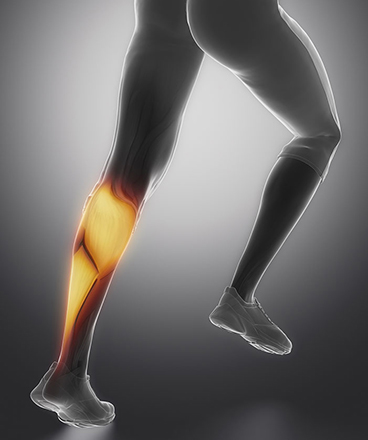
Achilles tendonitis is a common overuse injury that causes Achilles tendon pain. Your Achilles tendon is the anchor that attaches your calf muscles to your heel bone. This makes it possible for you to move your foot and to do the most basic daily activities like walking. Even though Achilles tendonitis is a common injury among people who practice sport, it can just as easily happen to people who do not take part in sports. The biggest cause is excessive overuse or overburdening of the Achilles tendon, which leads to heel pain that feels worse when you walk, run uphill or climb stairs.
Achilles tendonitis is also called Achilles tendinitis or Achilles tendinopathy, with no difference in meaning. Achilles tendonitis treatment involves that you change the load and amount of work that you require your Achilles tendon to do. This article explains exactly how to do that and how Cilliers & Swart Physiotherapy can help you.

Anatomy of the Achilles Tendon
A tendon is a band of tough connective tissue connecting a muscle to a bone. Tendons can be compared to ligaments. Both are made of collagen, but ligaments connect bones to each other and tendons connect muscle to bone. Tendons are able to withstand a great amount of tension and need a lot less blood supply and oxygen than muscles. This allows tendons to not get tired as quickly as muscles do, because they need to carry loads and maintain tension for long periods of time. The Achilles tendon is the biggest and strongest tendon in the human body and it anchors your calf muscles to your heel bone (calcaneus).
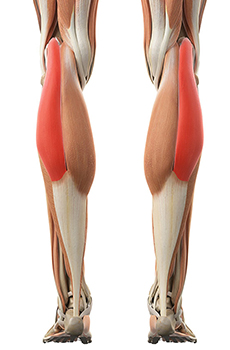
Your calf is mainly made up of two big muscles (the gastrocnemius and soleus muscles), which join at your heel. Your Achilles tendon stems from these calf muscles and anchors them to your calcaneus. It is surrounded by a sheath (synovium) that allows it to move freely between the different layers of tissue surrounding your heel. There is a bursa (called the retrocalcaneal bursa) that lies between your Achilles tendon and your calcaneus. A bursa is like a small fluid-filled sac and can be found on different joints in your body. The retrocalcaneal (meaning at the back of the calcaneus) bursa helps to decrease friction between the Achilles tendon and calcaneus.
Your Achilles tendon takes a huge amount of load when you step and put your own body’s weight on your foot. It is also able to withstand the tension of your calf muscles pulling on your calcaneus when you are standing or walking.
Fun Fact
The Achilles tendon is named after the great Greek hero, Achilles, who was dipped in the river Styx by his mother, Thetis, for protection. He thus became invincible, except for the area around his heel, where his mother held him. This weak spot later caused his death when he was shot by an arrow trough his heel. He couldn’t move after that and fought to his death. This gives meaning to the proverbial ‘Achilles heel’, meaning that it is your weak spot.
What does the Achilles tendon do?
The Achilles tendon connects and anchors your calf muscles to your heel bone. When your calf muscles contract (shortens), they pull on the Achilles tendon. Your Achilles tendon then pulls on your heel bone (calcaneus) to make your toes point – like a ballet dancer. This muscle-tendon-heel-bone-pulling happens when you raise your heels off the ground when you stand on your toes. The opposite action, for example pulling your toes towards your shin, will stretch (lengthen) your calf muscles because the heel bone (calcaneus) is pulling on the Achilles tendon in the opposite direction.
