An aching, gnawing pain deep in your buttock when you walk or run. A tingling feeling together with pain spreading down the back of your thigh. Even when you’ve been sitting for a while, you feel your buttock pain getting worse. This is what piriformis syndrome feels like. You can literally call it a ‘pain in the butt’ because piriformis is a buttock muscle. With piriformis syndrome, this muscle gets overworked or stretched too far, causing muscle pain and sometimes symptoms of sciatica-like pins and needles and burning pain down your leg.
It is important to find out what is causing your piriformis muscle to get overworked and tight. That will be the only way to prevent piriformis syndrome from simply returning.
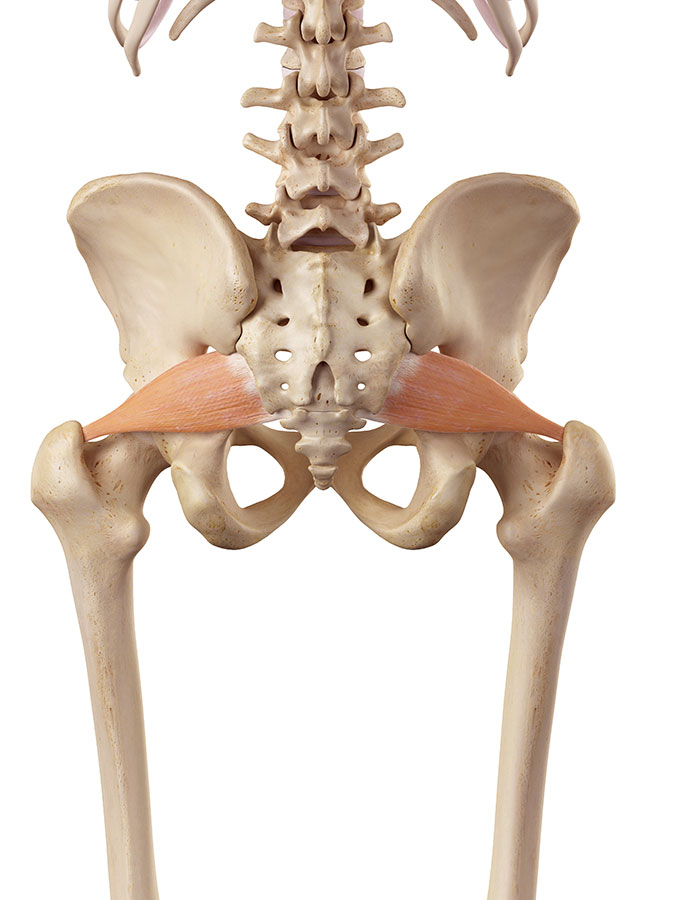
The structure of your piriformis muscle
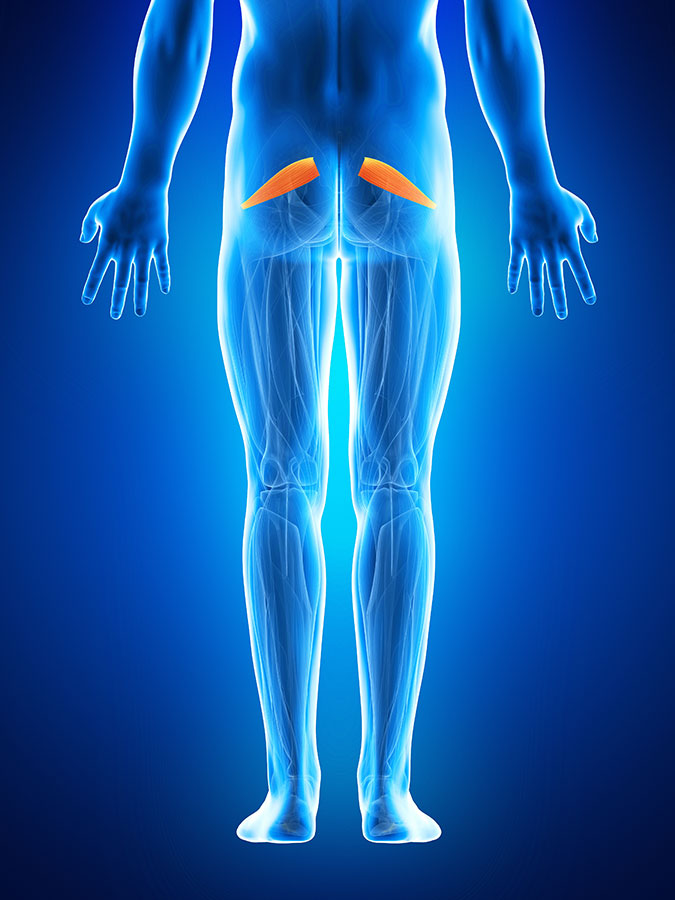
The piriformis muscle is deep in your buttock, underneath other layers of muscles. Its name (piriformis) has a Latin meaning, describing the muscle’s pear shape. The fat end of the piriformis muscle attaches to the sacrum, and the thin end connects to the top of the thigh bone. You have a muscle like this on both sides.
