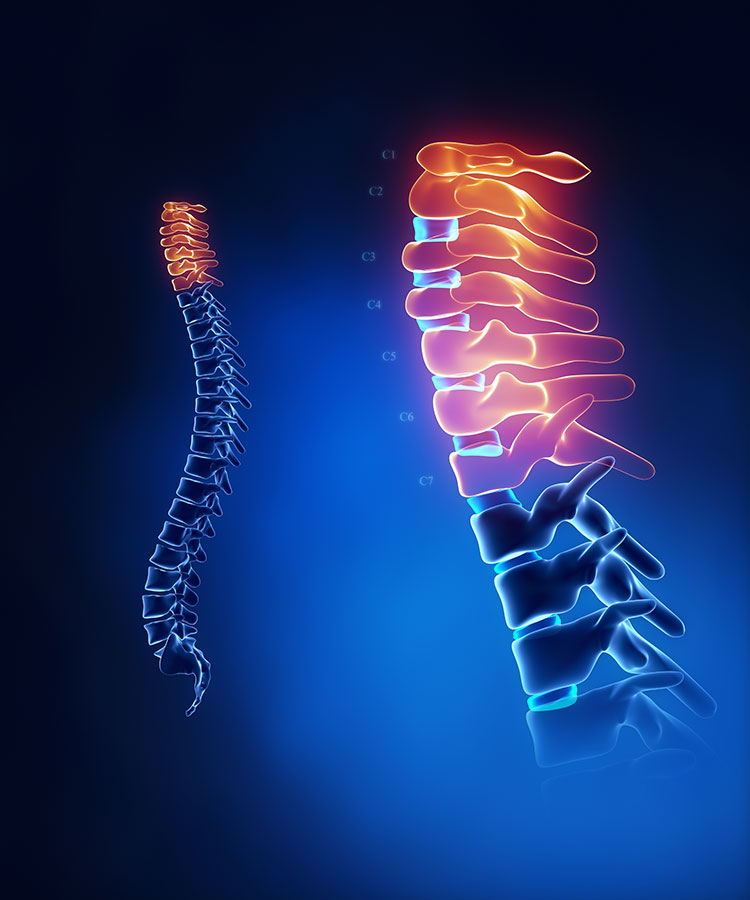
Cervical spondylosis refers to the normal degenerative changes in your neck caused by aging and posture. This is the “wear and tear” that your doctor might have described when discussing your X-ray with you. These changes aren’t abnormal or dangerous, think of it as a normal part of life like graying hair or wrinkles. It is not always cause for panic and alarm, even if pain progressively creeps in.
Spondylosis of your neck doesn’t mean you will always have pain. Many people would notice a stiff neck that may be painful at times or with certain movements. The spondylosis doesn’t change from day to day, but the levels of pain and stiffness varies. This is what we will focus on when you come to see us because of a stiff, sore neck – we cannot reverse the degenerative changes in your neck, but we can definitely improve your quality of life.
How does it happen?
Degeneration of the neck joints start because of normal forces acting on the joint complex. The joint complex refers to the entire team who has to carry the load and allow pain free movement. This team includes two cervical vertebrae, the disc in between, the ligaments that aid in stability and the muscles that attach or pass over the joint to generate movement. All these components directly affect the neck joint’s movement, lets look at each individual component.
Discs
With age, discs lose their hydration the same way skin loses it’s elasticity. This will lessen the disc’s ability to absorb forces placed on the neck. The disc narrows from top to bottom because of the increase in forces. Loss of disc height is the reason elderly people seem to get shorter as they age. The increase in load may lead to disc bulge/prolapse which results in the surrounding structures being pinched & compressed.
Ligaments
The ligaments lose their elasticity which causes traction spurs to develop on the bone. Osteophytes are bone spurs that form as the body’s attempt to help stabilize the joints. Osteophytes can form in the way of a nerve root or may even become dislodged. The facet joints – where the top vertebra fits onto the bottom one – undergo changes where they become bigger in an attempt to stabilize the motion segment of the neck joint. This contributes to limited movements and the feeling of a “stiff neck“.
