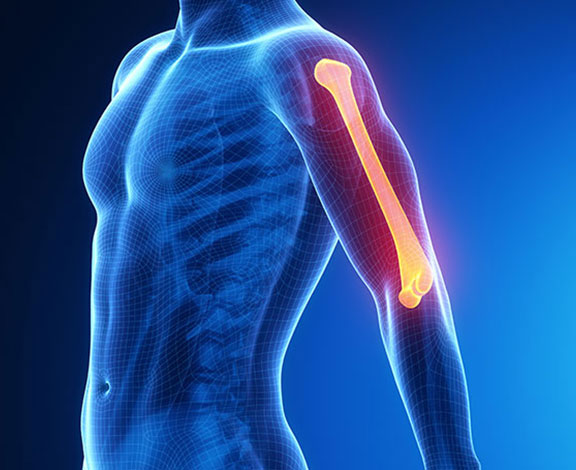
Everyone feels some form of shoulder pain at some point in their life, the questions is – when is it serious. Constant pain that doesn’t react to medications, heat or change in position. That’s your warning signs that you’re in for some trouble. The first step is to determine the underlying cause of your shoulder pain, then treatment can be focused on that specific structure. Your shoulder is made up out of muscles, tendons, ligaments, nerves and 3 joints. Any one of these can be the culprit. And starting treatment without knowing what you’re dealing with is going to leave you more frustrated in the coming weeks. Get an expert’s eye to give you a clear picture what you’re dealing with. Or you might up causing more harm. Let’s look at the different types of structures in your shoulder and how injury or damage to them causes pain.
We treat patients with shoulder pain daily. This is because the shoulder is one of your body’s most mobile joints, and very vulnerable to injury. When the mobility of the joint is increased, stability is sacrificed. For this reason, your shoulder is prone to injury, especially traumatic or overuse injuries.
It’s very common to find neck pain involved with shoulder pain. This makes sense, because shoulder and neck injuries often overlap. The shoulder is one of the most challenging areas of treatment for any sport medicine practitioner. The complexity makes shoulder conditions difficult to diagnose and can cause rehabilitation to be a lengthy process.
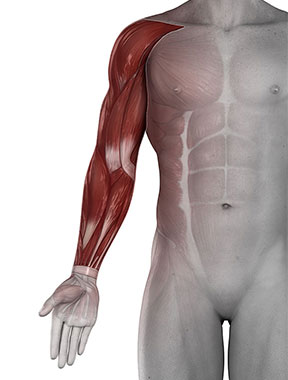
What causes my shoulder pain?
To understand where your shoulder pain is coming from, you’d have to determine how you injured it, or if you can remember when it started. Some are outright obvious like when a fall onto your shoulder, meanwhile others are subtle and creeps up on you – getting worse day by day. So, it’s easier to establish how your pain started and changed until now. Changes in your shoulder pain gives us many clues to understand where your pain is coming from.
Your shoulder consists of various types of tissue, some elastic like tendons, or strong like cables (ligaments), some tissue can generate movement & force like muscles. The structures in your shoulder is quite vulnerable to injury, especially overuse injuries. There are more than 82 structures in your shoulder that can get injured. Some problems are more common than others, but just to be safe – we test them all.
Here’s a breakdown of a few conditions that we frequently see, and how things go wrong to cause your shoulder pain:
Get to the root of your shoulder pain
Different structures, cause different types of shoulder pain, although these are not concrete it’s a good guideline to which structure produces what type of pain
- Muscle — Dull ache or stiffness, sharp pain with contraction, pain comes & goes
- Nerve — Numbness, tingling, weakness, electrical stabbing feeling
- Tendon — Burning pain with certain specific movements
- Joints — Constant stiff feeling, worse after rest, better with movement
- Labrum — Pinching pain, pressure increases or decreases pain immediately
- Bursa — Pain only comes on after being active, better with rest
- Bone — Constant pain, sharp pain with certain movements
- Cartilage — Sharp pain when at certain point, painful arch of movement
- Ligament — Pain at the end of range, unstable, clicking
- Referral from other joints — Difficult to pinpoint pain, vague painful area
Causes of Shoulder pain
- Trauma – dislocations, fractures, labrum injuries, muscle strains and ligament sprains
- Overuse – Tendon inflammation, labrum injuries and arthritis
- Instability – Impingement of rotator cuff muscle (swimmer’s shoulder)
- Autoimmune – Adhesive Capsulitis (Frozen Shoulder)
- Referral from other joints – Acromio-clavicular joint, sterno-clavicular joint, neck
- Visceral referral – Diaphragm, gallbladder, heart, top part of lung and spleen
- Nerve impingement – Usually in the neck
Size – The larger the area of your shoulder pain, is better, because muscles in your shoulder stretches from your neck to your upper arm. Pain tends to radiate along the neck muscles and affect larger areas. Muscles heal easier & recover faster.