Your Achilles tendon is essential for all ankle movements. It is specifically active in pushing off movements or controlling your landing onto surfaces. Examples of pushing off movements include the push off phase when you are walking or running, pushing your heel off the ground when you’re standing on your toes or jumping, and pushing your foot off of a surface like the start before a sprint. Opposite examples include your Achilles tendon absorbing the force of landing from a jump or exercising control when walking down an incline.
Without your Achilles tendon, you won’t be able to do some of the most basic ankle movements, never mind walk or run. Your foot will feel like it is flopping about when you try to walk.
How does Achilles tendonitis happen?
Healthy tendons are brilliant white in color and have a fibro-elastic structure that consists mostly out of collagen fibers. However, the blood supply and oxygen consumption of tendons and ligaments is 7.5 times lower than that of muscles. The fact that tendons have poor blood supply, means that tendons heal a lot slower after an injury.
The structure of a tendon will change if repetitive strain is put on it. Either through compression or tension. The network of collagen fibers in a tendon gets disrupted by micro-trauma caused by too much strain. It leads to hypercellular activity in the tendon, which is an excess production of collagen cells. So, in an attempt to heal, your body produces more new collagen cells. However, this leads to the tendon thickening and becoming less flexible and ultimately the collagen structure weakening.
Your Achilles tendon must be able to withstand the tension of your calf muscles pulling on it, while also withstanding the compression force of pushing off with your heel. The tendon is elastic, meaning it can stretch and recoil. However, straining the Achilles tendon during physical exercise and overburdening the tendon above it’s physiological limit can cause micro-trauma. Continuous micro-trauma and thickening of the tendon causes increased friction between the fibers. Changes in the tendon changes the ability and strength of the tendon to handle the load put on it. Ultimately it could lead to degeneration of the tendon.
To illustrate using an example: Imagine a bungee cord with no elasticity. When the person at the end of the rope falls, the lack of elasticity means the rope won’t recoil. This means that the cord might snap, because of the sudden jerk (force) without the ability to absorb the shock. The same principle applies with your Achilles tendon. If a sudden force is placed on the tendon, when it is unable to absorb shock or recoil, it gets injured, “frizzles out” or worst case scenario it snaps (Achilles tendon tear/rupture).
Note: Achilles tendon tears are explained in a different article.
The root of the problem
Achilles Tendonitis describes the injuring and subsequent overburdening and wearing out of your Achilles tendon. Wearing out this tendon involves repetitive pulling on the tendon (referred to as ‘overuse’ e.g. jumping into the air) or putting the tendon under excessive force (referred to as ‘overload’ e.g. landing on hard surface from a jump). Other factors like your body weight, biomechanics and metabolic health might make you more prone to get an injury like this.
The term tendonitis, tendinitis and tendinopathy all mean basically the same. The meaning of these terms all boil down to pain, inflammation and pathology of a tendon. Thus, Achilles tendonitis can be described as a generic term used to describe pain and pathology associated with overuse in and around your Achilles tendon. The pain is typically worse with or after movement.
There are different stages of Achilles tendonitis. The condition of the tendon is especially susceptible to change in the early stages of tendonitis. Later on degeneration sets in, and it comes to a point where the tendon cannot change back to a healthy tendon. In the early phase of Achilles tendonitis there might be some inflammation present, but it is mostly the sheath around the tendon that becomes swollen and inflamed. In later stages of tendonitis or chronic tendonitis, very little inflammation will be present in the tendon, if any. The main problem can be traced back to the weak or disrupted tendon fibers.
Interestingly enough it has been shown that not using a tendon enough is just as bad as overburdening it. The same kind of changes happens in an ‘unburdened’ tendon that changes the mechanical integrity of the tendon.
There are two distinct and different areas where Achilles tendinopathy can develop:
Insertional Achilles tendinopathy:
Pain located at the base of your heel, where the Achilles tendon anchors its fibers directly onto the calcaneus.
