If your first few steps out of bed in the morning feel like walking on shards of glass, you are not alone. Millions of people experience foot and heel pain in their lifetime, with plantar fasciitis as the biggest culprit. Despite how debilitating that sharp, stabbing pain can be, it is important to remember that the plantar fascia is incredibly resilient. It isn’t broken; it is simply overloaded (most often by sudden changes in your routine). The good news is that while this condition can be stubborn, it responds really well to the right treatment.
Most people worry that their heel pain signifies permanent damage, torn tissue, or the need for invasive surgery, but the reality is quite different. A structured approach that balances relieving your symptoms, rest, and progressive exercise is the best way forward.
The remarkable engineering of the foot
Your foot is designed to be both a flexible shock absorber when your heel hits the ground and a rigid lever when you push off to take a step. This dual role is supported by the arch of the foot, which is a complex, bridge-like structure at the bottom of your foot.
Bones and Joints
The foot is made up of 26 bones and 33 joints. The arch is primarily formed by the tarsal bones (the midfoot) and the metatarsals (the long bones leading to your toes). They naturally fit together to distribute your body weight. Numerous ligaments connect bone to bone, acting as the glue that keeps the joints of the arch from shifting too far apart.
The Plantar Fascia
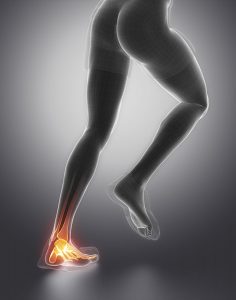
This is a thick, multi-layered band of connective tissue that runs from your calcaneus (heel bone) to the base of your toes. Think of it as a high-tension cable that prevents the bone arch from collapsing under your weight.
Muscles and tendons
-
Intrinsic Muscles: These are small muscles located entirely within the foot and toes. They act like the “core” of your foot, providing fine-tuned stability with every step.
-
Extrinsic Muscles and Tendons: These are larger muscles that start in your lower leg (like the tibialis posterior, flexor hallucis longus, flexor digitorum longus, and the peroneals) and send long tendons down into the foot. These tendons act like stirrups, pulling the arch upward and providing the power needed for gripping your toes, walking, and running.
Together, these muscle groups dynamically adjust and support your foot arch as you move.
The perfect combination of structure and movement: The Windlass Mechanism
As your big toe bends upward during a step, it pulls the plantar fascia tight, which automatically lifts the arch and locks the bones into a rigid, powerful position for push-off.
What changes with Plantar Fasciitis?
The term “fasciitis” implies inflammation of the fascia. But it is more of a loading issue where the fascia struggles to keep up with the demands placed upon it. The harmony between your passive (bones, ligaments, and fascia) and active (muscles and tendons) support structures is disrupted.
-
Plantar Fascia: Instead of being an elastic support structure, it loses its ability to stretch and recoil.
-
Muscles: The intrinsic foot muscles and the calf muscles overwork to try to guard the foot and arch.
-
The Windlass Mechanism: The coordinated tightening of the arch when you push your heel away becomes painful. As a result, your body subconsciously changes how you walk to avoid tensioning the fascia.
Ultimately, your ability to walk changes in many ways. Suddenly, you feel like you’ve lost the spring in your step, and you can’t stand or walk for too long. Walking feels heavy and tiring, and you can’t stretch or put weight on your foot like you used to.
I think I have Plantar Fasciitis. How did it happen?
While the name, Plantar Fasciitis, implies that the fascia is inflamed, the actual pathology of plantar fasciitis is a complex journey from early irritation to structural change.
The initial microtrauma
It all starts when the movement and weight (load) on your foot exceeds what your plantar fascia is used to handle. Usually, this is triggered by changes in your day-to-day routine. Like walking or running further than you used to. Or wearing different, less supportive shoes. Being less active can even change and decondition your foot’s ability to carry the usual weight. These changes ultimately put stress on the fascia in the foot and cause microscopic “fraying” or micro-tears in the collagen fibers, usually at the point where the fascia anchors into your heel bone (the calcaneus).
Inflammation builds up
Your body responds to the microtrauma with a classic acute inflammatory response. Specialized cells rush to the site to start the clean-up and healing process. The tissue becomes swollen and warm due to a change in cellular activity, and chemical inflammatory markers sensitize local nerves, making the tissue extremely sensitive. This is when you feel the sharpest pain (especially in the mornings) and notice that the area is sensitive even to light pressure.
The repair cycle fails
If the repetitive stress on the fascia continues without enough rest, your body enters a state of “failed healing.” Because the fascia has a relatively poor blood supply compared to muscles, it heals more slowly. Instead of producing strong, organized collagen in the fascia, it lays down disorganized tissue. Now, the tissue is thickened, scarred, and less elastic. Instead of just experiencing an inflammatory flare-up, you end up with structural changes and eventual tissue degeneration (weakening).
