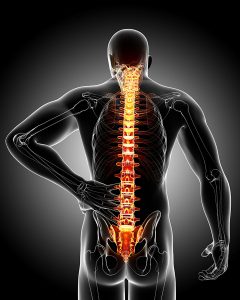
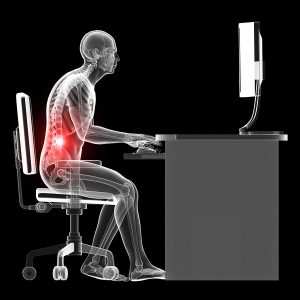
The extremely uncomfortable feeling of a muscle ‘pulling’ or ‘spasming’ in your back leaves you in severe pain. You feel like you can’t straighten up properly or like your back is ‘skew’, pulled in one direction. Simple things like bending to pick up your bags or turning to talk to someone next to you leaves you in such pain that you feel weak from it. Suddenly you feel much older, because you can’t move the way you would like to. This is what a back muscle spasm feels like. And, even though everyone gets a muscle spasm in their back at some point in their life, most people fail to recognize that there might be a bigger problem lurking underneath. This should change the way you think about a back muscle spasm and change the type of treatment you expect to get.
Usually, you wait for the muscle spasm to subside by itself and try to treat it with a massage or by taking a muscle relaxant. But what if it doesn’t go away? What if it doesn’t ease? Or even worse it comes back again. Did you know that muscle spasms form in an attempt to keep your spine stable and to protect other vulnerable structures like joints, nerves and discs. Now it should be clear why it is so important to get the right treatment from the start and to find out exactly what is causing your back muscle spasms.
Anatomy of the muscles in your back
Let’s first look at the underlying structure of your back so that you can understand where and how muscles fit in.
The basic structure
Your spine is the stable foundation of your back, giving you an upright form. It consists of bones (vertebrae) stacked on each other. There are 24 vertebrae altogether and can be divided into three parts namely: your neck (cervical spine), your middle back (thoracic spine) and your lower back (lumbar spine). Between each vertebra, there is a disc, made up out of a gel-like material. These discs act as shock absorbers and they improve the mobility of your spine, without sacrificing the supportive strength of your vertebral column. Ligaments connect the different vertebrae together and provide extra stability. Between each vertebra, a nerve root exits on each side, branching out to connect to other nerves.
Muscles allow the spine to move
The human body has over 600 muscles and that is around 40% of your bodyweight. All muscles are made of an elastic kind of tissue. Each muscle consists of thousands and thousands of small muscle fibers. A muscle’s strength depends mainly on how many fibers are present. With more movement and more muscle contractions, muscles grow bigger (hypertrophy), but with less movement they become smaller and weaker (atrophy).
Back muscles
The muscles in your back, along you spine, work together as a group, giving stability to your spine, but also allowing your upper body to move, bend and twist. Even though your spine can be divided into three parts (your neck, middle back and lower back), the muscles in each part do the same basic movements. They can be divided into four groups: extensors, flexors, lateral flexors and rotators.
- Extensor muscles are the back layer. They make it possible for you to straighten up and lift objects.
- Flexor muscles are the front layer. They make it possible for you to bend forward.
- Lateral flexor and rotator muscle are the side layers. They help to rotate your spine and bend sideways.
What is the function of the muscles in my back?
Muscles along your spine allow you to move, bend and twist your upper body and neck. Even though the muscles are divided into different groups responsible for different actions, they never work in isolation.
When you move, you don’t think about each muscle you should contract or control. No, you simply move when you want to move. You can change from one position to the next and your body tries to accommodate you in whatever you want to do. With each movement, there are groups of different muscles that coordinate with each other. For example: when you bend forward, your flexors would be the main muscle group responsible for that. They contract and shorten, pulling you forward. However, your extensors need to lengthen, to control this movement and to prevent you from bending too far forward or even falling over.
Flexors:
Flexor muscles moves your spine forward, allowing you to bend forward. Bending over to pick up your grocery bags or bending down to brush your teeth are some of the basic things that these muscles help you with.