The surrounding anatomy
You have to examine the structure of your lower back to understand fully how your piriformis muscle works because it attaches directly to your lower spine. The lowest part of your spine is where your lumbar vertebrae connect to your sacrum and coccyx. Each bone is numbered according to the level it is on. Your lower back is numbered L1-L5, and your sacrum (sitting bone) is numbered S1-S5.
Between each vertebra, there is a disc and a nerve root that exits on each side. Nerves are like power cables, giving the right kind of impulses to your muscles so that you can move. The nerve roots from level L4 – S3 in your spine merge to form the sciatic nerve.
The sciatic nerve
The sciatic nerve runs from your spine deep through your buttock, down the back of your leg and into your foot. It is the thickest and longest nerve in your body. This nerve allows muscles in your leg to move and allows the skin around your leg to feel different sensations like pain, pins and needles, and different temperatures.
Your sciatic nerve and piriformis muscle cross paths along the way
As the sciatic nerve passes deep through the buttock, it passes underneath the piriformis muscle. They directly cross paths. Some people have an anatomic variation where the sciatic nerve runs through the Piriformis muscle instead of underneath it. In either case, the contraction of the piriformis muscle can irritate the sciatic nerve. A ‘spasmed,’ tight, or shortened piriformis won’t allow normal sciatic nerve movement, leading to sciatic nerve compression. Ultimately leading to nerve symptoms of burning pain and pins and needles spreading from your buttock down your leg.
What does your piriformis muscle do?
The piriformis muscle turns your hip outwards, turning your hip, thigh, and toes to face outwards. It also assists with lifting your leg sideways (away from your body) and helps stabilize your hip when you stand on one leg. You use your piriformis muscle for any activity where you balance on one leg, such as walking, climbing stairs, running, and getting in and out of your car.
Your piriformis muscle can contract and shorten (concentric contraction) but also lengthen with control (eccentric contraction). This eccentric kind of contraction is essential for hip stability. Other buttock muscles, like your gluteus medius and minimus, rotate your leg inwards, which puts your hip joint in an uncomfortable position. The piriformis muscle works to oppose this by contracting eccentrically, keeping the hip joint in a neutral position. This counter-rotation force that the piriformis muscle must control leads to thickening, shortening, and hypertrophy.
I think I have piriformis syndrome. How did it happen?
It starts with a muscle injury.
While running uphill one day, you feel a muscle ‘pull’ in your buttock. Initially, you only feel a deep, aching muscular pain in your buttock, and luckily, it seems to go away when you rest. This is the start of piriformis muscle pain. An injury to the piriformis muscle, whether a direct fall, strain, stretch, or repetitive overuse injury, leads to inflammation in the muscle tissue. This causes a deep, dull ache in the back of your buttock area, which gets worse when you try to contract or stretch it.
Now, the pain starts to spread down your leg.