Color – Bruising around the outside, back and in your armpit is quite common after a muscle tear, because of the high concentration of blood vessels in your shoulder. These capillaries rupture & leak plasma that pools in your shoulder. Blue discoloration in your armpit is more concerning for it involves nerves running to your arm.
Swelling – Swelling is your body’s way of healing itself by sending cells to heal the tissue. More swelling could mean more tissue damage, however not all shoulder injuries swell. Injury to tissue that develops over a few weeks doesn’t swell, because the tissue trauma is continuous and repetitive, so your body stops the inflammatory reaction. A new injury on an old problem is also possible.
Area – Shoulder pain that you’re able to pinpoint is less severe. Sharp pain over a small area makes it easier to pinpoint structures near your pain. Vague, dull & deep shoulder pain takes longer to identify the root cause. Compensatory patterns, spasms and guarding develops, sometimes it takes a while to just get rid of those.
Motion & sore shoulder
Stiff – Shoulder stiffness followed by pain is regressing and getting worse. Seek help. Whereas pain followed by stiffness is a good sign of tissue healing. Scar tissue is hardening wound tissue that tends to shorten and pull on structures surrounding the injury site. This is more pronounced in muscle strains & tears, where the normal slide of muscles are restricted during a contraction.
Range of movement – Difficult moving your shoulder through its range is a big problem. A painful arch means it only takes tension over that specific range i.e Your shoulder is only painful when you lift it up the between 60 to 90 degrees. Shoulder pain over a smaller range of movement is not necessarily better. This may point to muscle tears combined with instability and likely some ligament injury. Pain only at the end of your range its less severe and easy to fix. When your shoulder pain stops movement completely and too painful to move you should definitely come see us as soon as possible.
Monitor over time:
Intensity – When you grade your pain from 0 – 10. You may think it’s not that bad because it’s not that painful. On the contrary, pain intensity is not a reliable sign of how severe your tissue injury is for example, complete ruptures of ligaments are less painful than partial tears. When fibers are stressed while it’s anchors are completely loose, there’s not much pain, but fibers that are partially torn will produce severe shoulder pain. People have different pain thresholds, so be careful to ignore your shoulder injury.
Frequency – Pain that’s fleeting or intermittent, short burst of pain must not become more frequent and constant. This shows that the tissue damage is not getting any better. Pain that only lasts for a few seconds tend to heal faster, so the longer your pain lasts the faster you should get to us. Pain that is persistent must be stopped before you’re in agony.
Latency – If your pain lags to come on and builds up over the day you must be very cautious. This is a sign of a relapse of your tissue pathology. It’s difficult to judge what makes it worse, because the pain only comes on a few hours after your activity, and not during. Nerve irritation is one of the conditions that has this unique sign where it comes on with revenge in the afternoon.
Loading – Pushing through your shoulder pain while you train or go on with life, is not a good idea. Putting compromised tissue under strain is dangerous. Would you tow a car with a partially torn cable? No! Because it just needs that final pull or jerk that could cause catastrophic tissue damage. Loading soft tissue without knowing what it’s able to handle is dangerous & reckless. What you’ll notice (if you just push through) your pain free shoulder range of movement gets smaller.
Diagnosis of shoulder pain
Our physiotherapists know and understand the intricacy of the anatomy of your shoulder. There are many structures to test, and we even consider the complex biomechanics of your upper arm & neck movements. We’ll accurately diagnose which structures are involved, and to what degree.