Extensors:
Extensor muscles pulls your spine backwards, allowing you to straighten your back, look up and bend over backwards.
Rotators and lateral flexors
These muscles allow you to turn and bend sideways. Even something as simple as looking over your shoulder in the car involves not just only turning your neck, but also turning your whole body.
Stability
Another very important job for your back muscles is to give your spine stability. Muscles, together with ligaments, prevent your vertebrae from moving or shifting out of place. Ligaments provide static stability because they can’t move or contract. Muscles provide dynamic stability. That means that even while they move your spine, they still keep it as stable as possible.
You might think that sitting or standing in one position doesn’t require a lot of work from your muscles. But, just because you’re not moving, doesn’t mean that muscles are not working hard to keep your spine upright. The same way that muscles can be divided into different groups responsible for different movements, they can also be divided into ‘moving muscles’ or ‘stabilising muscles’.
‘Moving muscles’ (mobilisers) are big strong muscles responsible mostly for moving you. ‘Stabilising muscles’ (stabilisers) are located in the deep layers, close to the spine. They contract constantly throughout the day keeping your back upright, making sure that each segment (each vertebra) stays in place. Overall, if each segment is stable, your whole spine is stable. In the end, instability is what leads to injury.
So, even while you are sitting, thinking that your back is ‘rested’, your stabilisers continue to do very important work.
I have a back muscle spasm. How did it happen?
A muscle spasm can be defined as a “persistent, involuntary muscle contraction”. The main reason why this involuntary muscle contraction causes pain, is because it causes a decrease in circulation to the area. This pain is a message and a warning.
Usually, it starts with some warning signs
Stiffness, discomfort, and a feeling of “something is not right in my back”. This is your warning sign of a muscle spasm forming. Your body is trying to bring to your attention that something is wrong. Usually, people ignore these initial warning signs and push through the discomfort.
The next step your body takes is to form of a full-blown muscle spasm in your back. By doing this, your body is limiting your movements to protect itself. To protect deeper structures like joints, ligaments, and nerves from further injury.
Your lifestyle contributes too
In today’s world we sit more than anything else. Work has become something where you sit, looking at the work on your desk or computer screen on a daily basis. You don’t get enough sleep, your stress levels increase, and physical exercise and your overall sense of well-being takes the backseat.
Your back helps to carry a lot of your body’s weight. If you are overweight or don’t have the necessary back muscle strength, your back takes a lot of strain on a daily basis. Ultimately, this causes instability of your spine. Instability causes increased pressure on the intervertebral discs, joints and nerves, leading to injuries like a bulging disc or nerve compression. It also causes muscle spasms in an attempt to protect your spine. That is why it is so important to create a lifestyle that encourages you to have good muscle strength. Strong back muscles can support your back better and help to hold you upright.
Take a step back and look at the bigger picture
Imagine your back is a tower of Jenga blocks stacked on top of each other, without any of the pieces missing.
Stage 1 – Healthy and strong
You have a healthy spine and a healthy lifestyle that allows you proper sleep, enough exercise, good health and manageable stress. This is a system that works in perfect harmony and one that can react to any load that you put on it. The tower of Jenga blocks is stable and solid.
Stage 2 – Falling apart
Now, one by one, the Jenga blocks are removed. If you don’t get enough sleep, remove a block. Working long hours in a terrible posture? Remove a block. Weak back muscles? Remove a block. With each block that is removed, the chances of the tower collapsing becomes more likely. When a sufficient number of blocks are removed, the tower becomes so unstable that it is still standing, but the slightest movement can topple the whole structure.
Stage 3 – The last block
The last block is removed and now you end up with a muscle spasm in your back. Without the other supporting blocks, the tower is so unstable that it is about to topple over. The muscles in your back attempt to desperately save your vertebrae from shifting or your spine from collapsing, the same way the tower is about to collapse.
Stage 2 is where most of us are and we rarely ever return to Stage 1.