Inflammation is a normal part of the healing process. However, taking an already tight and shortened piriformis muscle and adding swelling and inflammation to the area is a recipe for more problems. It irritates your sciatic nerve, which runs directly underneath your piriformis muscle. The sheath around your sciatic nerve gets compressed, and the friction between the piriformis muscle and the nerve is higher than usual. Your sciatic nerve is literally getting ‘rubbed the wrong way.’ This causes a burning type of pain and a sensation of pins and needles that sometimes travel down the back of your thigh. These symptoms are a warning sign that your sciatic nerve is irritated and not getting enough blood supply.
The pain gets so severe it stops you in your tracks.
You tried to push through the pain by continuing to exercise. Maybe you even tried to stretch out your piriformis and buttock muscles or tried to roll it out with a foam roller. Nothing is helping. Instead, it seems like it is getting worse. That is because your piriformis muscle has gotten even more overworked and stretched too far. And the irritation of your sciatic nerve has gotten worse. Now, it is getting squashed and strangled. Your buttock pain is severe and constant. Even sitting down to rest gives you pain. The pain spreads down the back of your thigh, leaving your leg feeling weak and clumsy.
At this stage, you can not exercise, climb stairs, or even walk without pain shooting down your leg. You don’t know which is better, to rest or move, because sitting is just as painful. This pain has literally stopped you in your tracks and brought your life to a standstill. Nerves are very sensitive structures and if the compression on your sciatic nerve is not somehow relieved, it can lead to nerve damage.
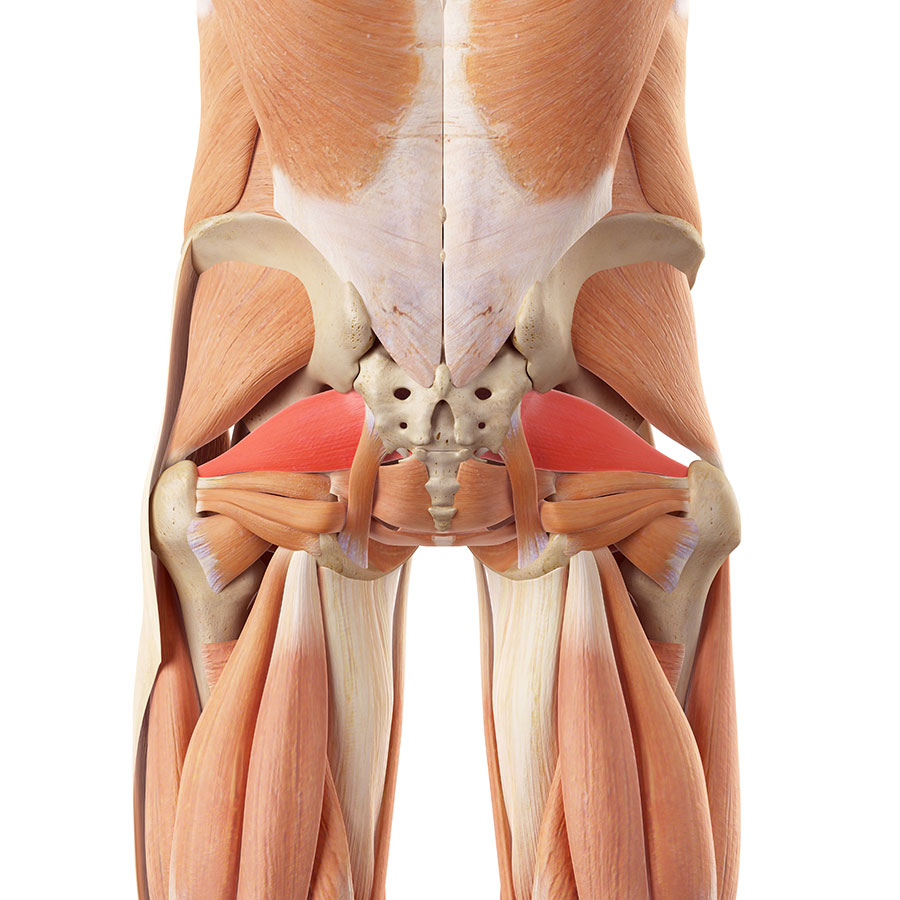
Piriformis syndrome is not just a muscle injury.