Mid-portion Achilles tendinopathy:
Anywhere along the Achilles tendon, but more than 4 centimeters above the heel and before the tendon and calf muscles connect. Pain in this area can be experienced on any side of the tendon e.g. inside border, outside border or middle/belly.
Causes of Achilles tendonitis
The biggest cause of Achilles tendonitis is overburdening or overloading of the tendon. However, there are a few other things that can make you more prone to get Achilles tendonitis. Each person is different, so looking at the bigger picture and every different contributing factor is the best way to determine what is the main cause of your Achilles pain. External (extrinsic) factors and internal (intrinsic) factors contribute to causing your Achilles tendonitis. You can develop acute Achilles pain quite suddenly, or struggle with it chronically.
Extrinsic causes:
- A sudden increase in force – pushing yourself off the ground during high jump
- Running further and faster – sprinting the last 100 m of a 10 km race
- A change in your activity – starting to train for a marathon when you haven’t really jogged in a while
- Changes to the surface on which you exercise – jumping and landing on hardwood floors vs. concrete floors
- The shoes you wear when walking or running – Shoes that are worn out or not giving enough support vs new shoes that you aren’t used to
- Pushing through your pain continuously – Continuing to train even though you’ve injured yourself
Intrinsic causes:
- Alignment of the foot and ankle – Increased pronation of the foot can be associated with Achilles tendinopathy
- Calf muscle strength – Calf muscles of one leg stronger than the other
- Flexibility – Lack of flexibility of your calf muscles puts more strain on the Achilles tendon
- Body weight and biomechanics – This influences how much of the load your Achilles tendon takes
- Age and gender – Flexibility tends to decrease with old age
- Hormones – Certain levels of hormones can influence the flexibility of ligaments and tendons
- Diabetes – Diabetes can lead to circulation problems and slow healing of tissues
- Poor circulation – Certain health conditions cause poor blood circulation in your body and can slow down healing of tissues
- Use of certain medications – It has been shown that certain medications (like certain antibiotics) can weaken the structure of tendons
Acute tendon pain
When an acute injury occurs, you will immediately know it. In that moment the force will be too much for your Achilles to handle and there will be an immediate, sharp/shooting pain at the back of your heel. It will be debilitating and you’ll not be able to continue with your activity. For example when you attempt to sprint, without a proper warming up.
Note: Achilles tendon ruptures are different from tendonitis.
Chronic Achilles tendonitis
Chronic tendonitis can develop slowly over time. Especially if you have had repeated injuries without getting treatment. Initially the pain feels dull and stiff, but then it lingers and just never seems to “go away”, even with basic activities like taking that first few steps in the morning or climbing stairs.
Acute Achilles tendon pain on top of chronic Achilles tendonitis
Maybe you have struggled with a dull ache in your heel for a long time. Now it gets worse with sudden foot movements and the pain spikes every time you need to quickly get up. This is an acute on chronic condition where you get a flare-up of your “old” symptoms.
Symptoms of Achilles tendonitis
It is important to note that you can be in any phase of tendinopathy and not always be in pain. Pain comes when you change the amount of work that the Achilles tendon is supposed to do.
How bad is my Achilles tendonitis?
Tendonitis can be classified into three different stages. It starts with acute Achilles tendon pain and if the right steps are not taken to get the tendon back to a healthy state, it progresses. The structure of the tendon weakens over time and can start degenerating and disintegrating. Ultimately leading to an Achilles tendon rupture.
1. Reactive tendonitis (First stage)
The acute phase of Achilles tendonitis (reactive tendonitis) is caused by a change in the amount of work that your Achilles tendon needs to do. Straining, overload and overburdening the Achilles tendon is the biggest deciding factor. Usually, in this phase there will be some inflammation and possibly swelling around the tendon or tendon sheath (synovium).