You thought you fixed it
We try to find ways to return to Stage 1, by trying to fool our system. We desperately try to build the tower of Jenga blocks back up and make it work by taking medication, going for massages or doing some stretches. This way, you feel a bit better and fool your body to believe that “it’s all back to normal”. But in fact, you have not built the tower of Jenga blocks back up to its original state of stability, you only do damage control. The tower is standing, but on the edge of collapsing again when a piece is removed in future.
To really prevent back muscle spasms, you need to start building the blocks from the bottom up and not just reposition the last one. Part of the reason that we don’t do this is because we feel better halfway through. The first sign of such relief gives us reason to believe that we have ‘fixed’ our back muscle spasm. But the fact is, it will just be a matter of time before it all comes back again.
Pushed to the limit
When a muscle in your back is forced to contract under a lot of pressure or remain contracted for a long time, a back muscle strain occurs. It becomes too much, the muscle can no longer hold the contraction and this combination of muscle fatigue and overload lead to a muscle injury (strain). It is pushed beyond its limits, beyond a point of simply spasming. Now, you end up with a torn muscle and inflammation that causes swelling and further irritation. The other muscles surrounding the injured muscle will spasm protectively to prevent even further injury. Now, you are left in even worse pain and you won’t be able to do the easiest things like bending down to brush your teeth.
What is causing the muscle spasms in my back?
Muscle spasms caused in response to instability and underlying injuries
Instability of your spine leads to increased pressure on structures like your discs, joints and nerves. This leads to injuries like a herniated disc, osteoarthritis or nerve compression. On top of this, protective muscle spasms form to prevent you from injuring yourself even further. The muscle spasms are likely to keep recurring if the instability and inflammation is ongoing.
Back muscle spasms due to a muscle strain
A muscle strain is a muscle injury where the muscle gets overstretched or torn. The injured muscle and surrounding muscles will spasm in an attempt to protect you from worsening the injury. Pain and stiffness will make it impossible for you to move. This protects you from bending too far and overstretching or completely tearing the injured muscle.
Bending to pick up a heavy object
Bending forward puts the muscles in your back in a stretched position. To get back up, requires these muscles to pull your whole upper body back up. Now, imagine how much harder they need to contract when you bend forward to pick up a heavy box from the ground. If the effort is too much, you end up with a muscle strain and protective muscle spasms in your lower back, due to overexertion.
Holding or carrying a heavy object for a period of time
Carrying a very heavy hiking backpack or carrying new furniture around the house puts a heavy load on your back. Your muscles grow tired from contracting under extra pressure, causing a muscle spasm in your lower back.
Repetitive bending or twisting movements
While picking up the children’s toys, you repeatedly bend and twist your body in an awkward way to reach the toys and you get back up to put them back in their place. A repetitive movement like this means the muscles in your back has to contract and relax again and again. Your muscles get tired and while you want to push through to finish the task, you could strain a back muscle or end up with a severe muscle spasm.
Slipping or falling
You slip on a wet floor and in the wink of an eye you’ve fallen over, hurting your back. While you are falling, your body responds and tries to protect you. The suddenness of the fall, leads to a protective reaction where you tense the muscles in your back. Usually, it’s not the direct impact that hurts you the most. It is the quick, intense contraction of the muscles trying to stabilise you, that leads to a muscle spasm.