Nerve
All of these changes occupy space in an already tight fit area, even under normal circumstances. This can lead to stenosis, a narrowing of the canal through which the spinal cord passes. This narrowing between the bones will lead to compression of the nerves running to the shoulders and upper arm. This causes symptoms similar to that of a disc bulge/prolapse, but can be traced back to its origin from the neck joints.
Muscles
The surrounding muscles need to work overtime to move against the in-congruent joint surfaces. Stability muscles get weaker, leaving you with the headache of a constantly stiff and sore neck.
Causes of cervical spondylosis
Cervical spondylosis is basically degeneration of the structures in your neck: the intervertebral discs, facet joints and ligaments connecting these different structures to each other. This is a natural process that happens over time like your car tires that become worn.
Spondylosis diagnosis peaks between the ages of 50-59, with approximately 3 in every 1000 people diagnosed with cervical spondylosis. About 95% of people over the age of 65 have some degree of spondylosis. Men and women are equally affected, but men tend to be diagnosed at a younger age. In South Africa rugby injuries are most likely to be blamed. The neck joint levels of C5/6/7 are the most commonly affected due to their position and the curve of the neck.
Your risk of developing neck joint degeneration will be higher after injury or trauma – like a car accident, fall, rugby injury, disc prolapse/bulge – or excessive strain due to posture, work or sport – like dentists, computer work, cycling etc.
Symptoms of cervical spondylosis
How bad is it?
You may experience recurrent attacks of pain that come and go, which may differ in intensity and duration. It does not develop overnight, but rather progressively gets worse, starting off as occasional stiff and sore neck. Over time it happens more frequently, lasts for longer periods of time and eventually your pain is constant.
The pain will be dull and deep on both sides of the neck and as it gets worse you may experience numbness and weakness of the arms and hands. This referred pain could be due to nerve compression or muscular referral. Pain will be worse with sudden movements, movement into end range or sustained positions e.g. sitting in front of a computer for hours, driving or texting.
Pain will get worse with too much activity and relieved by rest, but keeping your neck completely still will also cause more pain. Symptoms are worse in the mornings with stiffness in all directions, which takes about 30 minutes to ease. The longer it takes to ‘settle’ or ‘get moving’ the more progressed the degenerative spondylosis of your neck has become. Your neck may make sounds with movement or feel dry and in need of some ‘oiling‘ to just get moving again.
As the condition gets worse over time you will find that you lose movement when turning your head, like looking in your blind spot when driving. Looking up will also be stiff and painful and as the cervical spondylosis progresses you will notice that you cannot lift your head very far to look up.
Stage 1: Non-specific neck pain
In the first stage of cervical spondylosis you will only have neck pain from time to time and the pain will only be in your neck.
Stage 2: Cervical radiculopathy
In the second stage of cervical spondylosis you will start getting symptoms in your arms – this could be pins & needles, weakness or numbness. These symptoms are called radiculopathy and it’s caused by an irritated or pinched nerve in your neck which is due to the degenerative spondylosis.
Stage 3: Cervical myelopathy
In this stage you will have constant symptoms due to pressure on the spinal cord. This could be numbness, grip weakness in your hands, clumsiness when walking or bladder and bowel problems.
Diagnosis
The diagnosis of cervical spondylosis is made by taking a thorough history of the condition and testing the movements of your neck. X-rays are useful to confirm the diagnosis, but aren’t necessary, because what we see on an X-ray doesn’t change the treatment. Your physiotherapist will treat what we find during our assessment, not what we see on an X-ray.
Movement tests
Our assessment will always start with an interview to find out when your symptoms started, what could be contributing to your pain and if there are any other medical conditions we should be aware of. We will test the range of movement of your neck to find out which movements are limited and also to determine what makes your pain worse. During these tests we will ask you where the pain is when you do the movement, because this will tell us if it’s caused by a neck joint problem or muscle stiffness problem.
Contributing factors
There are different causes for a stiff and sore neck. We will also assess movements of your shoulders and upper back to see if any stiffness or other injuries (for example a rotator cuff tear) could be putting extra stress of your neck and contributing to your problem.