Let’s say you felt your Achilles ‘pulling’ during a run uphill, but it seems to go away after a while. Now you continue running every day for the rest of the week. At the start of each run you feel pain in your heel, but it improves when you run. It can’t be that bad then, can it? When you push through this pain every time, you are repeatedly causing micro-trauma to your Achilles tendon. If you do not get the right treatment during this phase, the structure of your Achilles tendon starts to change and it gets weaker. At this stage the tendon has the potential to recover and revert back to its normal structure.
2. Tendon dysrepair (Second stage)
Reactive tendonitis (first stage) can progress to tendon dysrepair (second stage) if the tendon is not allowed to recover. During this phase there is continuous breakdown and disorganisation of the collagen network as your body continues to try and heal the tendon. This means that the collagen fibers are not neatly arranged in bundles, but they tear away from each other, like a cable or rope where the individual strands break and seperate. Applying more force will cause more damage.
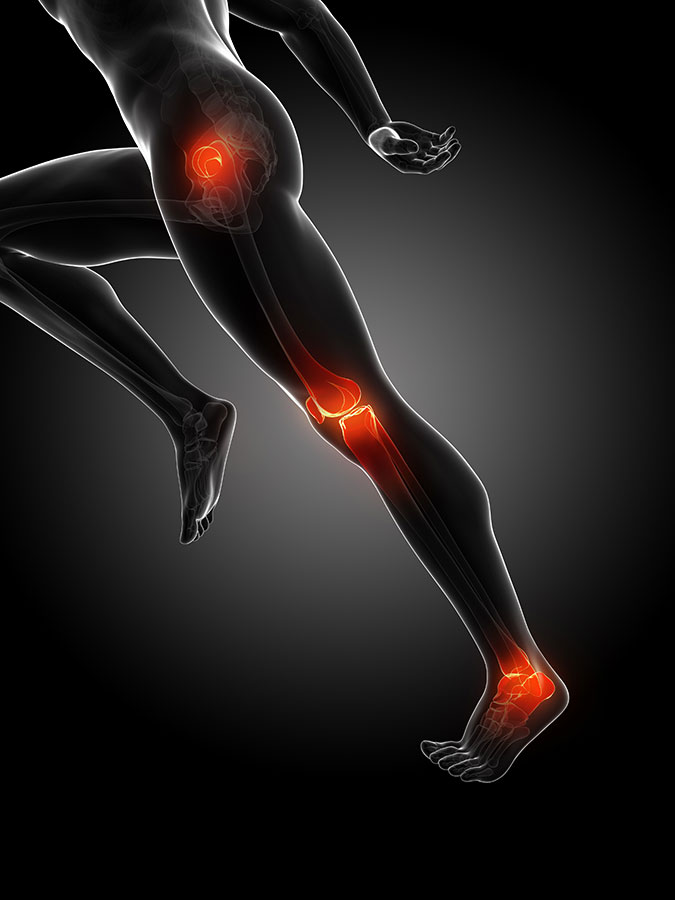
In this phase, you will feel a dull pain in your heel at the start of your run, but it will linger a little bit longer, and bother you more and more. Now you start to feel the pain not just during your run, but also throughout the day with simple activities like walking or climbing stairs. As the tendon structure changes, it is not capable of doing the work it should and this causes you more pain. If you do not decrease the burden on your Achilles tendon and allow it to rest, further damage will occur and it can now lead to problems elsewhere, like the knee, hip and lower back.
3. Degenerative tendonitis (Final Stage)
Degenerative tendonitis is the final stage and at this stage there is a poor prognosis for the tendon. The degeneration of the tendon are now irreversible. The structure of the Achilles tendon weakens further. Adhesions form between the tendon and the sheath around it. These adhesions are patches of wound tissue that attempts to heal the torn fibers. The adhesions, together with the fact that the tendon thickens, makes the tendon less flexible. The normal gliding movement of the tendon inside the sheath becomes impossible.