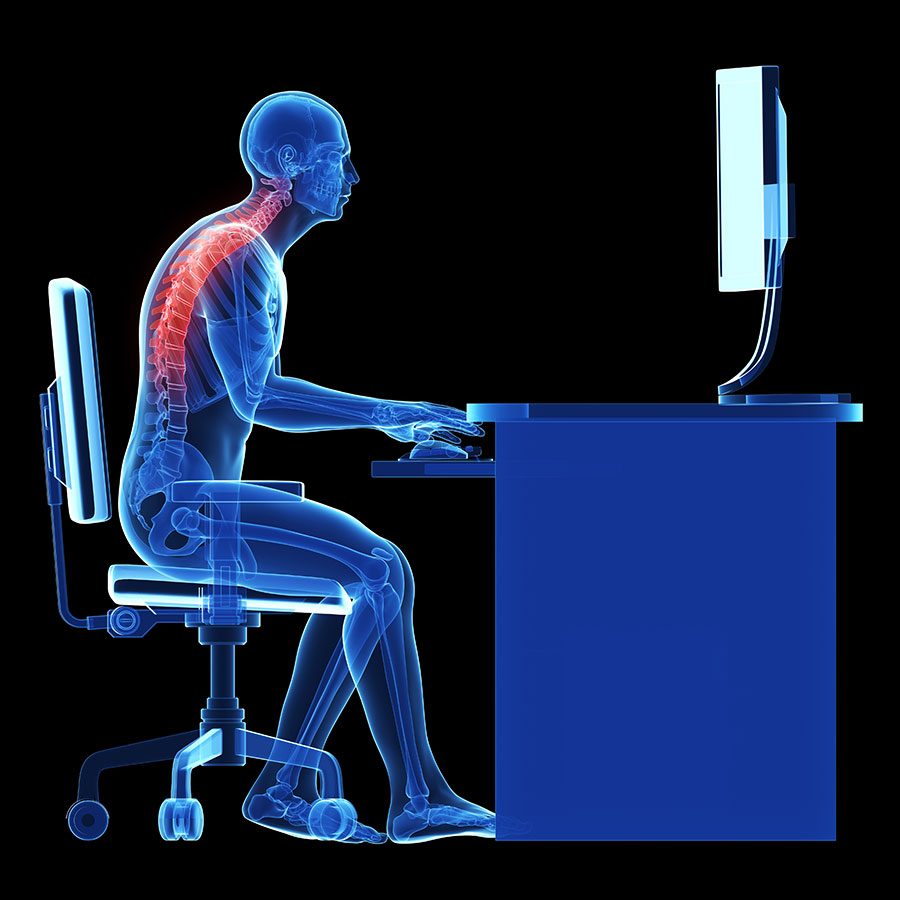
Sitting for many hours on end
Clearly, we were never made to sit in front of a desk or computer for such a long time without breaks or interruptions. Although you feel ‘rested’ while you’re sitting, your spine is not actually relaxed. The muscles that stabilise your spine will have to contract and work the whole time you are seated to keep you upright. They get tired and fail to support your back. The pressure and the weight of your upper body squash the discs and joints together, not just for a few minutes, but for hours on end. Your body detects the tissue damage and causes muscle spasms in response.
Overloading the wrong muscles
Different muscles have different jobs to do. You have big and strong MOVING muscles, allowing you to bend in any direction. Then you have STABILISING muscles, that can be found in the deeper layers of muscles around the joints of your spine, whose job is stabilisation. If you sit or stand for a long time and have to keep your back straight, your STABILISING muscles will grow tired and fail to do their job. Now, automatically your body recruits the bigger MOVING muscles to help. If this continues to happen, with time, the MOVING muscles get used to STABILISE and MOVE. They now have a dual role of stabilising the spine AND moving it. They can’t maintain contractions like this and will fatigue, leading to muscle spasms in your back.
Muscles spasms in your lower back will recur time and time again if you don’t get the right treatment for the real underlying cause.
Symptoms of a back muscle spasm
How bad is my back muscle spasm?
There is no specific grading for the severity of a muscle spasm. A good way to determine the severity of the muscle spasm in your lower back, is to look at how much it is influencing your life. Are you able to bend, sit, get up to stand, walk, run or exercise? Severe muscle spasms in your back is so disabling that simply turning to talk to someone sitting next to you will be excruciating.
It starts with a muscle spasm, but could get worse
If the load placed on your back muscles is too excessive, the muscles won’t be able to hold the contraction. Standing stooped over a box while you sort through some things will cause your back to get tired. Your back muscles are now forced to contract while being overstretched. This makes them vulnerable to injury. This combination of muscle fatigue and overload may lead to a muscle spasm at first. This spasm is to warn you to not push any further. Pushing through it leads to a muscle strain.
