Intense pinching pain when you simply bend down to brush your teeth. Getting up from a chair and straightening your back gives you such severe pain that your legs feel weak and wobbly. You don’t want to move your leg, because you know how much pain will be spreading down your whole leg and all the way into your toes. Your whole leg feels useless, numb and weak. These are all symptoms of sciatic nerve pain, caused by a pinched sciatic nerve or sciatic nerve injury.
The sciatic nerve is the largest, thickest and longest nerve in your body that runs from your lower back all the way down your leg to your foot. That’s why the severity of sciatic nerve pain will drive you mad if you don’t find the cause and root of the problem. Severe compression of your sciatic nerve can cause permanent irreversible damage and that is why it is important to get the right treatment from the start.
The structure of your sciatic nerve
The sciatic nerve starts out in your lower back and follows its path down your leg all the way to your foot. It runs through openings between your vertebrae, past intervertebral discs and beneath layers of muscles. The nerve can become trapped at any of these points and give you sciatic nerve pain. Our job is to determine the exact site of compression to the nerve along its pathway. Let’s start by looking at the structure of your lower back, where it all starts.
Your spine, the place where it all starts
Different bones (vertebrae) stacked on top of each other form your spine. Each vertebra has a number, according to the level. The vertebrae forming your lower back is numbered L1 – L5 and just below it S1 – S5. Between each bone, there is a disc, made up of a gel-like substance. They act as shock absorbers and without them, your vertebrae would grind against each other with every movement. With the discs in place, there is enough space between each bone and it creates openings for nerves to exit from. Strong ligaments connecting every bone in your spine, give your spine enough stability. Muscles connecting to your spine, give you the ability to bend in any direction. Nerves connect all these structures and stimulate them to move.
A network of nerves
Your spinal cord is a thick cord of nerves that runs from your brain down to the lowest part of your spine. The space between each vertebra form an opening from which a nerve root exits on each side. Nerve roots form pathways that form a whole network of nerves throughout your body.
Nerves are like the power cables in your body, connecting different parts of your body together. This network of power cables provides the power that allows you to move and feel.
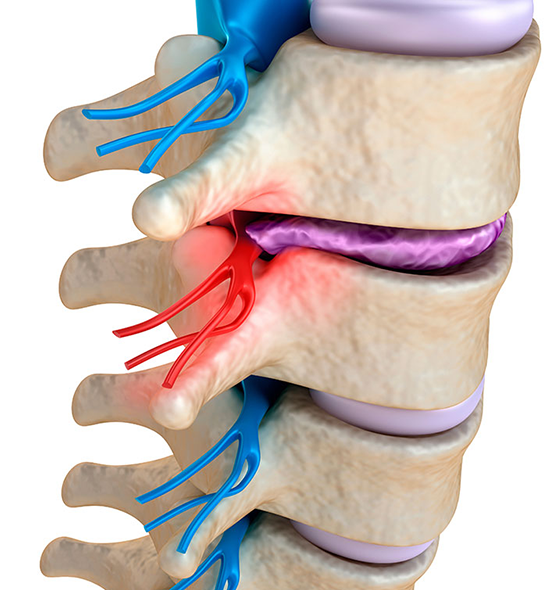
Your sciatic nerve is formed by nerve roots
The sciatic nerve is the largest nerve in your body. Level L4 to S3 nerve roots are bundled together to form a new thick (almost as thick as a man’s thumb) power cable called your sciatic nerve. On each side and it runs all the way from your lower back, deep through your buttock, down the back of your thigh and all the way to the heel of your foot.
At the back of your knee, it divides into two new branches called the tibial and peroneal nerves.
- Peroneal nerve: The peroneal nerve is a more superficial nerve that travels sideways along the outer part of your lower leg and down into the upper foot.
- Tibial nerve: The tibial nerve continues deep into the calf and travels downward toward the heel and sole of the foot.
Nerve insulation
Your sciatic nerve, just like all other nerves in your body, is covered by protective layers and sheaths, namely the myelin sheath. The purpose of the myelin sheath is to act like a good layer of insulation, improving your nerve’s ability to conduct impulses. The layers covering your nerve protect it and allow the nerve to glide inside it. As you move your leg, your sciatic nerve needs to be able to move and glide with you without getting overstretched or stuck somewhere.