Now, the tendon is able to carry even less load. Leaving you in pain with simple daily activities. This phase of tendonitis usually bothers older people who has had underlying and ongoing Achilles tendon problems, or younger people who has continued to overload the tendon.
Diagnosis of Achilles tendonitis
Physiotherapy evaluation
Our physiotherapists are able to accurately diagnose your Achilles tendonitis without expensive scans. We know and understand the anatomy of the lower leg, foot and ankle and we know which other soft tissue structures could be involved with Achilles tendonitis. We consider the the intricacy of the biomechanics of walking, running and jumping.
Different factors will contribute to each patient’s Achilles tendon pain. Therefore we look at the bigger picture. We look at what is important to you and what you would like to achieve with your training. During your physiotherapy evaluation, we will be able to determine how bad your Achilles tendonitis is by stretching and stressing the tendon as well as different joints and muscles in the area. We also test muscle strength and length, range of movement and can measure swelling in the area. This is why our physiotherapists are the best at diagnosing this type of problem.
X-rays
If your physiotherapist feels that it’s necessary to refer you for X-rays it will be discussed with you. X-rays can be helpful to exclude fractures of any bones in and around your foot and ankle, but will not show evidence of Achilles tendonitis.
Children have softer bones and are still growing. In a child, the Achilles tendon anchors onto the heel bone and onto a growth plate. This means that continuous strain and tension of the Achilles tendon on the growth plate of the heel bone can cause pain, inflammation and damage to the growth plate itself. In this case, taking an x-ray will be an option.
Ultrasound (diagnostic)
This is the preferred test to use to confirm that you have Achilles tendonitis. Diagnostic ultrasound will show thickening of the tendon as well as areas of swelling around the tendon. An ultrasound will be enough to confirm your diagnosis.
MRI
Doing an MRI or even a CT scan to confirm Achilles tendonitis is expensive and unnecessary. However, it can be useful to exclude other conditions. You can only get an MRI done, if you are referred by a specialist. If your physiotherapist feels it is necessary to refer you to a specialist, it will be discussed with you.
Why is my Achilles tendon pain not going away?
Treatment for Achilles tendonitis is something that can take a very long time. It will feel like your pain takes a long time to improve. Tendons heal a lot slower than other structures and Achilles tendonitis is a type of injury where you will need to change your routine. Tendons don’t like sudden changes to the amount of load they have to carry.
By increasing the distance that you are walking or running, you are increasing the amount of work that your Achilles tendon must do. Increasing your speed, changing your shoes or even changing your route to run uphill more often, are all things that increase the load on your Achilles tendon. Pushing through the pain that has developed in your heel is not the way to go. It will feel like your pain is improving when you move. Only to come back after training or the next morning.
The only way to address this issue is a change in the load that your Achilles tendon must carry. That means that you must decrease your distance or speed or that you might have to do another form of exercise to let your Achilles tendon rest.
You can create a cycle of damage if you constantly overload or overuse the tendon before it heals. An overused or overloaded Achilles tendon causes pain, inflammation or disintegration of the tendon. It takes a long time to recover from this type of injury, which means early diagnosis is very important. Don’t wait too long before you see a physiotherapist and don’t push through pain each time you move!
What NOT to do when you have Achilles tendonitis
What you SHOULD do when you have Achilles tendonitis
What makes Achilles tendonitis worse?
A big problem we see these days with Achilles tendonitis
A common problem we see is that patients wait too long before they seek help for their Achilles tendon pain. By the time patients come to see us, they have had Achilles tendon pain for 6 months to a year and they continued training. Now, the tendon structure has already started to change and weaken, leading to recovery taking so much longer.
Often, patients try to take anti-inflammatory medication in the hopes of decreasing their pain. This, however, only slows the process of healing. And tendons already heal a lot slower than other structures. The only long-term solution for your pain is to change the load that you put on your Achilles tendon. Taking medication will not fix your problem.