Piriformis syndrome is a collection of symptoms that come not only from your piriformis muscle but also from the sciatic nerve. It can easily be confused with sciatica because many of the symptoms overlap.
That is why it is so important to find out what exactly is causing your piriformis muscle pain and where exactly your sciatic nerve is getting irritated. Treatment for piriformis syndrome should aim to find the true reason for your piriformis muscle pain, which started everything in the first place.
Causes of piriformis syndrome
Piriformis syndrome can be caused by any one or a combination of these problems.
Weakness of the piriformis muscle
Not getting enough exercise is the main reason for muscle weakness. A weak piriformis muscle won’t be able to give a muscular contraction and quickly becomes fatigued. Even if you are active during your workday by climbing a few flights of stairs or walking a lot, it is not enough to count as exercise. Exercising specifically targeting your buttock muscles is the only way to strengthen your piriformis muscle.
Weakness of other buttock muscles
Your gluteus muscles make up most of the shape of your buttocks. They are big muscles capable of performing strong hip movements and stabilizing your hip joint. However, if they are not strong enough, your piriformis muscle is the next muscle to activate to try to take over. This causes your piriformis muscle to do double the work and become overworked and fatigued.
Posture
Your piriformis muscle attaches to your spine, lower back, and hip. Your posture influences how you stand, sit, or exercise and will affect how you use your piriformis muscle. An example of this is if you have a very hollow lower back. A hollow back puts your pelvis in more of an anterior-tilted position. Your buttock muscles, especially the piriformis muscle, are placed in a lengthened, stretched position the whole time. Eventually, it leads to more tension and tightness in the muscles as they work harder. Now, imagine you try to exercise or run where you need your buttock muscles to contract forcefully and repeatedly. You end up in pain due to overuse of your piriformis muscle, caused by an underlying postural problem.
‘Pulled’ piriformis muscle
Let’s say you were exercising to work on buttock muscle strength. You stepped it up and added an extra weight or added more resistance. But this time, when you did the exercise, you felt something ‘pull’ in your buttock. This is what we call a muscle strain. Your piriformis muscle got overstretched and had to contract under so much pressure that it led to a muscle injury and tear, which needs time to heal. The scar tissue that forms during this healing process can attach to your sciatic nerve. This is not normal, as a contraction of the piriformis muscle will pull on the nerve branch.
Lower back problems
Injuries like a herniated disc or osteoarthritis in your lower back decrease the stability of your spine. Your lower back muscles will already be working hard to stabilize your spine. Even your buttock muscles need to work harder and do double the work, which leads to your piriformis muscle being overworked and shortened. Here, the piriformis muscle is a secondary problem to a problem elsewhere.
The only effective treatment for piriformis syndrome is to look for the exact cause of why your piriformis muscle is causing you pain. Posture, habits, and wrong movement patterns are often the biggest culprits for piriformis syndrome.
How bad is it?
It starts out with a deep aching pain in your buttock that you are constantly aware of. For a while, you feel like you can still push through it and try to exercise in the hopes that it will go away. However, with time, it gets worse. Now, your pain bothers you throughout your whole day. You can’t go for a run or sit for too long, and even something as simple as putting on shoes is becoming hard to do.
This is where nerve irritation starts
With time, you start to feel other symptoms as well. Instead of only pain in your buttock, you feel your pain spreading down your thigh. Previously, it was an aching, gnawing pain. Now, it is becoming sharper and burning. You even feel a tingle, like pins and needles, running down your leg, especially when you have been sitting for a while.
This is what we call intermittent irritation of the sciatic nerve. In certain positions, like bending, your piriformis muscle and sciatic nerve get stretched and irritated, causing nerve pain. Whereas a position like sitting puts more pressure directly on your buttock muscles and sciatic nerve. You feel the familiar tingle down your leg when you try to walk fast or even run. When your piriformis muscle is contracting, the irritation worsens. The irritating symptoms down your leg seem to improve whenever you lie down. We call it intermittent nerve irritation because it comes and goes.
It gets serious
Now, the intermittent irritation that only bothered you at times has progressed to sciatic nerve compression. You start to feel like you’ve lost power in your leg and hip, and some patches of skin on your leg feel completely numb. Weakness or clumsiness of your leg may not be as excruciating as the burning pain, but it is more serious.