A network of small, fine arteries provides the outside sheath with enough oxygen and nutrients. Just like all other tissues in your body, nerves need oxygen to be able function. Other tissues can survive for a very short while without blood supply, but nerves are extremely sensitive to compression and a loss of circulation and oxygen. Ultimately, this is what causes nerve pain. It acts as a warning that the nerve is not getting enough oxygen and this could lead to nerve damage.
Variations in the sciatic nerve
The structure of your sciatic nerve could be different from the next person. Instead of passing between the different layers of your buttock muscles, your sciatic nerve could divide and one part then passes through a buttock muscle called the piriformis muscle. Even though a variation like this is considered normal, the portion passing through the piriformis muscle can be compressed a lot easier by the movements of the muscle.
What is the function of your sciatic nerve?
Nerves act like power cables that give impulses of energy. This energy allows your body to move and allows you to feel different sensations like soft touch, pressure, temperature, and pain. Your sciatic nerve is the power cable that connects the skin and muscles of your thigh, leg and foot to your spinal cord, the main power source.
The part of the nerve that supplies energy to muscles is called the motor function and the part that supplies the ability to feel is called the sensory function.
Motor functions of the sciatic nerve:
- Knee flexion: Bending your knee
- Hip adduction: Bringing your thighs together
- Plantarflexion: Pointing your foot downward
- Toe flexion: Bending your toes downward
- Dorsiflexion: Lifting your foot upward
- Toe extension: Pulling your toes upward
If your sciatic nerve is pinched, you will feel one or more of these movements as clumsy and weak.
Sensory functions of the sciatic nerve:
The sciatic nerve allows you to feel different sensations in your leg in very specific patterns called dermatomes. Different nerve roots supply different dermatome levels down your leg. The following areas are the dermatomes for L4 – S3 (the nerve roots that form your sciatic nerve):
- Front, back, and outside of your thigh
- Front, back, and outside of your lower leg
- Top and outer side of your foot
- Sole of your foot
- The web between your first and second toes
Your skin feels ‘abnormal’ when your Sciatic nerve is irritated or pinched. That can range from burning, tingling, pins and needles, numbness or sharp electrifying pain.
Why do I feel sciatic nerve pain?
Pain serves to warn and protect you that something is wrong in your body. The same can be said of sciatic nerve pain. When the sciatic nerve is either irritated, pinched or compressed, it causes sciatic nerve pain. The sheath around the nerve that provides it with blood supply and nutrients is compressed, disrupting the blood flow. The pain that you then feel is a message saying something is wrong. Nerves are very sensitive structures and if the source of irritation or compression is not found, it can lead to nerve damage.
Stretch-related sciatic nerve pain
Nerves are flexible, but not as flexible and elastic as muscles. They can not lengthen or shorten like muscles but can move and glide with muscles and other layers of tissue and skin. When a stretch or traction force is applied to your sciatic nerve and it is too strong, injury occurs, overstretching and possibly tearing the nerve. If this happens continuously it could lead to nerve damage. Compare this to the action of tugging on a power cable. Eventually the cable starts to fray and tears apart or disconnects from the socket, leading to a disruption in the flow of power or damage to the power cord.
Sciatic nerve irritation:
Imagine your phone’s charger cable being rubbed over the edge of your desk over and over again. With time, the intense friction will cause the power cable to fray. The next time you charge your phone, sparks will fly. Your sciatic nerve can be irritated in the same way. The friction between the nerve and the tissues around it causes a point of irritation. Sciatic nerve irritation sparks a sharp and sudden electrical shock type of pain that runs down your leg. Even though the nerve is irritated only at one certain spot, it causes pain down the length of the nerve. If the point of irritation can be relieved, the sharp and shocking pain is relieved. Usually, certain positions or movements bring on the pain.
Sciatic nerve compression (pinched sciatic nerve):
Pinching and compression on your sciatic nerve not only reduces proper blood supply to the nerve, it also delays the messages or signals sent through it. The ability of your sciatic nerve to transmit impulses and send messages to your spinal cord and brain is reduced if it is pinched somewhere along the line. Initially, compression on your sciatic nerve leads to a burning or sharp pain down your leg that doesn’t ease. With more severe compression, the current of signals travelling through your nerve is reduced. This leads to clumsiness and weakness and your skin feeling completely numb. Leaving a heavy box on top of your internet cable will lead slower internet speed and poor internet signal. With sciatic nerve compression, you will feel much the same. Like you’ve lost power and like you can’t control the movements that you want to do with your hip, knee or foot.