What is the difference between a muscle spasm and a muscle strain?
A muscle strain is an injury that leads to tears in the muscle tissue and a muscle spasm is a continued, involuntary contraction of a muscle. Muscle spasms usually serves as a warning for you to stop doing what you’re doing because it could lead to a muscle strain. Back muscle spasms can ease with the right treatment, whereas a muscle strain is a tear in the muscle that needs to heal with time.
Grading of a muscle strain:
• Grade 1: A small amount of micro tears occur within the muscle. It usually presents as stiffness rather than pain.
• Grade 2: A large number of micro tears occur, causing a partial tear of the whole muscle. It is painful to move or stretch the muscle.
• Grade 3: The muscle tears along a large area or tears completely. This is the most severe muscle strain that you can get. This degree of muscle strain will cause intense sharp pain and even the slightest movement or stretch will cause severe pain.
Recurring, chronic muscle spasms is a secondary problem caused by an underlying injury. Instability and repeated pressure and compression of the joints, discs and nerves in your back, will cause protective muscle spasms. This is known as muscle guarding. If you ignore the warning signs and push through the pain of your muscle spasms, you could be injuring yourself even further. With time and with recurring back muscle spasms, you become afraid of doing certain movements. You never know when your back will seize up. Now, you think twice before you say yes to jump on the trampoline with your kids. It could happen any moment and you know by now, how bad it is. You want to avoid it at all costs.
Repeated spasms or muscle strains can cause permanent damage to the structure of your back muscles. Listen to the warning signs that your back is giving you and get the right treatment for the spasm in your back from the start!
Diagnosis of a back muscle spasm
Physiotherapy diagnosis
Our physiotherapists are experts in human anatomy and movement with the necessary experience to diagnose a muscle spasm or muscle strain. We fully understand the intricate way muscles work in coordination with each other and can accurately diagnose which muscle has been injured and if any other structures in your back has been injured as well. Doing a full clinical assessment and getting the necessary information about your pain is the starting point.
During your physiotherapy evaluation, we will stretch and stress the muscles along your spine to determine which one has been injured. We can accurately identify where your spasm is coming from. We will also test other structures like joints, discs and nerves. Thorough evaluation makes our physiotherapists the best at diagnosing this type of problem.
X-rays
Muscles cannot be seen on an x-ray, so it will not be effective to diagnose a muscle spasm. X-rays will however show the integrity and alignment of joints in your spine. This will enable us to see if something is wrong with the structure of the bones in your spine or if there is a loss of disc space.
Your physiotherapist will refer you to get x-rays taken if deemed necessary.
Diagnostic ultrasound
Our Diagnostic ultrasound can be used to show the presence of a muscle tear (muscle strains), inflammation, swelling or simply increased contraction of a muscle (muscle spasms).
If you need an ultrasound, your physiotherapist will refer you.
MRI
An MRI will show all of the structures in and around your spine. This includes vertebrae and soft tissue like muscles, discs and nerves. It will show a muscle tear and areas of bruising or bleeding within the muscle. However, an MRI is an expensive test and you need to be referred by a specialist to get one. So, it won’t be necessary for you to go for an MRI from the start.
If your physiotherapist suspects anything bigger than a muscle spasm and feels it is necessary for you to get an MRI, you will be referred to a specialist.
Why is the pain from my back muscle spasm not going away?
A back muscle spasm might start out as a protective mechanism. It protects you from injuring yourself any further. However, if you do nothing about it and the muscle spasm continues to bother you, it will prevent you from getting your full movement back. If you don’t move fully and with ease, your muscles become weaker, joints become stiff and your spine less stable. You become stuck in a cycle of pain, not knowing if it is safe to move or not.
Make sure you are getting the right treatment for your back spasm from the start
The sooner you sort out exactly what is causing the muscle spasms in your back, the better. Certain treatments like medication might ease the pain from the spasm in your back, but it won’t prevent the pain from coming back if there is something deeper causing it. If it was a muscle strain and not just a muscle spasm, it will take longer for the tear to heal.