Neurological assessment
If you have referred pain (pain into your arm and hand), pins & needles or numbness we will also do a neurological assessment. This means that we do tests to find out if the nerves are affected. Each nerve leaving the spine supplies specific muscles and a specific part of the skin, so we use these tests to check each nerve that could be affected.
Palpation
After taking a history of your problem and doing movement tests, your physiotherapist will assess each level of the neck by pressing on the area. Our knowledge of anatomy and how each area “should” feel & move makes us able to find the levels causing the problem. We also check for tightness and trigger points in the muscles around your neck.
X-ray
The first and most frequently used tool are X-rays. The bony changes can be seen on X-ray. Your report may sound something like this:
“Early onset degeneration, loss of disc height, osteophyte formation, facet joint hypertrophy.” The medical lingo is just a short version of the degeneration discussed above. A disc bulge or prolapse will not be visible on X ray. It may be necessary to have a MRI.
At our practice we try to get hold of old X-rays that shows us 2 points in time in order to determine the rate of degeneration and identify the neck joint levels that might be more at risk, and start there. X-rays from 10 or 15 years ago will be very helpful, even if its outdated, it this case it can serve a very useful purpose.
MRI or CT scan
If you have severe, constant pain in your arm or pins and needles/numbness in both hands you may need an MRI or CT scan to see what is causing pressure on the nerves. An X-ray only shows bone, so to see what’s happening to the nerves, intervertebral discs and ligaments you will need more specialized imaging.
However, these are expensive tests and, if there isn’t any instability or pressure on the nerves, what we see won’t change your treatment. Also, only surgeons can refer you for an MRI or CT scan and this is usually done if they suspect that you may need surgery. Physiotherapy is always a good place to start before seeing a surgeon, because we will do a neurological examination to find out if the nerves are involved. We can then refer you to a neurosurgeon or orthopaedic surgeon if we suspect that you may need an operation.
Sonar (Diagnostic ultrasound)
Diagnostic ultrasound isn’t of value with cervical spondylosis, because it only shows superficial soft tissue like ligaments and tendons. The ligaments and discs in the neck are too deep and all the structures are too close together for a sonar to give useful information.
Why is my pain not going away?
Degenerative spondylosis of your neck is a natural process of aging, so the damage is not reversible. However, these changes in your neck joints doesn’t mean that you should always have pain.
An important principle with cervical spondylosis is finding the balance between rest and activity. You will find that your pain gets worse if you do “too much” and then gets better when you rest. Our goal with physiotherapy is to change what “too much” is.
For instance, you have unbearable pain after a day of working around the house or garden. Our aim with physiotherapy treatment will not just be to get rid of the stiffness and muscle spasm that cause the pain. We will also give you exercises to strengthen the muscles around your neck and shoulders, so that your body doesn’t think that these normal chores are “too much”. If you are stronger you will be able to do more without flare-ups and, if you do have a flare-up, you will need less rest for the pain to get better.
What NOT to do
What you should do
Making the injury worse
A big problem we see with cervical spondylosis
Waiting too long
A big problem that we see with degenerative spondylosis of the neck these days is that people wait until the pain is unbearable before they make an appointment. Some patients have a stiff and sore neck every couple of months for years before they come for physiotherapy treatment. Over time they realize that the pain becomes more frequent and takes longer to go away. If cervical spondylosis is treated in the earlier stages when you have pain once or twice a year, we can treat the stiffness, muscle imbalance and contributing factors before there is severe degeneration. This treatment can then slow the progression of the condition and you won’t reach the stage of constant pain and stiffness.
Soft collar
Using a soft collar or neck brace for a prolonged period of time is also a problem that we see. A neck brace for a couple of days when your pain is unbearable can be useful, but this becomes a problem if you wear the brace every day for weeks. The muscles around your neck become weaker and the brace will push your neck into an abnormal position with your chin poking forwards. This makes your symptoms worse, so you get stuck in a vicious cycle of pain making your wear the brace and the brace causing pain.
Surgery
Another problem we see is that patients go for surgery first and if that doesn’t improve their symptoms they try physiotherapy treatment. Depending on the surgery, this can have a drastic impact on the range of movement we can restore with physiotherapy treatment. For example, after a neck fusion there will be stiffness at that level that cannot be reversed. We can still treat stiffness around the level(s) of the fusion and treat muscle imbalances, but the fusion will result in a permanent loss of some of the movement of your neck.