If you’ve gotten to this point, your sciatic nerve is suffocating and cannot properly conduct impulses. This will lead to nerve damage if you do nothing about it. Your piriformis muscle has gotten so overworked, tight, and shortened that it cannot do its job anymore. Now, other buttock and lower back muscles are taking over, leading to muscle spasms in other areas. Prolonged dysfunction of your piriformis muscle may cause the muscle tissue and tendons to become scarred, making a normal, smooth contraction of the muscle so much harder.
Your piriformis syndrome symptoms have gotten so severe that they are affecting your life, sleep, work, and exercise. The pain from this is so severe you will feel like you don’t want to move at all. You’ve gotten to a point where the pain is no longer only a warning. You are damaging your piriformis muscle and sciatic nerve. Do something about it!
Chronic, recurring piriformis syndrome
Chronic flare-ups of piriformis syndrome are very frustrating and debilitating. You never know when you’ll feel it again, and it always stays in the back of your mind, leaving you afraid of the pain you know too well. You can never run or exercise to your full ability again because you know that you don’t want to push yourself too far for fear of a flare-up. Finding the true cause of your piriformis syndrome is the best way to clear it up. The longer you have piriformis syndrome, the higher your chances of having permanent muscle and nerve damage.
Diagnosis
Our physiotherapists are experts in human anatomy and movement and have the necessary experience to diagnose piriformis syndrome easily. We fully understand how muscles and nerves work and can accurately diagnose what is causing your piriformis muscle pain. The starting point is a clinical assessment and getting the necessary information about your pain.
During your physiotherapy evaluation, we will stretch and stress your piriformis muscle and sciatic nerve, as well as structures in your lower back, hip, and knee. We also look at the mechanical interface, which is all the layers of tissue and muscles surrounding the nerve. Your sciatic nerve should be able to glide and move between these layers of tissue. During our examination, we test everything.
Movement and sensation:
Suppose your piriformis syndrome has gotten to such a point where you are feeling spreading pain, pins and needles, numbness, or weakness. In that case, your evaluation will include further testing for sciatic nerve function. Your sciatic nerve is responsible for two critical things. Movement and sensation. Testing movement (motor function) by looking at muscle strength, length, reflexes, and range of movement. To test your sensation, we will test your ability to feel soft touch, sharp pain, and different temperatures. Our thorough evaluation makes our physiotherapists the best at diagnosing this problem.
X-rays
Soft tissue, like muscles and nerves, cannot be seen on X-rays. However, X-rays show the integrity and alignment of the lumbar spine, sacrum, and hip position. This enables us to see if something is wrong with your hip or lower back structure, and we can determine whether the source of your piriformis syndrome could be your hip or lower back.
Your physiotherapist will refer you to get x-rays taken if deemed necessary.
Diagnostic ultrasound
Diagnostic ultrasound is effective in showing different layers of soft tissue. It shows compression on your sciatic nerve by measuring its diameter before it crosses the piriformis muscle and after, which can visualize the compression. Sciatic nerve irritation will show thickening of the muscle, oedema, or even scar tissue around the nerve pathway.
If deemed necessary, your physiotherapist will refer you to get an ultrasound.
MRI
An MRI shows all of the structures of your lower back and pelvis, including soft tissue like muscles and nerves. Because it’s a much more detailed scan, it may show signs of sciatic nerve irritation, but remember that it’s an image taken in a still-rested position, and it may not show up. That is why a diagnostic sonar is opted for.
An MRI is an expensive test, and you need to be referred by a specialist for one. If you have already had an MRI, please bring it along to your first consultation. If your physiotherapist feels it is necessary, you will be referred to a specialist.
Why is my buttock pain not going away?
Let’s say you have had piriformis syndrome before and even tried treatment like medication and rest. Previously, it helped because your pain got better. However, when you try to get back into running or exercising at your full capacity, your pain returns. Now, you’re always aware of the pain in your buttocks, and you wonder if it might trigger that familiar burning pain down your leg.