Compensation of the foot and bone
As the fascia loses its elasticity, it affects the movement of the surrounding joints. Your toes and ankle won’t be able to move and stretch the way they used to, because it is like they are pulling on a very tight spring. Over time, the constant pulling (traction) on the heel bone triggers your body to grow extra bone in the direction of the pull. This is how heel spurs develop. While the spur itself isn’t usually the cause of the pain, it is a visible sign that the fascia has been under high tension for a long time.
Functional breakdown
Finally, the Windlass Mechanism becomes compromised. Because the fascia tissue is thickened and less elastic, it cannot efficiently maintain the arch and support of your foot. This leads to muscle fatigue in your calf and foot muscles, as they try to support and move your foot at the same time. If your muscles can’t keep up, you end up not being able to walk as far as you want to. You compensate by walking with a rigid foot, but that causes your opposite leg and foot to hurt. By doing less and less, it keeps the painful cycle in motion.
Causes of Plantar Fasciitis
Mechanical and Lifestyle Factors:
- Sudden increases in activity: A rapid increase in time on your feet, like running further, walking more, climbing more stairs, or hiking uphill.
- Prolonged standing: Spending more time standing in queues or occupations that require standing for many hours (e.g., nurses, teachers, factory workers)
- Different or inappropriate footwear: Flat shoes with minimal arch support, worn-out trainers, or new shoes with a hard sole are all culprits that force the fascia to work harder.
- Surface changes: Your foot has to work harder on different surfaces, especially if it isn’t used to it. Think of walking on loose sand or cobblestones, or going from road running to trail running or strenuous hiking.
Predisposing factors:
- Foot arch biomechanics: Having naturally flat feet or high, rigid arches causes the fascia to overstretch and lack the ability to absorb shock.
- Calf and ankle stiffness: Decreased flexibility in the calf muscles and ankle joint forces the fascia to excessively pull on the heel. Previous injuries to your Achilles, ankle, and calf play a role here.
- Walking pattern: Subconsciously changing your gait due to a knee, hip, or even lower back problem alters the way your weight is transferred through your leg and foot.
- Age: Plantar fasciitis is more common between the ages of 40 and 60 (and up), a period when the natural elasticity and recovery of connective tissue declines.
- BMI (Body mass index): Increased body weight directly affects the load that your foot has to carry with every step you take.
- Systemic conditions: Underlying health factors, such as diabetes or rheumatoid arthritis, affect your circulation, inflammation levels, and impair your body’s ability to heal.
Diagnosis
Physiotherapists are trained to examine the structures of the foot, including the bone, ligaments and tendons. We will be able to guide you if further investigations are necessary. X-rays enable us to see the bony structures of the foot, and a heel spur can be diagnosed this way. The plantar fascia is soft tissue and can be visualized with an ultrasound (sonar). The ultrasound will show thickening and damage to the the structures.
Risks and complications
If left untreated plantar fasciitis will usually worsen. You may experience severe pain when placing weight on your foot. This can then lead to limping, in an attempt to reduce the weight you take on the foot. Limping can then influence your ankle, knee, hip and eventually your back too.
Recovery time
Plantar fasciitis should heal within 3 months with treatment. If you have surgery, you should wait three to six months before returning to sport.
If you think you may have Plantar Fasciitis you should:
- Stop aggravating activities (walking/standing/jogging)
- Use ice and rest to reduce the inflammation
- Call us to set up an appointment to confirm the diagnosis and guide you through a rehabilitation program
Physiotherapy treatment for Plantar Fasciitis
Early stage
- Electrotherapy to reduce local inflammation (ultrasound/LASER/TENS)
- Soft tissue mobilisation to relieve your symptoms (myofascial release/dry needling)
- Immobilization with strapping or taping
- Night splints can be warn to reduce morning stiffness
- Orthotics (insoles) may be necessary
- Specific exercises and ice application at home
You may begin:
- Deep water pool running to maintain your cardiovascular fitness
If your Plantar Fasciitis fails to respond to physiotherapy treatment
Your GP can prescribe medications to alleviate your pain and reduce inflammation.
We may refer you to a specialist for injection directly into the tendon.
If your plantar fasciitis symptoms persist for 12 months, as a last resort, we will recommend surgery to relieve tension and information from the plantar fascia.
How severe is my….?
Choose 4/6 of the below signs and DISCUSS why you (as a professional) use to identify and classify the … into: Severe vs Not severe
EXPLAIN WHY it is a serious type of injury ~ This describes the scope of … to a patient in order to understand if it’s worse or better than another person with …
Meaning: Imagine there’s a group of 20 patients, all with … and you must rank them from ‘less severe’ to ‘more severe’ ~ What markers/ signs will you look for to make your hierarchy and group them?
- Frequency – Intermittent/Constant/recurring
- Movement or static positions (rest) flare pain.