You might feel frustrated that your back spasm isn’t easing, but there could be something else that needs your attention. There is a risk of more critical and possibly irreversible damage to your back if you don’t take the warning signs seriously.
Problems we encounter when people come to us with back muscle spasms
Waiting too long and not getting a proper diagnosis
A common problem we see is that patients wait too long before they seek help. By the time patients come to us for treatment of their back spasms, they have had problems with recurring back muscle spasms for months or even years. The problem with this attitude is that by the time you come to see us, the problem is a lot more advanced and it will take a lot longer to get better.
If you don’t get a proper diagnosis from the start, it wastes time. If anyone treating your back spasms is not looking for the cause, they will keep on treating the incorrect thing. This is ineffective and the muscle spasms will simply return. Over time, you learn that you never know when a severe muscle spasm is going to hit you and that is scary. You start to think twice about doing the things you love like gardening or playing with your kids, because you anticipate that you’ll have pain. The longer you wait, the bigger your chances of causing permanent damage.
Trying out, but not completing different forms of treatment
Often, patients try to get relief by taking medication or getting a voltaren injection in the hopes that it will ease their pain. They also try massages, foam-rolling, cupping or stretching. However, these treatments only mask the pain and stiffness that comes with a back spasm. You are not addressing the root of the problem by trying any of these treatments in isolation.
And then, a lot of people tend to feel that their back spasm is easing halfway through their treatment programme, so they stop. You need to address the root of the problem and get your back muscles conditioned to handle more load. That is the best long-term solution. Patience is key with recurring back muscle spasms.
Resting too much or too little
Resting too much leaves you weaker than before. Moving too much causes extra spasms, inflammation or even injury to the muscle. Finding the balance between resting and doing safe movements is key!
Let us help you get the right treatment for your back spasms stop it from bothering you again in the future.
Physiotherapy treatment
We are confident that we can provide the best treatment for back muscle spasms. We understand that you would want to pick something up without any fear of ‘spasming up’ or do a deadlift in the gym with confidence. That is why we are here to provide guidance and answers. Physiotherapists can implement a very effective and structured plan of action that treats all the aspects of the problem and gets you back to where you want to be living your best life. Our physiotherapy treatment will help you to improve your muscle strength so that you are able to regain control and stability of your spine and restore normal movement.
The basic structure of our treatments:
- Determine which muscle has been injured
- How bad is it injured?
- Protect it from further injury
- Give it time to heal
- Strengthen
- Re-evaluate to monitor progress
We will be looking at different aspects, like testing back and neck’s ability to bend and turn in different directions. And we will also look at muscle strength, range of motion, flexibility and stability. Treatment for back muscle spasms will include: soft tissue massage, joint mobilisations, dry needling, strapping, laser therapy, nerve mobilisations and guiding you through a rehabilitation program of gradual strengthening, control and conditioning. It’s important that you commit to the treatment plan, as this improves your chances of successful long-term recovery.
Phases of rehabilitation
1st Phase: Protection & initial Healing
Protect
We have found that patients tend to push through their pain and even continue to exercise with a back muscle spasm. This can cause continuous inflammation and pain. Protect the injured muscle by resting and avoiding painful movements.
Avoid anti-inflammatory medication
Avoid using anti-inflammatory medication especially in the first two days after your muscle injury. It delays healing by delaying inflammation. Ideally, use only pain medication without an anti-inflammatory component for pain in the initial phases of your injury. That way, your pain will be under control and you will be able to get enough sleep without pain that constantly bothers you. Once the pain is under control, you can decrease the use of your medication and eventually stop taking it completely.
Compression and heat
Strapping can provide good support for the painful area in your back, which in turn will decrease your pain. Heat also has a pain-relieving effect, so you can apply a beanbag or hot water bottle to the area of your pain.
Information
Make sure that you get information from the person that is treating you. Its important to understand what you should and shouldn’t do. If you are informed, you can also make the right decisions. Your body knows best, so avoid too many types of treatments at once.