Finding the root of the problem
It is essential to not only get treatment for the pain that you’re feeling but to find out precisely what is causing your piriformis syndrome. That way, you will know what is causing your pain and what you can do about it. Years of bad habits, poor posture, or lack of exercise will lead to weakness of the entire hip. If you do not take the time to complete your strengthening and rehabilitation, your pain will always return. Without a proper evaluation and treatment plan, your piriformis muscle dysfunction won’t simply improve.
Is it better to rest or to move?
If you focus on resting, it will probably help the inflammation and nerve irritation will settle. However, now you get weaker, and your buttock muscles won’t cope with the load when you get active again. Now, your piriformis muscle gets overworked again, and the repeated muscle contractions flare up to the point of irritation and inflammation in your sciatic nerve. This leaves you in a cycle of pain, not knowing if it is better to rest or move. Trying to push through the pain to get back to exercising will cause you to injure your piriformis muscle and sciatic nerve, leading to permanent damage if it is repeatedly injured.
Problems that pop up when we see patients with piriformis syndrome
Waiting too long and not getting a proper diagnosis.
The common problem is that patients wait too long before seeking help. By the time patients come to see us, they have had piriformis syndrome for months. If you don’t get a proper diagnosis from the start, it will waste time. If anyone treating your pain is not also looking for the cause of your piriformis muscle dysfunction, they will keep on treating the incorrect thing. This is ineffective. Now, the pain becomes unbearable; it holds you back from doing normal day-to-day activities, and it will take so much longer to heal.
No pain, no gain
People try some home treatments, like foam rolling or piriformis stretches, without much success. Taking an approach of ‘no pain, no gain’ or ‘pushing through the pain’ is actually not a good idea when it comes to piriformis syndrome. There is a big chance that your pain will flare up, irritating your sciatic nerve.
Trying out but not completing different forms of treatment.
Often, patients try to get relief by taking anti-inflammatory medication or getting a cortisone injection in the hopes of easing their pain. This, however, only slows the healing process. Simply taking medication does not address the root of the problem. Many people then tend to get impatient and stop taking their medication and stop their treatment plan as soon as they feel better.
Resting too much or too little
Resting too much leaves you weaker than before. Moving too much causes extra inflammation and irritation. Finding the balance between resting and doing safe movements is critical!
Physiotherapy treatment for piriformis syndrome
We understand that patients are often anxious to return to their daily routine and exercise, so we are here to provide guidance and answers. Our Physiotherapists implement a very effective and structured plan of action that treats all the aspects of the problem and gets you back to where you want to be. Our treatment program plays a vital role in restoring the normal smooth contraction and stretch of the piriformis muscle without irritating your sciatic nerve.
Our priority is to determine the extent of the damage to your piriformis muscle. Then, we test the structures surrounding your hip and lower back to clear the nerve pathway and resolve the sciatic nerve pain. Avoiding nerve compression is crucial to prevent relapse and restore the sciatic nerve’s regular sliding. We must protect the muscle from overworking by differing forces away from the piriformis muscle, strengthen the surrounding muscles, correct the compensation, and retrain the correct firing pattern. This allows time for the piriformis muscle to adapt and heal. Our practitioners bring on a change and monitor the results until it’s working, and then we magnify the effects to get even better outcomes.
Your treatment goal is to restore the normal movement of your piriformis muscle without irritating the sciatic nerve. It must be able to stretch into the end of its range. The muscles and nerves should be able to move and glide without obstructions to give you full flexibility. Your physiotherapy treatment involves working on muscle strength, range of motion, flexibility, and stability. Treatment techniques include soft tissue massage, joint mobilizations, dry needling, strapping, laser therapy, nerve mobilizations, and guiding you through a rehabilitation program of gradual strengthening, control, and conditioning. You must commit to the treatment plan because it improves your chances of successful long-term recovery.
Phases of rehabilitation
For patients with piriformis syndrome, it’s important to prioritize rest and the use of crutches to alleviate the load on your buttocks and hip. Strapping or using an elastic bandage provides support to the piriformis muscle. Avoid using anti-inflammatory medication continuously, and instead use pain medication without anti-inflammatory components to control pain. Get information directly from your healthcare provider to make better decisions about your treatment. Gradually return to normal activities while allowing your pain to guide you and finding a balance between rest and movement.