- Duration – Days, Weeks, Sudden, Short burst, change position of your … eases the pain.
- Size – Radiate – Shoulder, Upper back, Head…
- Intensity (pain) – bearable, pain doesn’t stop you, hesitant to
- Colour: Bruising, Blue, Red,
- Loading: Contraction, Low load required to bring on pain, High load (jump)
- ROM: Limitation? Less than 10 degrees limitation (not a problem) vs completely locked up.
- Stiffness
- Swelling
- Intensity: Discomfort – Painful – Sharp sting
On a scale from 0-10 describe a picture of Regression.
- Ligament tear Gr 1 – 3
- Muscle strain, micro tear – complete separation split in fibers
- Tendon phase of degeneration
- Cartilage erosion, plugging, tears
Diagnosis
Physiotherapy diagnosis
Describe a sentence to give the patient confidence that we’re the equipped/best at diagnosing this problem.
“We can handle it” vs “Our knowledgable expert physiotherapists are well versed, confident, and experienced in their approach to diagnosing your…”
We follow a structured plan to diagnose, classify the severity, and determine the hierarchy of priority that your knee needs. We stress, screen and scan all the possibilities that could be causing your pain. Identify any other injuries to surrounding structures. If there is an injury to the ligaments, meniscus, muscles or nerve, or cartilage we will find it.
We understand the physiological healing stages you’ll go through, and custom-fit your treatment program. By knowing the extent of the tissue damage we can guide you through a structured program to recover faster and safely return to the things you love doing. That’s why our physiotherapists are the best at diagnosing this type of problem.
Why is it crucial to get/understand a diagnosis? Does it mean anything? Or is it a death sentence? or will you treat it differently if you know what you’re dealing with?
X-rays
Muscles cannot be seen on an x-ray, so it will not be effective to diagnose a muscle spasm. X-rays will however show the integrity and alignment of joints in your spine. This will enable us to see if something is wrong with the structure of the bones in your spine or if there is a loss of disc space.
What are you looking for on an X-ray? Cortical stress lines, Displacement measurements, What Classification is done via X-ray?
Your physiotherapist can refer you to get x-rays taken if necessary.
Diagnostic ultrasound
Diagnostic ultrasound can be used to show the presence of a muscle tear (muscle strains), inflammation, swelling or simply increased contraction of a muscle (muscle spasms).
If you need an ultrasound, your physio will refer you.
MRI
An MRI scan can image all of the structures in your lower back, including soft tissue, discs, nerves and bones. However, for a muscle spasm an image like this is unnecessary and very expensive. If your physiotherapist suspects anything more than just a muscle spasm, you will be referred to the right specialist.
Is an MRI necessary for this diagnosis – if not when could it become a necessity?
Why is the pain not going away?
Why will this condition NOT resolve or recover on it’s own
Discuss 3 Problems that are OUT of the patient’s control but can, with guidance, be leveraged to accelerate and control healing or limit setbacks or regression.
A prompt to ask Gemini: Search medical journals published to Rank the risks of complications and secondary fallout caused by with a… treated using non-surgical rehabilitation not limited to, but including predictable compensation patterns, joint stiffness, specific muscle weakness, physiological complications due to anatomical structure, swelling, non-union, malunion, rupture, tendonitis, arthritis, accelerated joint erosion. Also, indicate the percentage likelihood of the development of these complications.
Expected compensation, adaptation
- This section assumes that NO intervention/ treatment/ personal care/medical attention is applied….
- A patient who leaves his … untreated, undiagnosed, what will happen next…
- Pathology:
- If you don’t take the warning signs seriously, you risk more critical and possibly irreversible damage.
- Discuss physiology that slows down your recovery (severed nerves, swelling impede arterial bloodflow & nutrients, venous clearing of debris
- Discuss – Non-union, Malunion, Prolonged healing, Abnormal Callus formation, etc.
- You become stuck in a cycle of pain, not knowing if it is safe to move or not.
- Without intervention or treatment, why is the tissue state not improving?
Problems we see when patients come to us with …
Discuss 3 Problems that are WITHIN the patient’s control with guidance, which can be leveraged to accelerate and control healing or limit setbacks or regression.
Complications (guaranteed, or high probability of developing with this problem/diagnosis/condition.
- One concept per paragraph. Explain what resistance or problems you can encounter during the treatment process. Stay to the core message.
- These are not bullet points —they are only to guide your thoughts. Choose a few (not all) and explain why.
- Themes range from: Ignoring… , Accurate Diagnosis, Immobilisation, Too much rest, Too little rest, Medication use,
- Speak to your patient as if each of these is happening to them.
- Without treatment, a “wait and see” approach. – What’s wrong with it, and what problems will they face?
- Explain why it’s a problem. Not only state “it’s a problem” but explain why.