During your evaluation, we’ll be stretching & stressing the soft tissue structures like muscles, ligaments, nerves, joints and tendons. This way we can diagnose muscle tears, ligament sprains, tendinitis’s and nerve irritations. We’ll test different aspects like muscle strength, range of motion, flexibility and stability in order to confirm how severe your tissue damage is, which will dictate your treatment plan.
Gathering information through our evaluation allows us to make a diagnosis. Then we’ll customize the shoulder treatment to your specific needs. Therefore our physios are the best at diagnosing shoulder pain & shoulder injuries.
The Process of Diagnosis:
There is a misconception that medical practitioners are able to know exactly that’s the problem the moment we see our patients. People tend to point to their shoulder and say, “treat it”. As if we already know what’s the problem by just looking at it. Sorry to disappoint, but unfortunately this is not how it works. Let me explain:
Diagnosis is a process of exclusion, not inclusion. Medical professionals are taught a process of elimination and deduction to identify the most possible diagnoses for your shoulder pain. The better you can describe & elaborate on your pain, the better picture you’ll give your Physio to understand what’s happened.
Our practitioner uses their skills to eliminate diagnosis’s it’s not and zoom in on your problem. This elimination brings us to only a few possibilities to what could be causing your shoulder pain. Then we test & assess all our possibilities to get to the root cause. In many cases your main problem is not at the site of your pain due to compensation, guarding or even protective muscle spasms. Our shoulder treatment program aims to get the answers you’re looking for.

Our professional experience in the treatment of shoulder injuries
Shoulder injuries are common in most sports but happen more often in contact sports. Suffering from a shoulder injury or shoulder pain can affect and limit your activities in ways you wouldn’t expect. You may have taken some movements for granted, for example opening a pack of chips, washing, dressing, putting clothes on, carrying children and reaching into cupboards to name a few.
After a shoulder injury your shoulder tends to compensate by using the opposite hand. Your brain even eases he strain off the injured shoulder by recruiting other muscles to help with the work. For example, your shoulder will rely more on neck, back or arm muscles to perform actions. As a result, your shoulder pain might subside, but the injury and damage to the underlying structure of your shoulder is still there.
We often hear patients avoiding certain movements. Some patients stop reaching overhead because it is too painful even years after the original injury. If the injury is left untreated, your shoulder problems can escalate and become even worse or develop into chronic shoulder pain.
Physiotherapist treatment
We have seen many patients with shoulder pain and provide the best possible treatment for a faster recovery. Pain and stiffness after a shoulder injury prevents you to move and you might feel hesitant to move, or scared you’ll damage it even more. We know that you’re anxious about the unknown, so that is why we are here to guide you and give you all the answers.
Your shoulder pain treatment will be tailored according to various factors, but just to give you a broad idea, our focus of our treatments are. Firstly to establish which structures are injured in your shoulder, and how bad is it. This puts the scope of the problem into full perspective. Usually there’s a knock on effect, where a few structures are involved, but we must determine what’s the order of priority. We even explain the extent of damage & the intricate details of your shoulder pain & how it may cause other problems.
Secondly, we must protect your shoulder from further injury and stop it form getting worse. Thirdly, we set the ideal conditions for tissue to recover. Now we can even accelerate and speed up your recovery and get tissue to heal. The last aspect of our process is monitoring your progress as you get better, making sure you achieve the goals and milestones. We adapt your program to the stage of healing you’re in.
Well Health Pro
Our team of experts can diagnose, test and treat any kind of shoulder pain. We work together to get rid of your pain as fast as possible. We have the best tools, techniques and machines to make sure you get the best value for your money. Our Physios will test a lot of different possibilities why you’re feeling this pain in order to explain what’s going on in your shoulder. It all depends on the results of our tests to determine what needs to be done. All our physios are specialists that can determine the slightest problem coming from your shoulder, neck or upper arm, so if you’re uncertain – we can help you.
Our experts determine the priority which problems to fix first. Shoulder injuries are our expertise & what we’re best at. We’ll guide you every step of the way.
Patients that don’t opt for treatment can develop the following:
- Abnormal Scar tissue formation which causes abnormal shoulder movement patterns leading to a cascade of compensatory mechanisms.
- Shoulder joint stiffness due to immobility and causes abnormal joint movement, stressing adjacent joints even more.