2nd Phase: Establish pain free range of movement
During your examination, it will become clear what you are able to do, and what you should avoid. We identify factors that contribute to cause your pain, specific to your case and will address these factors as your treatment progresses. When doing a movement, like crossing your legs to put on socks and shoes, you will be able to move to a certain point, before your pain starts. This is your pain-free range of movement. You are safe to move in this range and our exercises will be targeted between these boundaries of your pain.
The aim is that, with time, your pain-free range of movement improves and painful movements become less intense.
3d Phase: Tissue healing
We monitor the progress of the healing of piriformis muscle and sciatic nerve and track the formation of scar tissue at the site of irritation. On a cellular level we’re able to accelerate tissue healing using dry needling, laser and ultrasound. As healing takes place, we want to see not only improvement of your pain, but also improvement in the piriformis muscle’s ability to contract and stretch and a decrease in sciatic nerve irritation.
4th Phase: Soft tissue and nerve stress
During each session we will re-evaluate to see if you are achieving the necessary targets for the piriformis muscle and sciatic nerve to be able to handle tensile, elastic and compression forces. The piriformis muscle should be able to take load and contract harder without causing further irritation to the sciatic nerve. We start with small movements and minimal load and gradually get you used to more. We use isometric muscle contractions to start with. These are muscle contractions without much movement. This is to prevent further flare-ups of inflammation and irrtiation to the sciatic nerve.
5th Phase: Full range of movement and nerve mobility
To regain full range of motion of your hip, back and leg will be a very important component of your rehabilitation. The piriformis muscle should be able to stretch to the end of its range and the sciatic nerve should be able to glid smoothly underneath the piriformis muscle. Any scar tissue that might have formed in the muscle tissue can cause irritation of your sciatic nerve again. The mechanical interface and scar tissue must be lengthened and orientated to allow a smooth contraction and stretch of the piriformis muscle as well as the sciatic nerve. We will help you to stretch more, move deeper and work into your pain. For this we use massage, stretches and joint and neurodynamic mobilisations to achieve full range of movement.
At the end of this stage of rehabilitation, you should be able to comfortably lift and turn your leg and hip, making it easier to do a typical piriformis stretch in a cross-legged position.
6th Phase: Muscle strength
During this phase of your rehabilitation, you will work on strengthening not only your piriformis muscle, but your hamstrings, lower back muscles and buttock muscles. Repeated contraction of muscles, improves their strength. Stronger muscles have the capacity to work harder and can help to carry the load while keeping your hip stable. If your piriformis muscle doesn’t have to do all the work and become tight and overworked, there won’t be as much irritation on your sciatic nerve. We will progress your exercises more and more, adding resistance, doing more repetitions and building your overall strength.
Now, you should be able to walk, sit and get in and out of your car with ease.
7th Phase: Muscle control and stability
It is one thing to feel your muscles get stronger, but another thing to feel like you have control when you move. The type of muscle contraction we use during this phase of rehabilitation is called eccentric muscle contractions. Muscles are able to contract and shorten concentrically, but they are also able to slowly lengthen eccentrically. Climbing up and down stairs or standing on one leg when you put on pants are some of the things that require control and stability coming from your hip and buttock muscles.
8th Phase: Testing for return to activity
A big part of your recovery is to gradually return to your routine again. This way, we can determine if you are ready to return to fully working and training without any flare-ups of piriformis syndrome. Your physiotherapist will guide you to re-engage in safe increments, and make adjustments where necessary.
9th Phase: Balance, high speed and power
Now that you’ve worked through the different phases of your rehabilitation, we want to improve the power and speed of your piriformis muscle contractions. You need to be able to do activities with precise balance, high load, and speed to ensure that your buttock muscles are able to keep up with the demands of your body.
Your physiotherapist will guide you to return to normal activities but will also challenge you past your normal boundaries to determine how your body reacts to different forces. Ultimately we prepare you to return to participating in your sport.