Different nerve roots, different area of symptoms
Your sciatic nerve consists of different nerve roots running directly from of your spinal cord (L4-S3). If the area of irritation or compression is on only one nerve root, only the area (dermatome) where that nerve root runs to, will produce symptoms. In our experience, usually more than one nerve root is affected, leading to the feeling of your whole leg feeling pain.
A cycle of inflammation
The constant friction, irritation and overstretching of your sciatic nerve causes inflammation. Swelling sets in, increasing the pressure on the nerve. The next step is muscle spasms of the muscles in your back, buttock and leg. Your body is trying to protect you and prevent you from moving too much or irritating the sciatic nerve any further. Now, with the severe pain and stiffness that you’re feeling, the smallest movement becomes too painful to do. And when you do it, it irritates and stretches the nerve, stimulating more inflammation, and it keeps the cycle going. Simply bending down to brush your teeth or wash your face now sends you through the roof.
Continued irritation leads to compression. Initially, you feel pain only with certain movements or positions, but as the nerve starts to get compressed your symptoms change. Now, your leg starts to feel clumsy and weak, with patches of numbness and you have constant burning pain. Compression of your sciatic nerve is very serious and if the compression isn’t relieved as soon as possible, it leads to permanent nerve damage.
What is the difference between sciatica and sciatic nerve pain?
Sciatica is a broad term used to describe the symptoms that you feel due to pain that originates from the lumbar and/or sacral nerve roots. So, with sciatica you will feel pain and symptoms like pins and needles and/or numbness and weakness in the area of your sciatic nerve, but it won’t be caused purely by your sciatic nerve. It is only the symptom of an underlying condition. That is why sciatica and sciatic nerve pain have characteristics that overlap, but it is not the same thing.
Causes of sciatic nerve pain
It is very important to understand and find the cause of your sciatic nerve pain. This way, the root of the problem can be addressed, rather than just getting treatment for the symptoms of the nerve pain.
Herniated disc
A disc in your lower back may bulge or herniate, pushing out to the side and putting pressure on nerves. Sitting for long hours, bending and driving in a car increases the pressure on the herniated disc, which in turns increases the compression of your sciatic nerve.
Spinal stenosis
Stenosis or narrowing of the intervertebral opening through which a sciatic nerve root runs. It leads to compression of your sciatic nerve especially when you do certain movements like bending backwards.
Degeneration of the spine (osteoarthritis)
Degeneration of your joints happen as you age. It leads to the formation of bone spurs (osteophytes), thickening of facet joint capsules and thinning discs that may directly compress your sciatic nerve.
Segmental instability
Instability of a joint in your spine (vertebral segment) occurs if one vertebra slips over the one below it (spondylolisthesis). This can compress the sciatic nerve.
Traumatic injury to your lower back
Falls, motor vehicle accidents or a direct hit to your lower back can cause fractures of your spine or soft tissue injuries, which in turn leads to inflammation, irritation and compression of the sciatic nerve.
Chemical irritation/inflammation
Inflammation is a chemical process that takes place in your body after an injury. It causes swelling and this in turn can irritate your sciatic nerve, depending on the area of inflammation.
Sciatic nerve entrapment or tethering
As the sciatic nerve runs from your lower back, through layers of buttock muscles, down through layers of thigh and calf muscles, there are various areas where it can become entrapped. The soft tissues and muscles around your nerve are called the mechanical interface and can prevent the normal gliding movement of the nerve. The most common area of entrapment is when a muscle next to the sciatic nerve becomes tighter, less flexible or overworked. Common examples of muscles that cause entrapment is your hamstring and piriformis muscles.
Piriformis syndrome
Contraction or movement of the piriformis muscle (situated in your buttock) can irritate or pinch your sciatic nerve. It happens when the muscle spasms and becomes tight, disrupting the flexibility of the mechanical interface. It happens even more commonly in individuals where the sciatic nerve splits and one portion passes directly through the piriformis muscle. Even though sciatic nerve pain is a symptom of piriformis syndrome, it will be vital to find the cause as to why the piriformis muscle has become overworked or tight.