The use of an ankle brace or special insoles is another problem we see. An ankle brace will support your ankle and foot, which might help you to feel better when you walk or exercise. However, long-term use of a brace like this will only lead to you getting used to and dependent on the brace. It will lead to the joints and muscles in and around your foot and ankle to become very stiff and weak. This in turn will lead to a few other problems and only increase your recovery time. The same can be said about insoles. Be careful to change your shoes and get insoles too quickly. It will change the biomechanical way that your foot and ankle moves when you walk or exercise. This can put strain on other structures and lead to more pain.
Physiotherapy treatment of Achilles tendonitis
We have seen many patients with Achilles tendonitis, and we can provide the best possible treatment for Achilles tendon pain, that leads to faster recovery. Physios understand that patients are often anxious to get back to their normal activities, so that is why we are here to provide guidance and answers. We can implement a very effective and structured plan of action that treats all the aspects of the problem and get you back on to where you want to be living your best life. However, it’s important that you commit to the treatment plan for your Achilles tendonitis, as this improves your chances of successful long-term recovery.
The basic structure of our treatments:
- Determine what is injured
- How bad is it injured?
- Protect it from further injury
- Give it time to heal
- Strengthen surrounding muscles
- Re-evaluate to monitor progress
We will be looking at different aspects like testing and measuring the ability of the Achilles tendon to take load. However, we will also look at other aspects like muscle strength, range of motion, flexibility and stability. Treatment techniques will include: soft tissue massage, joint mobilisations, dry needling, strapping, laser therapy, nerve mobilisations and guiding you through a rehabilitation program of gradual strengthening, lengthening and conditioning of the tendon.
Your best bet would be to come and see us for comprehensive rehabilitation. We work on all the phases of healing until we can get you back to where you were before your injury.
Phases of rehabilitation
1st Phase: Protection & initial Healing
Protect
We have found that patients tend to continue walking on the injured leg with a limp. The tendon still carries the load every time that you put weight onto your leg. Depending on the severity of your condition, it is better to take some weight off your affected leg. Possibly by using crutches.
Rest
Rest from activities that is worsening your pain.
Reduce the load that your Achilles tendon must handle.
As soon as there’s no pain, don’t test it. Give it time to heal.
Ice
If there is a severe inflammatory reaction and the area around your Achilles tendon feels tender to touch or even slightly swollen, ice can be something to manage your pain. Ice will numb the pain and could help to manage swelling. Always keep a towel between the ice and your skin (to prevent freeze burn).
Compress
Use strapping or an elastic compression bandage to keep your foot supported. This will assist in managing your pain and control swelling.
Elevate
If your foot is slightly swollen, elevation can assist to control swelling and allowing you to rest. Lie on your back with your foot on a chair (your calf must be higher than your heart to allow gravity to assist in draining the fluid).
2nd Phase: Establish pain free range of movement
During your examination and tests, it’ll become clear what you’ll be able to do, and what you should avoid. We identify factors that contribute to cause your pain, specific to your case. There is a pain free range of movement that you’re safe to move within, and our exercises will be targeted between these boundaries. On completion of this phase you should be able to perform movements within limits of your pain.
As your Achilles tendonitis treatment plan progresses, we aim to gain a larger pain free range of movement while your painful range becomes less intense.
3d Phase: Tissue healing
During this phase of your Achilles tendonitis treatment, we monitor the progress of your pathology and track the fibrous tissue formation and scar tissue healing of your Achilles tendon. On a cellular level we’re able to accelerate tissue healing using dry needling, laser, ultrasoundand electrotherapy.
4th Phase: Tissue Stress & ability to heal
During each session we will re-evaluate to see if you are achieving the necessary targets as part of the Achilles tendonitis treatment plan. This way we will know if your Achilles tendon is be able to handle tensile, elastic and compression forces. We use isometric muscle contractions. These are muscle contractions without movement to keep the surrounding muscles active without compromising your Achilles tendon with too much load.