Physiotherapy treatment of cervical spondylosis
Unfortunately we cannot reverse the degeneration, it is not as simple as that. We can relieve a great deal of your pain and assist you in some lifestyle adaptations that will help you minimize your neck pain. In doing things differently you can slow down the degeneration process and limit painful episodes.
Changing your pillow or posture can greatly change the amount of pain you are feeling. Improving your neck strength will aid in stability and the body would be less inclined to seek stability from osteophytes and muscle spasm. Muscle spasm is one of the main reasons why people eventually decide to come see us.
It is important to find a balance between enough movement to keep the muscles strong and the joints moving, and too much movement that will cause a spike in inflammation and pain. We are able to guide you to find this balance.
Treatment will include:
- electrotherapy, including laser and ultrasound, to help with pain relief
- myofascial release and dry needling to get rid of muscle spasm and tightness
- joint mobilisation to improve or restore the movement of the vertebral joints
- nerve mobilisations to restore the normal gliding movements of the nerves
- taping/strapping to support the area
- exercises to strengthen the stabilizing muscles of the neck and the surrounding muscles to take strain off the neck
- advice and education to help you to understand your condition and know what you can change to be in control of your symptoms.
1st Phase: Protection & initial pain management
The first phase of your treatment will involve lots of information about your condition. We will explain the treatment plan and give you advice on everyday things to help manage your pain like changing your sleeping position or how you sit at your computer.
By the time patients come to see us with cervical spondylosis they usually have a lot of pain and discomfort. During this phase of treatment we will use joint mobilisations and myofascial release to treat the neck stiffness. Electrotherapy like ultrasound and laser will also help with pain relief at this stage. We use strapping or taping to help support and protect the area while we start with gentle, pain free exercises.
2nd Phase: Establish pain free range of movement
During your examination and testing, it’ll become clear what you can do and what makes your pain worse. We identify factors that contribute to your pain, specific to your case. You will have a pain free range of movement and our exercises will be tailored between these boundaries. For instance looking up will be painful, so an example of an exercise might be small nodding movements. This starts strengthening the deep stabilizing muscles in your neck without making your pain worse.
As your rehabilitation progresses we aim to gain a larger pain free range of movement while your painful range becomes less intense.
3nd Phase: Isometric exercises
We may find that all movements of your neck are painful in the first phases of treatment while we work on pain relief and stiffness. This is where isometric exercises come in.
An isometric exercise means that the muscles contract, but the joints don’t move like when you try to turn your head while your hand resists the movement. We use these muscle contractions to help with initial activation of the muscles around your neck. As your pain improves moving your neck will be less painful and your exercises will change to incorporate movement.
4th Phase: Improve range of movement
Neck stiffness – particularly in the mornings – is a characteristic of cervical spondylosis. During our initial assessment we find the movements that are limited and painful. If pain is what limits your movement we will use joint mobilisation, myofascial release and stretches to restore the movements of your neck.
If your degeneration is advanced or severe, there will be a loss of movement that isn’t reversible. Our treatment will focus on restoring the available range and then strengthening your neck muscles to maintain the range of movement we have gained . This muscle strength is very important for long-term improvements in your condition. The stability of your neck improves if the muscles around the neck are stronger, so your body doesn’t have to use muscle spasm and osteophytes to help with stability.
5th Phase: Concentric strengthening
After the initial phases of treatment you will have more pain free movement of your neck. This is when we start with strengthening exercises that include movement. A concentric exercises means the muscle shortens to make a joint move. For example, if the muscles on the left of your neck contract concentrically your head will tilt to the left.
As you progress through this phase and your muscles get stronger we will add resistance to the exercises. This ensures that the muscles will be strong enough to support the structures around your neck when you add load during everyday activities like carrying a heavy box or bag.
6th Phase: Shoulder girdle and upper back strengthening
The shoulder girdle is made up of your shoulder blades, upper back, shoulder joint, breastbone and collar bones. This area is where your neck is attached to the rest of your body. When the shoulder girdle is strong, there is less strain on your neck when you add extra load, like picking up furniture or children.