Direct traumatic injury to the sciatic nerve
Stab wounds, falls, fractures, failed surgeries or motor vehicle accidents are some of the things that can directly injure or lacerate your sciatic nerve anywhere throughout your leg, depending on where the injury takes place.
Individual traits
Posture, weight, fitness, pregnancy and leg length are a few things that could increase your risk of a sciatic nerve injury.
Occupation
People with certain occupations may be at a higher risk of developing sciatic nerve pain. In general, sitting or driving for long periods of time without proper posture or frequently moving the spine can be a contributing factor to sciatic nerve pain.
Vitamin B12 deficiency
Vitamin B12 is important for maintaining good nerve health and to maintain the sheath that covers nerves, which is important for nerves to function and conduct impulses.
Tumors
Tumors that form in the bones of your spine, next to your spine or anywhere down your leg can compress the sciatic nerve.
Infections or abscesses
Certain diseases like septic arthritis or TB spine can cause an abscess and area of infection and swelling in your spine. This can lead to compression of the sciatic nerve.
Symptoms of sciatic nerve pain
How bad is my sciatic nerve injury?
It starts out with a tingle down your leg when you bend down to put on your shoes or some pain down your leg when you’ve been sitting in your car for a while. However, once you start moving again, the feeling goes away and you forget about it for a while. This is what we call intermittent irritation of your sciatic nerve. In certain positions, like bending, it gets overstretched and irritated, causing you pain.
The irritation becomes worse
With time, this intermittent irritation of the sciatic nerve gets worse. Especially if you do nothing about it. You realise your back is getting stiff, preventing you from bending or sitting and more often than not, you start to feel a sharp pain spreading down your leg. Time goes by and now the pain bothers you constantly. You feel that certain patches of skin on your leg and foot feels numb and dead. Your leg is getting weak and there has been a few times where you felt your knee giving way beneath you.
Now, the intermittent irritation that only bothered you at times, has progressed to sciatic nerve compression. The nerve cannot properly conduct impulses anymore, leaving you with a painful, weak and numb leg. Your sciatic nerve pain has become so severe that it is is affecting your life, sleep, work and exercise.
It gets serious
Pinching or compression of your sciatic nerve will lead to nerve damage over time. The pain from this is so severe, you will feel like you don’t want to move at all. This pain serves as a warning. Your sciatic nerve is slowly dying, because it is not getting enough oxygen. Weakness or clumsiness of your leg will become permanent if the nerve is damaged.
Chronic, recurring pain
Chronic or recurring sciatic nerve pain can lead to nerve damage in the long run. Finding the true source of your sciatic nerve pain is the best way to clear up sciatic nerve pain or to prevent chronic pain from flaring up again. The sooner the problem can be identified, the better. The longer you have sciatic nerve pain, the higher your chances become of having nerve damage.
Sciatic pain can even affect both legs at the same time or it can alternate between sides with each flare-up. That will depend on the main cause of the pain.
Worst case scenario
If the sciatic nerve has been damaged, the severity of nerve damage can be classified as follows:
- Neuropraxia: The sheath around the nerve gets damaged, which helps with the conduction of impulses. This usually happens due to a compression type of injury. It leads to pain and reduced conduction ability of the nerve, but it can still heal if the source of compression is relieved soon enough.
- Axonotmesis: The sheath of the nerve is still intact, but the inside cord has been severed or has snapped. This however, is still the optimal circumstance for healing to take place, because the sheath that provides circulation and nutrients is still intact. A stretching type of injury will cause this type of damage, where too much traction was applied, snapping the inside of the cord.
- Neurotmesis: Complete disruption of the whole nerve. The nerve is now split in two, and the two parts of the nerve is not connected anymore in any way. This is a severe injury and happens mostly due to traumatic type of injuries such as stab wounds or lacerations.
Diagnosis
Physiotherapy diagnosis
Our physiotherapists are experts in human anatomy and movement with the necessary experience to diagnose sciatic nerve injuries very easily. We fully understand the intricate way nerves work and can accurately diagnose which structures are causing your sciatic nerve pain. A clinical assessment and getting the necessary information about your pain is the starting point.