Load
Let pain guide you to gradually return to your day to day activities. Initially, it is tricky to know if it is better to rest or to move, but finding a balance between the two is the best you can do. Safely moving your back, allows the joints and muscles to move, without you overdoing it.
2nd Phase: Establish pain free range of movement
During your examination, it will become clear what you are able to do, and what you should avoid. We identify factors that contribute to cause your back muscle spasms and will address these factors as your treatment progresses. When doing a movement, like bending forward, you will be able to move to a certain point, before your pain starts. This is your pain-free range of movement. You are safe to move in this range and our exercises will be targeted between these boundaries of your pain.
The aim is that, with time, your pain-free range of movement improves and you’re able to bend and also pick up your grocery bags with ease.
3d Phase: Tissue healing
During this phase of treatment for your back muscle spasm, we monitor the progress of healing of your injured muscle and track the formation of scar tissue and adhesions. On a cellular level we’re able to accelerate tissue healing using dry needling, laser and ultrasound. As healing takes place, we want to see not only improvement of your pain, but also improvement in the muscle’s ability to endure a contraction. If optimal healing takes place, then the muscle can contract and relax smoothly without any pain.
4th Phase: Regain stability
During each session we will re-evaluate you to see if your injured muscle can handle doing different movements, but also help to stabilise your spine. An important starting point in treatment for your back muscle spasm, is to help you find a position where you feel your spine is in a neutral position. Often, just getting used to keep your spine in a stable and neutral position is hard work because you got used to wrong movement patterns. From here on, you will have to be able to hold the stable position of your spine while we slowly get you to do different exercises. This way, you build your muscle strength back up with the ability to keep your spine stable. The best foundation you can have.
5th Phase: Full Range of Movement
The most important component of your rehabilitation is to regain full range of movement of the your spine and the muscles around it. The muscle fibres of the affected muscles must be lengthened and orientated to allow a smooth contraction. Once the muscle’s length and ability to contract has been restored, it will be able to help with stabilising your spine again. You should be able to not only bend in all directions, but have better movement of your spine as well. During this phase we will use: massage, stretches, myofascial release and joint and neurodynamic mobilisations.
You should be able to bend and turn in all directions at the completion of this phase of treatment for your back muscle spasm.
6th Phase: Muscle Strength
It’s common to feel some pain when you start to work on muscle strength. This is could be due to abnormal muscle tissue adhesions which prevents the muscle from contracting smoothly. But it could also be due to poor endurance and muscle strength. Usually, you feel pain when your muscles start to fatigue. That’s why it is so important for you to strengthen the muscles around your spine. Ultimately, it improves your pain and gives your spine the necessary stability in a neutral position so that you have a stable foundation. Your posture will improve and doing your day to day activities will become easier. During this phase of rehabilitation we will progress your exercises more and more, adding resistance, doing more repetitions and building your overall strength. You should pick up something heavy with more confidence after completing this phase.
7th Phase: Muscle control and stability
It is one thing to feel your muscles get stronger, but another thing to do movements slowly and controlled. The type of muscle contraction we use during this phase of rehabilitation is called eccentric muscle contractions. Muscles are able to contract and shorten concentrically, but they are also able to slowly lengthen eccentrically. In this phase of treatment for your back muscle spasm, you must be able to keep your spine stable whilst moving it, needing control and stability. You should also be able to control your spine while you move other body parts like your legs or arms. With improved muscle control, you improve the stability of your spine, thus protecting it and decreasing the chances of recurring back muscle spasms.
8th Phase: Testing for return to activity
Gradually returning to your routine and getting used to the intensity of your usual activities is a big part of your recovery. This way, we can determine if you are ready to return to fully working and training without any flare-ups of back muscle spasms. The improved stability of your spine is like a stable base or foundation that you can move from. Even with repetitive movements throughout your day (like sitting and getting up) or more load (like picking up your child), your back muscles should be able to handle it while keeping your spine stable. In this phase of treatment for your back muscle spasm, your physiotherapist will guide you to re-engage in safe increments, and make adjustments where necessary.