Whatever must be done – we’ll get you there. Running, sprinting or jumping and much more.
10th Phase: Sport specific training
This is the final stage of rehabilitation. Depending on your sport, your physiotherapist will tailor specific exercises to further improve your strength and endurance. A successful outcome is when you understand your condition, know how to prevent flare-ups and can participate at full power and speed, not to mention the benefits of minimizing your chance of future injury.
How long will it take for me to recover?
The treatment of piriformis syndrome addresses the piriformis muscle and the sciatic nerve. A piriformis muscle strain should heal within 6 weeks, given that you follow your physiotherapy treatment program and finish your rehabilitation. Sciatic nerve pain could take longer to improve, depending on the severity of the nerve irritation or compression. Nerves are susceptible structures and could take months to heal, even longer if there is nerve damage.
Some days will feel better than others.
Recovering from piriformis syndrome will have its ups and downs. You might feel better for a few days and worse for the next few because nerves are extremely sensitive structures that tend to flare up quickly, causing further inflammation and irritation. Just be prepared that your recovery process will be more of a cycle with ups and downs than a constant improvement from day 1.
Physiotherapy must start while your nerve is healing. If you have followed through with our treatment program, you should be able to recover completely and return to whatever you want to. You will need physiotherapy treatment twice a week for the first two weeks. After this, if you achieve the milestones, your treatment sessions will be spread out to once a week. This allows us to monitor your progress closely.
Other forms of treatment
- Your doctor may prescribe anti-inflammatory medication or give you a cortisone injection or nerve block as a treatment for piriformis syndrome and sciatic nerve compression. Both of these medications will temporarily relieve the pain and inflammation you are experiencing. However, they will not be the solution to your problem. And once the medication’s effect wears off and you try to get back into your normal routine, your pain could simply return.
- Steroid injections are not recommended in most cases, especially those with chronic conditions.
- Getting your lower back or hip ‘aligned’ or ‘clicked’ in the hopes of easing your pain will not change your pain. An alignment cannot change the strength or contracting pattern of your piriformis muscle. It could even worsen the irritation of your sciatic nerve. You need to look at the bigger picture.
- A biokineticist can help you in the final stages of your rehabilitation or get you back to actively training for your sport.
- Foam rolling and stretching your piriformis muscle might give you some momentary relief. However, you can easily overdo it and irritate your sciatic nerve further. Stretching your piriformis muscle alone will not change its strength. So, if a weak piriformis muscle is the cause of your pain, then you need to look at rehabilitation and strengthening.
Is surgery an option?
Surgery for piriformis syndrome will only be an option if you have had persistent and severe pain with severe sciatic nerve compression that leads to weakness, numbness, and clumsiness of your leg for more than 3 months and only after proof that non-surgical treatments have failed. Even with persistent nerve compression, a neurologist will help to decide if there is a chance that your sciatic nerve could be damaged. Then, our focus will shift from preservation to nerve protection, and surgery will be your next step.
Surgery is performed to relieve the compression on your sciatic nerve, and depending on the type of surgery done and on your surgeon’s orders, recovery from surgery can take you anywhere between 6 weeks and 6 months. Physiotherapy can still help you during the time of your post-operative recovery.
What else could it be?
- Herniated disc: A herniated lumbar disc causes pain in the lower back. It feels worse when you bend forward, sit, or drive.
- Lumbar osteoarthritis: Degeneration of the joints in your spine happens as you age. It causes a loss of disc space and bone spurs to form, which leads to pain when you move. The pain gets worse in cold weather, and your back feels stiff in the morning.
- Sciatic nerve pain: Irritation or compression of the sciatic nerve causes pain in the buttocks and down the leg. You may also feel pins and needles, numbness, or weakness in your leg.
- Gluteus Muscle Strain: A tear in your gluteus (buttock) muscles. It is painful to climb stairs or walk uphill.
- Hip Bursitis: Pain over the side of your hip bone. It feels significantly worse when you lie on your side.
- Lower back muscle spasm: Painful, ‘pulled’ muscle in your lower back. It’s worse when you bend over or try to pick up something heavy.