During your physiotherapy evaluation, we will stretch and stress the sciatic nerve as well as structures in your lower back, hip and knee. We also look at the mechanical interface, which is all the layers of tissue and muscles surrounding the nerve. Your sciatic nerve should be able to glide and move between these layers of tissue. For this we use neural tension tests and with it we can pinpoint the location of irritation or pinching of the nerve.
Movement and sensation:
Your sciatic nerve is responsible for two important things. Movement and sensation. Testing movement (motor function) will involve testing all muscles surrounding the sciatic nerve, by looking at muscle strength, length, reflexes and range of movement. To test your sensation, we will test your ability to feel soft touch, sharp pain and different temperatures.
Thorough evaluation makes our physiotherapists the best at diagnosing this type of problem.
X-rays
Soft tissue, like discs and nerves cannot be seen on x-rays. X-rays show the integrity and alignment of the lumbar spine and vertebrae. This will enable us to see if something is wrong with the structure of the vertebrae or if there is a loss of disc space. This way, we can see if the source of your sciatic nerve pain comes from your lower back.
Your physiotherapist will refer you to get x-rays taken if deemed necessary.
MRI
An MRI will show all of the structures of your lower back and pelvis, including soft tissue like nerves. It will show exactly where the sciatic nerve is being pinched and what is pinching it.
An MRI is an expensive test and you need to be referred by a specialist to get one. If you have already had an MRI done, please bring it along to your first consultation. If your physiotherapist feels it is necessary for you to get an MRI, you will be referred to a specialist.
Diagnostic ultrasound
Diagnostic ultrasound is effective in showing different layers of soft tissue. It will show areas of compression, but it it is not as effective as an MRI to image deeper areas. If deemed necessary, your physiotherapist will refer you to get an ultrasound.
Nerve conduction studies
- Electromyogram (EMG) – This is a test where needles are inserted into the muscles that the sciatic nerve supplies. It measures the electrical activity produced by these muscles. The electrical activity of the nerve will be tested when you contract and relax your muscles. This test can determine if there are any areas of nerve damage.
- Electroneuromyography (ENMG) – This test examines both the sensory (feeling) and the motor (ability to contract or relax muscles) function of the nerve. It will show the conduction velocity of impulses through your sciatic nerve between 2 points. It is considered abnormal when the impulse travels slower, and weakens between 2 points. This could be an indication of nerve damage.
These tests are expensive to do, and can only be done by a specialist like a neurologist. If your physiotherapist feels it is necessary for you to get these tests, you will be referred to a specialist.
Why is my sciatic nerve pain not going away?
Let’s say you have had sciatic nerve pain before and had treatment for it. Taking medication and resting helped, because the pain improved. However, now you want to get back to exercising or back to your day to day activities, but your pain keeps coming back. Now, each time you bend forward you wonder if it might trigger that familiar burning pain down your leg. Or each time you drive for long hours, you start to feel the familiar tingle in your foot.
Finding the root of the problem
It is important to not only get treatment for the pain that you’re feeling, but to find out exactly what is pinching the sciatic nerve. That way, you will know what is causing your pain and what you can do about it. Without a proper evaluation and treatment plan, your sciatic nerve pain won’t simply improve.
Better to rest or to move?
If you focus on resting, it will probably help the inflammation and irritation of your sciatic nerve to go down. However, now you get weaker and when you start to get active again, the muscles in your leg won’t be able to cope with the load. Now, the contraction of your muscles and movement of your joints flare up the point of irritation and inflammation in your sciatic pain again. This leaves you in a cycle of pain, not knowing if it is better to rest or move. Trying to push through the pain to get back to exercising will simply cause you to injure the sciatic nerve, leading to damage if it is repeatedly injured.
You will need to address the bigger picture of what is causing your sciatic nerve pain and everything that is contributing to your pain. Your posture, the way you sit at work or in your car or the way you exercise are only a few things that you will need to look at and change to improve your pain. A very important aspect of your treatment should be to get the normal gliding movement of the sciatic nerve back to its normal state. Addressing the mechanical interface and muscles that can contribute to compressing the nerve should be a vital part of your treatment. Your buttock muscles and hamstring muscles should be able to contract under load (like when you are climbing up a step) and still allow smooth movement of your sciatic nerve. This can only be done through a proper rehabilitation and treatment program.