During this phase of rehabilitation we will add exercises to strengthen your upper back and shoulders while teaching you to maintain the correct position of your neck. Examples of exercises will be different variations of push-ups, ” bird dog” exercises and rowing exercises.
7th Phase: Testing for return to activity
Over the course of rehabilitation we will build up to your previous intensity of normal activities and training. This is important to determine if your condition can withstand the repetitive loading without flare-ups. Our physiotherapist will guide you to reengage in safe increments and adjust your exercises where necessary. We’ll follow your progress and adapt where needed.
8h Phase: Sport Specific Training
This is the final stage of rehabilitation that can last anything from 2-4 weeks. Your physiotherapist will still continue with joint mobilization, myofascial release, trigger point release and electrotherapy modalities where needed, but functional rehabilitation is most important during this phase.
Depending on your sport, your physiotherapist will tailor specific exercises that will help strengthen the muscles pertaining to your sport. A successful outcome is when you have gained knowledge throughout the rehabilitation process and can participate at full power and speed.
Will my condition heal over time?
Cervical spondylosis is a degenerative condition, so we cannot reverse or heal the damage. However, we can make a huge difference to your pain and quality of life. Our treatment plan and how often we need to see you will depend on the severity of your condition and your current pain.
If you have constant pain we will see you twice a week until your pain is under control. Thereafter we will make an appointment once a week to maintain the joint movement we have gained and to increase the intensity of your exercises. As your exercises get progressively harder the time between treatments will increase to two weeks and later a month to check on your progress and adapt your exercises as necessary. You could have a flare-up sometime during the course of treatment if there is a sudden increase in your activity, but this will settle down after one or two treatments, because you have already started the rehabilitation process. Short term discomfort for long term gains.
Without treatment or if you don’t finish your rehabilitation, the pain and stiffness will always return and get worse over time. At some point you will find that you have constant discomfort and or pain that isn’t relieved by rest. Working with your physiotherapist you can make sure that this doesn’t happen.
Other medical treatments
- Your GP can prescribe anti-inflammatory medication, cortisone or muscle relaxants to help with pain relief. Medication is useful in the first week or two of physiotherapy treatment, because it helps to get the pain under control in the acute flare-up, so that we can start with exercises and rehabilitation. Your doctor can also prescribe a short course of stronger pain killers if necessary.
- Using a soft cervical collar (neck brace) for a couple of days can also help to improve your pain. However, the neck muscles will get weaker if you use the soft collar for more than a couple of days, so it is very important to start strengthening exercises as soon as possible.
- Sleeping on a cervical pillow that holds its shape and maintains the curve of the neck can also be useful.
- If your pain doesn’t improve with conservative treatment, a neurosurgeon can perform injections to the specific levels causing your pain. These injections are performed with X-ray guidance while you are under anaesthetic.
- A biokineticist can carry on with further strengthening and rehabilitation after you have completed your physiotherapy treatment.
Surgery for cervical spondylosis
Cervical spondylosis usually responds well to conservative treatment, but if your nerve symptoms – like numbness or weakness in your hands – keep getting worse you may need surgery to save the nerve.
The most common option for degenerative spondylosis of the spine will be decompression surgery depending on the affected area. Decompression surgery can be a discectomy where the surgeon removes the intervertebral disc or a cervical disc arthroplasty where the surgeon does a disc replacement on the affected levels. A fusion is usually performed with the discectomy to improve the stability of that level of the spine.
Also known as:
Stiff, sore neck
Neck degeneration
Cervical degeneration
Neck spondylosis
Degenerative spondylosis
“Wear and tear” of neck joints
Intervertebral disc degeneration
Other causes of a stiff, sore neck:
- Neck muscle spasm – your range of movement will not be affected as much as with cervical spondylosis
- Cervical Disc injury (Slipped neck disc) – pain will have an acute onset
- Interspinous ligament sprain – your pain will be more localised to a specific spot
- Pinched nerve in the neck – the pain in your arm will be more severe that your neck pain
- Cervical Facet joint sprain – pain will have an acute onset and be more localised
- Whiplash – your pain will have started after a specific incident like a fall or a car accident