9th Phase: Power and speed
You need to be able to do certain activities like sprinting or deadlifts with high load and speed. The muscles in your back must keep up with the demands of your body, without causing recurring muscle spasms. During this phase your physiotherapist will guide you to challenge your muscles past your normal boundaries to determine how your body reacts to different forces. Ultimately we prepare you to return to participating in your sport.
Whatever must be done – we’ll get you there. Weightlifting, sprinting, jumping, golf swings and much more.
10th Phase: Sport Specific Training
This is the final stage of rehabilitation. Your physiotherapist will still continue with myofascial release, trigger point release and electrotherapy modalities where needed, but sport rehabilitation is most important during this phase.
Depending on your sport, your physiotherapist will tailor specific exercises that will help strengthen the muscles pertaining to your sport. A successful outcome is when you can participate at full power and speed, not to mention the benefits of minimizing your chance of recurring back muscle spasms.
How long will it take me to recover?
The time it will take to heal will depend on the severity of your symptoms, initial inflammation and true underlying cause of your back muscle spasm. It might be ‘fixed’ in simply a few physiotherapy treatment sessions, but if we look at the root of the problem and address a longstanding problem of compensation and muscle weakness, it must be cleared up step by step. This is the part that takes much longer, but the rewards and long-term relief will last so much longer.
Initially, you will need physiotherapy treatment twice a week for the first two weeks. After this, your treatment sessions can be spread out to once a week or once in two weeks. You only spend an hour at a time with your physiotherapist. How fast you recover will greatly be up to you. If you complete your physiotherapy treatment protocol, you should be able to recover completely and return to your sport.
Other forms of treatment for muscle spasms in your back
- Your doctor will probably prescribe anti-inflammatory medication or give you a voltaren injection to get the muscle spasm to ease. Both of these medications will give temporary relief to the pain and stiffness that you are experiencing. However, it will not be the solution to your problem. Once the effect of the medication wears off and you try to get back to working or exercising, your pain could simply return.
- Getting your back or neck ‘aligned’ or ‘clicked’ in the hopes of improving the muscle spasm will not improve the state of the muscle or change your pain. It could even worsen or trigger a muscle spasm. You need to look at the bigger picture.
- A biokineticist will be able to help you in the final stages of your rehabilitation or to get you back to actively training for your sport.
- Wearing a back or neck brace in the hopes of giving it extra stability might ease the spasm and make you feel better while you’re wearing it, but it won’t be the solution to your muscular problem. In fact, muscles become weaker when you wear a brace and you become dependent on it. It will only worsen your problem.
- Stretching or foam-rolling your back might ease your muscle pain temporarily, but if the real problem isn’t addressed, your muscle spasm will simply return.
Is surgery an option?
Surgery is not an option for back muscle spasms. Recurring muscle spasms in your back is due to the loss of stability. An orthopaedic surgeon will use instrumentation to ‘fixate’ your spine and this will grossly reduce movement of your spine and movement between each vertebra (segment). It might be a solution for you, but you run the risk of future surgeries because the levels above and below the fixation will wear out and degenerate faster. That means that future surgeries will be inevitable.
If your physiotherapist finds the underlying cause of your pain and spasms as worrying, you will be referred to the right specialist.
What else could it be?
- Disc bulge/herniated disc: Pressure on the spine increases pressure on the discs. This could lead to a disc bulging out to the side, irritating the structures around it. Pain when you bend forward, sit for long periods, drive or look down at your computer.
- Spondylolisthesis: One vertebra slides forward on top of the vertebra below it. This causes your spine to become unstable leading to pain when you bend forward and especially when you try to come back up. You will feel the need to push yourself up with your hands.
- Osteoarthritis of your spine: Pain caused by degeneration in the joints in your spine. The pain feels worse when you overdo it (e.g walking far or standing for a long time). It also feels worse in cold weather and in the mornings. Improves when you rest.
- Nerve pain: Burning, electrifying pain with pins and needles and/or numbness. This is due to nerve compression or irritation.