Patience is key with a sciatic nerve injury
Nerves take much longer to heal and you will have to work through your rehabilitation and through the phases of healing to give your body time to heal.
Problems we see when patients come to see us with sciatic nerve pain
Waiting too long and not getting a proper diagnosis
A common problem we see is that patients wait too long before they seek help. By the time patients come to see us, they have had sciatic nerve pain and back problems for months. If you don’t get a proper diagnosis from the start, it just wastes time. If anyone treating your pain is not also looking for the cause of your pinched sciatic nerve, they will keep on treating the incorrect thing. This will be ineffective. Now, the pain becomes unbearable, it holds you back from doing normal activities like driving and it will take so much longer to heal. The longer you wait, the bigger your chances of causing sciatic nerve damage.
No pain, no gain
People tend to try some home treatments like foam rolling or stretching exercises, without much success. Going at it with an approach of ‘no pain, no gain’ or ‘pushing through the pain’ is actually not a good idea when it comes to sciatic nerve pain. There is a big chance that you will simply flare up your pain, irritating your sciatic nerve even further.
Trying out, but not completing different forms of treatment
Often, patients try to get relief by taking anti-inflammatory medication or getting a c injection in the hopes of decreasing their pain. This, however, only slows the process of healing. You are not addressing the root of the problem by simply taking medication. And then, a lot of people tend to get impatient and they stop taking their medication. Or on the other hand, if they feel better they stop their treatment. Patience is key with a pinched sciatic nerve. It is important to complete your rehabilitation to the end.
Resting too much or too little
Too much rest leaves you weaker than before. Moving too much causes extra inflammation and irritation around the nerve. Finding the balance between resting and doing safe movements is key!
Let us help you with that, and stop your sciatic nerve pain in its tracks.
Physiotherapy treatment for sciatic nerve pain
We are confident that we can provide the best treatment for sciatic nerve pain. We understand that patients are often anxious to get back to their day to day activities and that is why we are here to provide guidance and answers. Physiotherapists can implement a very effective and structured plan of action that treats all the aspects of the problem and get you back on to where you want to be living your best life. Our physiotherapy treatment plays a vital role to restore the normal gliding movement of the nerve, to ensure your nerve and supporting muscles move as you move, without flare-ups.
The basic structure of our treatments:
- Determine what is causing your sciatic nerve injury
- How badly is your sciatic nerve injured?
- Protect your sciatic nerve from further injury
- Give the nerve time to heal
- Strengthen surrounding muscles
- Re-evaluate to monitor progress
Your treatment will aim to restore all the normal functions of your sciatic nerve. Allowing you to feel different sensations and stimulating muscle movement. The nerve should be able to move and glide without any obstructions to give you full flexibility and range of motion. Your physiotherapy treatment will involve working on muscle strength, range of motion, flexibility and stability. Treatment techniques will include: soft tissue massage, joint mobilisations, dry needling, strapping, laser therapy, nerve mobilisations and guiding you through a rehabilitation program of gradual strengthening, control and conditioning. It’s important that you commit to the treatment plan, as this improves your chances of successful long-term recovery.
Phases of rehabilitation
1st Phase: Protection & initial Healing
Protect
We have found that patients tend to push through their pain or even walking with a limp. A pinched sciatic nerve can cause such severe pain that it is painful to simply take a step with your sore leg. The nerve is stretched each time you take a step of put weight on your sore leg. Protect your sciatic nerve by resting and using crutches to keep the load off. The main concern is to prevent continuous inflammation and pain.
Avoid anti-inflammatory medication
Avoid using anti-inflammatory medication continuously, it delays healing by delaying inflammation. If you have severe sciatic nerve pain, you can use anti-inflammatory medication initially. Ideally, you want to use medication for pain only in the initial phases of your injury. That way, your pain will be under control and you will be able to get enough sleep and won’t have pain that constantly bothers you. Once the pain is under control, you can decrease the use of your medication and eventually stop taking it completely.
Compression
By using strapping or elastic bandage, inflammation and swelling can be relieved. It gives support, which also helps for your pain.
Information
Make sure that you get information from the person that is treating you. Its important to understand what you should and shouldn’t to do. You can make better decisions if you are informed. Your body knows best, so avoid too many types of treatments at once.