- Muscle weakness which leads to other muscles working harder to perform that muscle’s function and constant spasms in your neck & shoulder.
- Shoulder joint laxity that can lead to unstable joints, clicking & grinding, that can even accelerate degeneration in your shoulder.
Shoulder Injury Treatment
You know when an injury occurs. There may be pain, swelling, bruising or even bleeding. The first and best thing to do is to apply the 5 step PRICE regime. It reduces your pain and swelling, and even minimizes the damage of the immediate injury. It also prepares the body for the next stage of treatment, not to mention the benefit of healing faster.
Protect
Protect the injured joint, muscle, nerve or tendon from getting worse by using strapping or a brace. Shoulder slings can also be used to prevent movement and provide support in an effort to minimize the tissue damage. We use it to ‘immobilize’ your shoulder, by restricting its movements and prevent you from using it.
Rest
Forcing yourself to go on when there are signs of an injury is not only damaging to the tissue but also unwise. “No pain, no gain” does not apply here. It prevents healing from taking place. Rest is important to allow the muscle, tendon or ligament to reattach and heal. Avoid any activity or movement that produces or brings on the pain for the first 3 days. After that, you need to start moving or other problems will develop.
Ice
Cold provides short-term pain relief by limiting the bleeding around the tissue injury. The bleeding from ruptured arteries and veins causes an increase of pressure surrounding the injured tissue which will also decrease the blood flow, and in turn nutrition and restrict removal of metabolic waste products. The first priority is to stop the bleeding as fast as possible. Wrap an ice pack or ice cubes in a towel, wet the towel and place on the skin. Apply the ice for 15 minutes on, 20 minutes off. Repeat 5 times per day for the first 3 days.
You will feel a redness and ‘warm’ feeling after the ice as been applied. This is when the body reacts by sending cells to clean up the injured tissue and start repair. Warning: Never apply heat (and heat rubs) to an acute injury in the first 48 hours. The heat encourages bleeding and could be detrimental if used too early.
Compression
Using a Compression bandage, elastic strapping, neoprene sleeve or brace reduces the bleeding and swelling which occurs when cells and other substances rush to the site of a shoulder injury. Applying compression also helps to prevent the blood from pooling in your tissue and reduces your shoulder pain. Take care not to have the bandage too tight, as it will restrict blood flow.
Elevation
Resting with the injured shoulder above the level of the heart is the best. In order to effectively use gravity, your shoulder must be above your heart to assist in the drainage. For example lie on your side propped up with some cushions with the painful shoulder on top.
When is surgery necessary?
After a consultation we assess the need and possibility of surgical intervention. Each conditions has a spectrum, and we’ll determine if you meet the criteria if surgical treatment is an option. We will refer you to a specialist if necessary. Before we opt for surgery, we want to give you the best chance of recovery, because once the surgeon intervenes – there’s no turning back.
The type of surgery and extent of shoulder damage determines your recovery time. Our extensive experience in rehabilitating shoulder injuries after surgery means we can work to get you pain free in the shortest and safest possible time.
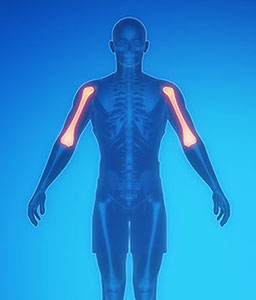
Shoulder Muscle Pain
Muscle strains are often called ‘muscle pulls’ or ‘pulled muscles’. These terms refer to the way these injuries occur – the muscle tissue is forcibly stretched until it is torn. Depending on the number of torn muscle fibers, muscle strains are classified as first degree (least severe), second degree (moderate severity) and third degree (most severe) strains. Strains are common and the first line of defense that usually fails.
Your shoulder is made up of joints, muscles and tendons. The joint looks like a lollipop with the ‘ball’ placed in a socket. This joint very mobile because it needs a wide range of movement. It need to give you enough freedom to move while also providing stability. Your joint also has a labrum (ring of cartilage) around the shoulder socket to help with smooth movements, and other shoulder joints connect the collar bone to your shoulder blade.