5th Phase: Muscle Strength & Full Range of Movement
The most important component of rehabilitation is to regain full range of movement of the muscle fibers of your calf muscles. The scar tissue that form inside the Achilles tendon must be lengthened and orientated to allow it to move without any restrictions. We use massage, stretches and neurodynamic mobilizations to achieve full range of movement.
On completion of this phase of your Achilles tendonitis treatment, you should be able to point and flex your foot without any restriction.
6th Phase: Eccentric Muscle Strength
Its common to feel some pain when you start to put more load on your Achilles tendon again. This is due to the breaking down of abnormal fibrous tissue adhesions that restrict the Achilles tendon to glide freely. And tightness in your calf muscles will also restrict the Achilles tendon from moving freely. A muscle contraction works in two directions: One where the calf muscle is contracted and it shortens like a heel rise (concentric), and controlling the movement when you drop your heel down (eccentric). Eccentric exercises are vital for conditioning the muscle fibers and Achilles tendon to absorb forces.
During this phase of your Achilles tendonitis treatment you should be able to control movements of your foot and contraction of the surrounding muscles, in all directions.
7th Phase: Concentric Muscle Strength
Shortening of the muscle during a contraction involves strength and power exercises that will be progressed gradually as your healing takes place. Your physiotherapist will monitor your Achilles tendon’s reaction to normal forces like walking, climbing stairs and driving.
When you have completed this phase of your Achilles tendonitis treatment, you should be able to point your toes against resistance, like walking on your toes.
8th Phase: Testing for return to activity
In this phase of your Achilles tendonitis treatment we will gradually help to build you back up to be able to cope with the intensity of normal activities and training. This is important for your Achilles tendon to be able to withstand repetitive loading without flare-ups. Your physiotherapist will guide you to re-engage in activities in safe increments, and adjust where necessary. We’ll follow your progress and adapt your treatment plan where needed.
9th Phase: High Speed, Power, Proprioception
Your Achilles tendon must be tested under high load and speed to ensure that it is able to keep up with the demand of your body. During this phase, your physiotherapist will guide you to return to your normal activities, which includes challenging your tendon past its ‘normal’ boundaries to determine how it reacts to different forces. Ultimately, this part of your Achilles tendonitis treatment will prepare you to return to participating in your sport.
Whatever must be done – we’ll get you there. Jumps, Landing, Sprints, and much more.
10th Phase: Sport Specific Training
This is the final stage of rehabilitation. Your physiotherapist will still commence with myofascial release, trigger point release and electrotherapy modalities where needed, but functional rehabilitation is most important during this phase.
Depending on your sport, your physiotherapist will tailor specific exercises that will help strengthen you for your specific sport. A successful outcome of this phase of Achilles tendonitis treatment, is when you have gained knowledge throughout the rehabilitation program and can participate at full power and speed, not to mention the benefits of minimizing your chance of future injury.
How long will it take for my Achilles tendonitis to improve?
If you keep in mind the slow healing rate of tendons, then you can plan on physiotherapy treatment for Achilles tendonitis taking anything between 6 weeks to 3 months. Every patient is different and will have different goals. You could experience flare ups in between, but if the full rehabilitation program is followed, we aim to get you back as soon as possible.
The first few weeks, while dealing with the acute phase, we will focus on pain management and healing and then we will progress to gradual tendon loading, and finally rehabilitation. For the first week or two you will need two physiotherapy treatments per week. Thereafter, your treatments will be spread out to once a week. You will have time in between to continue with your rehabilitation program.
Other medical treatments for Achilles tendonitis
- Medication can be used for treatment of your Achilles tendonitis, but long term use of anti-inflammatory medication is not advised as it slows down healing.
- Cortisone injections will not be the solution to your problem. Initially, you might be given a cortisone injection by a doctor for treatment of your Achilles tendonitis. This could help with pain and inflammation and give you some relief. However, cortisone is not good for joint and tendon integrity in the long run.
