairs, it is best to operate within 2 weeks of your injury, because the condition of your soft tissue is still optimal.
Depending on the type of dislocation and the type of surgery done, you will need rehabilitation after surgery. Your surgeon might not permit certain movements or movements against resistance, and you may have to wear a sling after your surgery. However, it will be in your best interest to see your physiotherapist during this time of recovery. Even if you have to wear a sling, your physiotherapist can help you by passively moving your shoulder and preventing any joints from becoming stiff. This way, when your orthopaedic surgeon allow you to start moving, your physio is up to date and ready to start treatment.
Chronic recurring dislocated shoulder
If you get to a stage where your shoulder has dislocated repeatedly, it becomes very unstable and dangerous. You will probably need surgery to try and improve the stability of your shoulder.
What else could it be?
- Fractures of bones around the shoulder – Usually due to direct trauma. You will have pain whether you move or not, but it will be worse when you push on your arm.
- Arthritis of the shoulder – Pain and stiffness of your shoulder. It feels worse with cold weather and when you get up in the mornings.
- Rotator Cuff Injury – An injury to the muscles around your shoulder. Usually due to overuse, lifting something too heavy or forceful throwing.
- Acromioclavicular (AC) Joint Dislocation – This happens due to a direct blow to the shoulder or falling directly onto the shoulder. The front of your shoulder might look ‘abnormal’.
- Shoulder labrum injuries – Pain in the shoulder that includes ‘clicking’ or ‘popping’ noises or your shoulder feeling stuck in one position.
- Axillary nerve injury – Pain accompanied by pins and needles or a loss of sensation around your shoulder. Lifting your arm sideways will be hard or impossible to do.