- Reasons that delay recovery time
Pain medication (how long is normal/ acceptable)
Misconceptions about treatment
Physiotherapy treatment
Please inspire confidence in your ability to test, identify, diagnose and treat/ deal with this.
Example:
Our priority is to determine the extent of the damage to your piriformis muscle. Then, we test the structures surrounding your hip and lower back to clear the nerve pathway and resolve the sciatic nerve pain. Avoiding nerve compression is crucial to prevent relapse and restore the sciatic nerve’s regular sliding. We must protect the muscle from overworking by differing forces away from the piriformis muscle, strengthen the surrounding muscles, correct the compensation, and retrain the correct firing pattern. This allows time for the piriformis muscle to adapt and heal. Our practitioners bring on a change and monitor the results until it’s working, and then we magnify the effects to get even better outcomes.
Patient asks you:
“So why should I come see you for … ?”
Your answer is…
- We can provide the best treatment for, provide guidance and answers., Implement a very effective and structured plan of action like
- Use the antonyms of the words the patient complains of. Instibility – stability/stable, Fear – confidence, worried – calm/carefree, anxiety – serenity
- And we will also look at (muscle strength, joint range of motion, flexibility, ligament stability, and nerve control.)
- Gradual strengthening, control, and conditioning.
Phases of rehabilitation
Keep your focus on the primary problem structure.
As long as I can see progression & functional expectations changing, Example:
- crutches
- 20% Weight (limited ROM)
- 50% weight (FROM)
- 100% weight with concentric & eccentric contractions
- Speed & Power (Jump)
Please work the PEACE & LOVE protocol into the Plan of Action (Not all in the first phase)
- Balance on one leg
- Perform a lunge
- Squat to 90 degrees
- Balance reactions (stepping out sideways, forwards & backwards)
- Jump & Land from a step
- Do a Single leg jump
- Sit in a crouched position & get up
- Jump over a hurdle
1st Phase: What you want to achieve (Week 0 – 1)
Functional expectation, what we’ll do.
E.g. “Our first aim is to get the proper diagnosis and identify and prioritize any contributing factors to your unique problem. Now, we can guide you in avoiding any aggravating activities for the time being and managing your symptoms. This includes a list of things that are safe to do and some that are not. ”
To progress to the next stage you should be able to …
2nd Phase: What you want to achieve in Week 1 – 2
What needs to happen in the tissue/ pathology to fix it
This is the thing you should be able to do by now
3rd Phase: What you want to achieve in Week 2 -3
Treatment elaborated
This is what you need to be able to do with ease so we can progress to the next phase of treatment.
4th Phase: What you want to achieve in Week 3 – 4
Re-inforce, strengthen, guide,
What you should be able to do by this stage is ….
5th Phase: Test return to normal life Week 4 – 6
To makes sure you’re safe to turn to
- Driving you should be able to
- Jogging you should be able to
- Run you should be able to
- Work
6th Phase: Final medical clearance tests (Week
By now, you should be able to jump and throw, but there are some specific stress tests you should be able to do.
By now, you should be able to return to your routine. During the final week of your …….. treatment, we want you to be able to train at your full capacity. ………….. should be able to handle stretch stress, max load, and compressive forces.
So we can sign off on your recovery, knowing you’re safe.
Healing time
Physio protocol time frame for healing (weeks/months)
- A full recovery and return to sport will take longer and should not be confused with the healing period.
- It takes about 3 to 4 months to return to exercise and sports.
- You will need physiotherapy treatment twice a week for the first two weeks.
- After this, your treatment sessions can be …
- Remember: “Non-operative Treatment” or Non- Surgical Not
conservative
Other forms of treatment
This section is about other treatments that can help the process services that can help – but we don’t provide.
- Your doctor (GP) will probably
- Pain meds, injections,
- Getting your back or neck ‘aligned’ or ‘clicked’ in the hopes of improving the … will not improve the state of the muscle or change your pain. It could even worsen or trigger a muscle spasm. You need to look at the bigger picture.
- A biokineticist will be able to help you in the final stages of your rehabilitation and get you back to training for your sport.
- Wearing a back brace won’t be the solution to your problem.
- Stretching or foam-rolling might ease your pain temporarily, but
Is surgery an option?
Surgery is necessary when …
- These surgical checkboxes must be ticked before surgery is even considered.
- What is considered a failure of conservative treatment when surgery must be considered?
- Give the components of clinical measurements that indicate surgery
- Surgery is only the Halfway mark for a successful surgery; the rest is reintegration, strengthening, and adapting your body to the change.
- Why is rehab important after surgery?
What else could it be?
- Only mention a few (up to 5) differential Diagnosis
- Describe one symptom or difference between the two that sets them apart
- This section is for very similar Conditions but one or 2 differentiating factors.
Also known as
- Synonyms
- List key phrases (careful – start each bullet with different word)