- Getting an alignment done to improve the way you run or walk will not be the solution or the right form of treatment for your Achilles tendonitis. A sudden pulling movement like this could damage your already weakened Achilles tendon.
- Seeing a biokineticist is not a bad idea. However, in the initial stages of treatment for your Achilles tendonitis, you will need to be seen by a physiotherapist first. Your physiotherapist will then refer you to an appropriate biokineticist when you are ready to progress to the final stages of your rehabilitation program.
Is surgery an option for Achilles tendonitis?
If your pain continues without reason and your physiotherapist is worried that something else is wrong, you will be referred to the appropriate specialist. Generally, surgery is not really something to consider with Achilles tendonitis. There is a minimally invasive technique called ‘Tendon stripping’ that could be done by an orthopaedic surgeon. Adhesions formed between the tendon and the surrounding sheath are ‘stripped’ or scraped away. This could improve Achilles tendon pain, because the tendon can now move more freely.
Weighing up surgery and conservative treatment of your Achilles tendonitis is something to think about. A surgical technique could relieve pain in your Achilles tendon, but with physiotherapy and the right rehab, you will improve not only your pain, but any contributing factors to your pain will also be addressed. Surgery will address the symptoms that you feel now. Whereas, your physiotherapist will help you to take a step back and look at the bigger picture. Addressing all the problems and weaknesses that cause your Achilles tendonitis to come back time after time is the best long-term solution.
What else could it be?
Plantar fasciitis – Pain at the bottom of your heel or pain stretching over the arch of your foot. It is especially painful when taking the first few steps in the morning.
Haglund deformity – A prominent bony point at the back of your heel bone (calcaneus) that feels especially painful and irritated when you wear tight shoes that rub against the back of your heel.
Sever’s disease – A common cause of heel pain in growing children and adolescents. It is inflammation of the growth plate at the back of the heel bone due to repeated stress and tension of the achilles tendon on the heel bone.
Calcaneal fracture or stress fracture – It is a hairline crack or fracture of the heel bone (calcaneus). It usually happens due to overuse (like marching) or a hard fall directly onto the heel. Walking, marching or running will be painful.
Heel fat pad syndrome – Deep, bruise-like pain in the center of the heel. Usually due to changes to the fat pad in the heel. The fat pad can become worn and thin or painful and inflamed. It is especially painful when you put pressure on the heel, walking or stepping on your heel specifically.
DVT (deep vein thrombosis) – Pain, redness, throbbing and swelling in your calf due to a blood clot in the area. Especially worse when you try to flex your foot (trying to pull up your toes toward you) or when you try to step on your leg.
Joint Causes
Posterior ankle impingement – Pain at the back of your ankle or heel due to compression of the bones, joints and soft tissue structures. Compression like this happens during repeated and forceful plantarflexion (pointing your toes). It often affects ballet dancers.
Ankle arthritis – Pain and stiffness of your ankle and foot. Your pain feels especially worse in cold weather, after resting and after walking far. Arthritis can affect any of the many joints around your foot and ankle.
Nerve causes
Tarsal tunnel syndrome (posterior tibial nerve impingement) – Ankle and heel pain due to a compressed nerve. It usually happens due to an injury or previous injury that causes irritation or compression to the nerve. You will feel burning pain around your foot that worsens when you are standing or moving your ankle and foot.
Referred pain from your lower back – Pain in your leg, heel and foot that seems to spread from your lower back. Usually you will feel symptoms like pain or stiffness in your back as well. The spreading pain usually worsens when you sit or bend forward. It can also include symptoms like burning, numbness or pins and needles.
Partial or complete achilles tendon tear – A sudden, sharp pain or even snapping sound that you feel at the back of your heel. The achiles tendon can tear (or even tear only partially) during sports, sprinting or even walking. You won’t be able to lift your foot up when you walk or point your toes.
Achiles tendonitis can also be known as:
- Achilles tendinitis
- Pulled Calf muscle
- Stiff Achilles
- Achilles tendinopathy