Loading
Let pain guide you to gradually return to your normal activities. Initially, it is tricky to know if it is better to rest or to move, but finding a balance between the two is the best you can do. Letting your back and your leg carry some of the load is a good way to keep muscles and joints moving, without overdoing it.
2nd Phase: Establish pain free range of movement
During your examination, it will become clear what you are able to do, and what you should avoid. We identify factors that contribute to cause your pain, specific to your case and will address these factors as your treatment progresses. When doing a movement, like bending forward to tie your shoelaces, you will be able to move to a certain point, before your pain starts. This is your pain-free range of movement. You are safe to move in this range and our exercises will be targeted between these boundaries of your pain.
The aim is that, with time, your pain-free range of movement improves and painful movements become less intense.
3d Phase: Tissue healing
We monitor the progress of the healing of your sciatic nerve injury and track the formation of scar tissue at the site of irritation. On a cellular level we’re able to accelerate tissue healing using dry needling, laser and ultrasound. As healing takes place, we want to see not only improvement of your pain, but also improvement in the sciatic nerve’s ability to conduct impulses. Your pins and needles and sensation should improve as well as your muscle strength. The normal glide of the sciatic nerve will be restored , without any areas of pinching, if optimal healing takes place.
4th Phase: Soft tissue and nerve stress
During each session we will re-evaluate to see if you are achieving the necessary targets for the sciatic nerve and muscles around it to be able to handle tensile, elastic and compression forces. The different muscles around the sciatic nerve must be able to take load without causing further irritation to the nerve. We start with small movements and minimal load and gradually get you used to more. We use isometric muscle contractions to start with. These are muscle contractions without movement to keep the surrounding muscles active without too much movement that could flare up the site of nerve irritation.
5th Phase: Full Range of Movement
The most important component of your rehabilitation is to regain full range of movement of the different joints and muscles that has been affected as well as a smooth range of movement of your sciatic nerve. Any scar tissue that forms on the inside at the site of the injury can cause future entrapment or pinching of your sciatic nerve. The mechanical interface and scar tissue must be lengthened and orientated to allow a smooth gliding movement of the nerve and smooth movement of all muscles and joints. We will help you to stretch more, move deeper and work into your pain. For this we use massage, stretches and joint and neurodynamic mobilisations to achieve full range of movement.
Bending forward to touch the ground should become easier during this phase.
6th Phase: Muscle Strength
During this phase of your rehabilitation, you will work on strengthening muscles in your back, hip and leg. Repeated contraction of muscles, improves their strength. But, it also improves your sciatic nerve’s ability to conduct impulses and stimulate muscles to contract. Stronger muscles have the capacity to work harder and can help to take the load off of painful joints and prevent compression on your sciatic nerve. We will progress your exercises more and more, adding resistance, doing more repetitions and building your overall strength.
You should be able to walk or get up from a chair without your back or your leg feeling weak and clumsy.
7th Phase: Muscle control and stability
It is one thing to feel your muscles get stronger, but another thing to feel like you have control when you move. The type of muscle contraction we use during this phase of rehabilitation is called eccentric muscle contractions. Muscles are able to contract and shorten concentrically, but they are also able to slowly lengthen eccentrically. Picking up something heavy or climbing down stairs are some of the things that require control and stability. You will also need to strengthen your core to give your spine and your lower back the stability it needs. With improved stability of your spine, you protect your spine and decrease compression on a pinched nerve.
8th Phase: Testing for return to activity
A big part of your recovery is to gradually return to your routine again. This way, we can determine if you are ready to return to fully working and training without any flare-ups of sciatic nerve pain. Your physiotherapist will guide you to re-engage in safe increments, and make adjustments where necessary.
9th Phase: Balance, High Speed, Power
With sciatic nerve compression, the normal amount of time that it takes for your sciatic nerve to conduct impulses, would have been reduced. Now, you’ve worked through different phases of your rehabilitation and at this stage we want to improve the accuracy and speed of your sciatic nerve’s impulses. You need to be able to do activities with precise balance, high load, and speed to ensure that the sciatic nerve and muscles in your leg will be able to keep up with the demands of your body.
Your physiotherapist will guide you to return to normal activities but will also challenge you past your normal boundaries to determine how your body reacts to different forces. Ultimately we prepare you to return to participating in your sport.