Because the shoulder joints have a wide range of movement, they need to be stabilized by muscles to prevent the join. The main muscles providing this function is the rotator cuff. They work in unison to keep the joint in its socket. In patients with chronic shoulder pain these muscles are injured, damaged or unbalanced (in a way rate that they fire) and as a result increases your pain.
How to Stop chronic, daily annoying shoulder pain
Without injections, Without taking painkillers and
WITHOUT having to wear a Support or Brace…
If you’re living with shoulder pain what just won’t go away, they’re painful or they ache – it’s very easy to think that it’s “just something that comes with age”, it’s a bit of “wear and tear”, or that it’s nothing and it’ll go away on its own.
You can’t quite point your finger on why you’re feeling the pain in your shoulder – but it doesn’t seem to be getting any better!
If that’s happening to you, you’re not alone – we hear this type of thing all the time. In fact, shoulder pain is one of the most common problems that we see in our Physio practice. When it comes to living with shoulder pain, everybody we see wants to know the answers to these questions:
Why am I still suffering with shoulder pain that keeps getting worse
Most people think that when they get shoulder pain, it’ll eventually “ease off” and go away on it’s own. That they’ll wake up one morning and like “magic”, your shoulder pain will be a thing of the past… But 3 months later you’re still living with the annoying shoulder pain, often even worse than it was at the start. Does that sound like you?
Another scenario we see all the time in our physiotherapy practice is when people go to their Doctors, and the well-meaning Doctor tells them to “rest”, “try these painkillers” and “come back in 6 weeks if it’s no better” – but then 6 weeks later, they end up going back to the same Doctor again because it hasn’t got any better, only to be given ANOTHER prescription of even stronger pills, and maybe a shoulder sling.
Has this ever happened to you?
Maybe you’re confused because you’ve been told different things, by different people. Maybe you think you have to rest because you’ve been told walking makes shoulder pain worse, or that you should be doing ‘this exercise’ and ‘that exercise’ to make it better. It’s very confusing to know exactly what to do – and that’s just to avoid making your shoulder pain worse, not to mention getting back to driving and all the other things you love to do.
And because of this confusion – this often leads people to procrastinate, and put off making a decision about what to do to help fix their shoulder pain. Worse, many people just end up accepting it as “part of life” – as if it’s normal, as if it “has” to be that way. Is this how you feel?
We are here to tell you – this is NOT what you deserve. You are made for great things, your shoulder pain is just a bump in the road. Make a decision to help yourself be better.
Why is your shoulder pain lasting longer than it should?
Does this sound like you?
If any of these have happened to you – we would love to help you. The fact that you’ve tried any or all of these things already is actually a good thing, because when you know what doesn’t work – you are closer to finding the thing that does!
We invite you to come and see us. Why? Because we do things differently. We’ll do a thorough assessment and test all the possible causes. After we’ve diagnosed your problem, and explained what it’s going to need to heal, we’ll make sure you understand why this is happening.
If you’re looking for solid advice on how to start solving your problem, click the link below to book a FREE phone call. The phone call is complimentary and there is no obligation to book any appointments with us after the call is over. This is an opportunity to get an expert’s advice about your situation. Our goal is to help you make the right decision about what to do next.
What you can do to get rid of your shoulder pain quickly?
Ask our shoulder experts
If you would like to know how the team at Well Health Pro can help you, we invite you to book a FREE, no-obligation, risk-free “Call me back” phone call.
Note: This Free Call is a service we offer to people who are nervous or unsure. You might not know if Physiotherapy is the right treatment for you. If you are unsure, please fill out our online form. We will contact you to find out what is wrong and how we can help. There is no financial obligation or risk on your part. You have nothing to lose except your pain.
Choose to see a Well Health Pro Physiotherapist to help you Get rid of your shoulder pain – in the next few days?
What your patients say:
I received very professional service from everyone involved and can definitely recommend this practice to anyone struggling with shoulder pain.
L Erasmus
Highly professional and very knowledgeable when it comes to shoulder injuries. He takes his time with his patients and always ensures he is providing the best possible care. Highly recommended treatment. Thank you for assisting me with my shoulder pain!
M Laas
“The best in the business”
She’s amazing, friendly and so thorough. She helped me with my shoulder pain. After only two sessions my shoulder was basically back to normal!
D du Toit