Whatever must be done – we’ll get you there. Sprinting, jumping, landing, golf swings and much more.
10th Phase: Sport Specific Training
This is the final stage of rehabilitation. Depending on your sport, your physiotherapist will tailor specific exercises to further improve your strength and endurance. A successful outcome is when you have gained knowledge throughout the rehabilitation program and can participate at full power and speed, not to mention the benefits of minimizing your chance of future injury.
How long will it take for my sciatic nerve injury to get better?
Nerves take a lot longer to heal, depending on the severity of your sciatic nerve injury. If there is nerve damage, it will take months to years to improve. Patience is key here.
Some days will feel better than others
Recovering from a sciatic nerve injury will have its ups and downs. You might feel better for a few days and then feel worse for a few days. Nerves are very sensitive structures so they tend to flare up easily, causing further inflammation and irritation. Just be prepared that your recovery process will be more of a cycle with ups and downs than a constant improvement from day 1.
Physiotherapy should start while your nerve is healing and if you have followed through with your physiotherapy treatment protocol, you should be able to recover completely and be able to return to your sport. Depending on the severity of your symptoms and initial inflammation, you will need physiotherapy treatment twice a week for the first two weeks. After this, your treatment sessions can be spread out to once a week or once in two weeks. You only spend an hour at a time with your physiotherapist. How fast you recover will greatly be up to you.
Other medical treatments for sciatic nerve pain
- Your doctor will probably prescribe anti-inflammatory medication or give you a cortisone injection or nerve block as treatment for a pinched sciatic nerve. Both of these medications will give temporary relief to the pain and inflammation that you are experiencing. However, it will not be the solution to your problem. And once the effect of the medication wears off and you try to get back into your normal routine, your pain could simply return.
- Getting your lower back or hip ‘aligned’ or ‘clicked’ in the hopes of improving the pinching of your sciatic nerve will not change your pain. An alignment cannot change the state of your nerve health or the inflammation taking place. It could even worsen a pinched sciatic nerve. You need to look at the bigger picture.
- A biokineticist will be able to help you in the final stages of your rehabilitation or to get you back to actively training for your sport.
Is surgery an option?
Surgery for sciatic nerve pain will only be an option if you have had persistent and severe pain and weakness of your leg that hasn’t improved with other non-surgical options of treatment. Even with persistent nerve compression, a neurologist will help to make the decision of when our focus of treatment should shift from preservation to protection of further nerve damage. Initially, we want to give your body a chance to heal on its own, but sometimes it is beyond the point of return. Surgical intervention is the next step after you’ve tried a non-surgical approach like physiotherapy treatment.
A few dangerous situations will lead to surgery being your first option:
- Cauda equina syndrome – a medical emergency where the lowest nerve roots (cauda equina) are compressed and you lose the ability to control your bladder or bowel movements.
- Tumors, cysts or abscesses
- Severe trauma such as severe fractures in the lumbar spine, or lacerations/stab wounds that causes complete nerve damage or a severed nerve.
Surgery is performed with the goal of eliminating the cause of your sciatic nerve injury and depending on the type of surgery done and on your surgeon’s orders, recovery from surgery can take you anywhere between 6 weeks or 6 months. Physiotherapy can still help you during the time of your post-operative recovery.
What else can it be?
- Piriformis syndrome: Pain in your buttock, sometimes spreading down your leg. Worse when you try to run, climb stairs or walk far. It can cause sciatic nerve pain and tingling/ pins and needles down your leg.
- Sciatica: Pain, pins and needles and numbness spreading down your leg. Caused by compression or irritation of a lumbosacral nerve root.
- Disc bulge/herniated disc: Pain in your lower back, with the possibility of pain referring down your leg as well. It is especially painful when you bend forward or when you sit or drive.
- Spondylolisthesis: One vertebra slides forward on top of the vertebra below it. This causes your spine to become unstable, therefore leading to pain when you bend forward and especially when you try to come back up. You will feel the need to push yourself up with your hands.
- Lower back OA: Pain caused by degeneration in the joints in your spine. The pain feels worse when you overdo it with walking far or standing for a long time. It also feels worse in cold weather and in the mornings. However, it improves when you rest.